-
PDF
- Split View
-
Views
-
Cite
Cite
Bellis van den Berg, Linda Grievink, Joris Yzermans, Erik Lebret, Medically Unexplained Physical Symptoms in the Aftermath of Disasters, Epidemiologic Reviews, Volume 27, Issue 1, July 2005, Pages 92–106, https://doi.org/10.1093/epirev/mxi001
Close - Share Icon Share
INTRODUCTION
Many studies have examined the health problems among survivors of disasters, showing that the most frequently reported symptoms after disasters are mental health problems, such as posttraumatic stress symptoms, depression, and anxiety (1, 2).
In the last decade, the Netherlands was struck by a few national disasters. On October 4, 1992, an El Al Boeing 747 airplane crashed into two apartment buildings in an Amsterdam suburb. Six years after the airplane crash, a study of the health effects of the crash was conducted. This study showed that, in addition to mental health problems, physical symptoms were very prevalent among the survivors of the plane crash (3, 4). On May 13, 2000, a fireworks depot exploded in a residential area of the city of Enschede. The explosions and subsequent fire killed 22 people and injured over 900 people, and about 500 homes were severely damaged or destroyed. The Dutch government declared this a national disaster, and the Ministry of Health, Welfare, and Sports decided to launch a study into the health effects of this disaster. This study showed that a substantial proportion of those who were affected by the fireworks disaster suffered from physical symptoms, such as headache, fatigue, and pain in the stomach, chest, joints, and muscles (5, 6). These symptoms are often labeled as medically unexplained physical symptoms (MUPS), but other labels, such as psychosomatic symptoms or functional somatic syndromes, have been given as well (7).
Survivors of disasters may attribute these physical symptoms to (suspected) exposure to toxic substances, and this may lead to social unrest and amplification of the health problems (8, 9). For example, after the Bijlmermeer airplane crash in Amsterdam, many survivors reported health symptoms that they attributed to possible toxic exposures, such as depleted uranium (3). General practitioners, however, associated only a small proportion (about 20 percent) of the most frequently reported symptoms with a diagnosis, and thus the majority of symptoms were unexplained (4).
In the nontraumatized general population, MUPS are also very common, with reported prevalence rates ranging from 5 to 35 percent (10, 11). The majority of these symptoms cannot be explained by a medical diagnosis; general population studies have shown that the etiology of 30–75 percent of such symptoms as headache, fatigue, and stomachache is unknown (10, 12, 13).
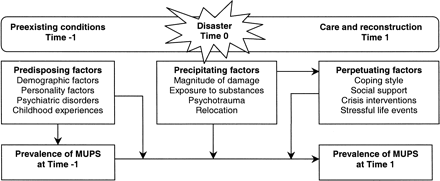
After disasters, the prevalence rates of MUPS seem to increase. However, since many but not all survivors develop these symptoms, the question arises as to which factors predict who will or will not develop MUPS. Mayou and Farmer (14) divided risk factors into three categories: predisposing, precipitating, and perpetuating factors (which we call the “3-P model”). Predisposing factors are factors that already exist before the disaster took place, such as certain demographic characteristics and personality factors. Precipitating factors are directly related to the disaster, for example, injury, relocation, fear, and loss of property. These factors might increase the proportion of survivors that develops MUPS. After the disaster, perpetuating factors, for example, the coping style of the survivor and lack of social support, are factors that might maintain or exacerbate the symptoms (figure 1).
Predisposing, precipitating, and perpetuating factors for medically unexplained physical symptoms (MUPS).
Since MUPS are associated with impaired emotional and physical functioning (15, 16), it is useful to identify risk factors that clinicians can use for early screening of MUPS after disasters. More insight into the prevalence rates of and risk factors for MUPS may help clinicians and policy makers to predict symptom outcomes and to optimize aftercare. To get more insight into the prevalence rate of and risk factors for MUPS after disasters, we reviewed the literature that was published in the last two decades. There are two central questions in this review: 1) What is the prevalence rate of MUPS among survivors of disasters at different points in time? and 2) which factors are associated with MUPS among survivors of disasters?
METHOD
To answer these questions, we reviewed the literature that was published between January 1983 and December 2003. We searched the electronic databases PubMed (US National Library of Medicine, Bethesda, Maryland), PsychInfo (American Psychological Association, Washington, DC), Embase (Elsevier B.V., Amsterdam, the Netherlands), Biosis (The Thomson Corporation, Stamford, Connecticut), Psyndex (German Institute of Medical Documentation and Information, Cologne, Germany), and SciSearch (Institute for Scientific Information, The Thomson Corporation, Stamford, Connecticut) without any language restriction. The keywords that were used in the searches are shown in table 1. We extended the search by examining the bibliographies of identified review articles and by searching private databases that were available at different research institutes in the Netherlands.
Key search terms
Symptoms | Medically unexplained symptom* (MUS), medically unexplained physical symptom* (MUPS), somatic disorder*, psychosomatic symptom*, psychosomatic complaint*, somatic symptom*, somatic complaint*, physical symptom*, physical complaint*, somatization, functional somatic symptom*, stress disorder*, posttraumatic stress disorder*, signs and symptoms, distress, morbidity, health, stress |
| AND | |
| Disaster | Disaster*, life event*, traumatic event*, environ mental exposure, NOT disaster planning |
| AND | |
| Design | Cross-sectional, prospective, case-control, cohort, causality, risk, determinant*, predict* |
Symptoms | Medically unexplained symptom* (MUS), medically unexplained physical symptom* (MUPS), somatic disorder*, psychosomatic symptom*, psychosomatic complaint*, somatic symptom*, somatic complaint*, physical symptom*, physical complaint*, somatization, functional somatic symptom*, stress disorder*, posttraumatic stress disorder*, signs and symptoms, distress, morbidity, health, stress |
| AND | |
| Disaster | Disaster*, life event*, traumatic event*, environ mental exposure, NOT disaster planning |
| AND | |
| Design | Cross-sectional, prospective, case-control, cohort, causality, risk, determinant*, predict* |
An asterisk was placed at the end of some words to search for all terms that begin with that word.
Key search terms
Symptoms | Medically unexplained symptom* (MUS), medically unexplained physical symptom* (MUPS), somatic disorder*, psychosomatic symptom*, psychosomatic complaint*, somatic symptom*, somatic complaint*, physical symptom*, physical complaint*, somatization, functional somatic symptom*, stress disorder*, posttraumatic stress disorder*, signs and symptoms, distress, morbidity, health, stress |
| AND | |
| Disaster | Disaster*, life event*, traumatic event*, environ mental exposure, NOT disaster planning |
| AND | |
| Design | Cross-sectional, prospective, case-control, cohort, causality, risk, determinant*, predict* |
Symptoms | Medically unexplained symptom* (MUS), medically unexplained physical symptom* (MUPS), somatic disorder*, psychosomatic symptom*, psychosomatic complaint*, somatic symptom*, somatic complaint*, physical symptom*, physical complaint*, somatization, functional somatic symptom*, stress disorder*, posttraumatic stress disorder*, signs and symptoms, distress, morbidity, health, stress |
| AND | |
| Disaster | Disaster*, life event*, traumatic event*, environ mental exposure, NOT disaster planning |
| AND | |
| Design | Cross-sectional, prospective, case-control, cohort, causality, risk, determinant*, predict* |
An asterisk was placed at the end of some words to search for all terms that begin with that word.
For the selection of the papers, we used four inclusion criteria: a disaster criterion, a subject criterion, a MUPS criterion, and a report criterion. A disaster was defined as a collective stressful experience with a sudden onset. With this definition, publications about natural disasters (e.g., hurricanes, volcanic eruptions) and man-made disasters (e.g., Three Mile Island accident, aircraft disasters) were included, while studies examining survivors of individual traumatic events, such as sexual assault and traffic accidents, were excluded. Although war situations are traumatic and stressful as well, studies about war veterans, survivors of wars, and refugees were excluded because the threat of war and the intention to harm make wartime exposure different from disaster exposure. Subjects had to be directly exposed to the disaster themselves (subject criterion). People with close family and personal ties to the primary victims and people whose occupations require them to respond to the disaster, such as relief workers, were excluded. Relief workers were omitted because they are mostly healthy young men who are selected on the basis of their physical and emotional functioning. In addition, most relief workers are trained to cope with stressful situations, and therefore they may react differently from citizens. The MUPS criterion implied that one or more symptoms from a MUPS cluster, based on the International Classification of Primary Care as developed by one of the authors (J. Y.), had to be measured (table 2). These symptoms could be measured by self-constructed questionnaires or by validated scales, such as the Symptom Checklist (SCL-90). Although a medical disorder cannot be ruled out for these symptoms, an increase at the population level of these symptoms among survivors of disasters, compared with levels that are found in the general population or a control group, may be assumed to be disaster related. In addition, studies reporting symptoms that were clearly the result of exposure to toxic substances, for example, eye irritation and respiratory symptoms after the Bhopal gas leak (17), were excluded from this review. To examine prevalence rates of MUPS among survivors of disasters, we included different types of studies (report criterion). First, we included studies that reported percentages of MUPS among survivors of disasters. Second, we included studies that reported about a percentage of survivors scoring above a standardized cutoff score. Since cutoff scores are based on scores in a normative population (e.g., those with a score above the 90th percentile have a high score), a control group was not required for these studies. Third, studies were included that reported a mean score on a MUPS scale. For these studies, a control group was required to compare the mean score of survivors with that of control subjects. In addition to these studies that reported about the prevalence of MUPS, we also included studies that did not report about prevalence rates but that did report about risk factors for MUPS.
Medically unexplained physical symptom cluster based on the International Classification of Primary Care
Pain general/multiple sites | Swollen ankles/edema | Disturbance smell/taste |
| Chills | Neck symptoms/complaints | Vertigo/dizziness |
| Weakness/tiredness general | Back symptoms/complaints | Neurologic symptom/complaint other neurologic system |
| Feeling ill | Low back symptoms/complaints without radiation | Pain respiratory system |
| Fainting/syncope | Chest symptom/complaint | Shortness of breath/dyspnea |
| Swelling | Back symptom/complaint | Wheezing |
| Sweating problem | Low back symptom/complaint | Breathing problem, other |
| Abdominal pain/cramps general | Chest symptom/complaint | Cough |
| Abdominal pain epigastric | Flank/axilla symptom/complaint | Sneezing/nasal congestion |
| Heartburn | Jaw symptom/complaint | Nose symptom/complaint other |
| Rectal/anal pain | Shoulder symptom/complaint | Sinus symptom/complaint |
| Perianal itching | Arm symptom/complaint | Throat symptom/complaint |
| Abdominal pain localized other | Elbow symptom/complaint | Tonsils symptom/complaint |
| Flatulence/gas/belching | Wrist symptom/complaint | Voice symptom/complaint |
| Nausea | Hand/finger symptom/complaint | Respiratory symptom/complaint other respiratory system |
| Vomiting | Hip symptom/complaint | Pain/tenderness of skin |
| Diarrhea | Leg/thigh symptom/complaint | Pruritus |
| Constipation | Knee symptom/complaint | Skin symptom/complaint other |
| Abdominal distention | Ankle symptom/complaint | Excessive thirst |
| Digestive symptoms/complaints on other digestive organs | Foot and toe symptom/complaint | Excessive appetite |
| Eye sensation abnormal | Muscle pain | Loss of appetite |
| Tinnitus/ringing/buzzing ears | Muscle symptom/complaint, not otherwise specified | Dysuria/painful urination |
| Heart pain | Joint symptoms/complaint | Urinary frequency/urgency |
| Pressure/tightness of heart | Headache | Genital pain female |
| Cardiovascular pain, not otherwise specified | Tension headache | Menstrual pain |
| Palpitations/awareness of heart | Pain face | Pain in penis |
| Irregular heartbeat, other | Restless legs | Pain in testis/scrotum |
| Prominent veins | Tingling fingers/feet/toes |
Pain general/multiple sites | Swollen ankles/edema | Disturbance smell/taste |
| Chills | Neck symptoms/complaints | Vertigo/dizziness |
| Weakness/tiredness general | Back symptoms/complaints | Neurologic symptom/complaint other neurologic system |
| Feeling ill | Low back symptoms/complaints without radiation | Pain respiratory system |
| Fainting/syncope | Chest symptom/complaint | Shortness of breath/dyspnea |
| Swelling | Back symptom/complaint | Wheezing |
| Sweating problem | Low back symptom/complaint | Breathing problem, other |
| Abdominal pain/cramps general | Chest symptom/complaint | Cough |
| Abdominal pain epigastric | Flank/axilla symptom/complaint | Sneezing/nasal congestion |
| Heartburn | Jaw symptom/complaint | Nose symptom/complaint other |
| Rectal/anal pain | Shoulder symptom/complaint | Sinus symptom/complaint |
| Perianal itching | Arm symptom/complaint | Throat symptom/complaint |
| Abdominal pain localized other | Elbow symptom/complaint | Tonsils symptom/complaint |
| Flatulence/gas/belching | Wrist symptom/complaint | Voice symptom/complaint |
| Nausea | Hand/finger symptom/complaint | Respiratory symptom/complaint other respiratory system |
| Vomiting | Hip symptom/complaint | Pain/tenderness of skin |
| Diarrhea | Leg/thigh symptom/complaint | Pruritus |
| Constipation | Knee symptom/complaint | Skin symptom/complaint other |
| Abdominal distention | Ankle symptom/complaint | Excessive thirst |
| Digestive symptoms/complaints on other digestive organs | Foot and toe symptom/complaint | Excessive appetite |
| Eye sensation abnormal | Muscle pain | Loss of appetite |
| Tinnitus/ringing/buzzing ears | Muscle symptom/complaint, not otherwise specified | Dysuria/painful urination |
| Heart pain | Joint symptoms/complaint | Urinary frequency/urgency |
| Pressure/tightness of heart | Headache | Genital pain female |
| Cardiovascular pain, not otherwise specified | Tension headache | Menstrual pain |
| Palpitations/awareness of heart | Pain face | Pain in penis |
| Irregular heartbeat, other | Restless legs | Pain in testis/scrotum |
| Prominent veins | Tingling fingers/feet/toes |
Medically unexplained physical symptom cluster based on the International Classification of Primary Care
Pain general/multiple sites | Swollen ankles/edema | Disturbance smell/taste |
| Chills | Neck symptoms/complaints | Vertigo/dizziness |
| Weakness/tiredness general | Back symptoms/complaints | Neurologic symptom/complaint other neurologic system |
| Feeling ill | Low back symptoms/complaints without radiation | Pain respiratory system |
| Fainting/syncope | Chest symptom/complaint | Shortness of breath/dyspnea |
| Swelling | Back symptom/complaint | Wheezing |
| Sweating problem | Low back symptom/complaint | Breathing problem, other |
| Abdominal pain/cramps general | Chest symptom/complaint | Cough |
| Abdominal pain epigastric | Flank/axilla symptom/complaint | Sneezing/nasal congestion |
| Heartburn | Jaw symptom/complaint | Nose symptom/complaint other |
| Rectal/anal pain | Shoulder symptom/complaint | Sinus symptom/complaint |
| Perianal itching | Arm symptom/complaint | Throat symptom/complaint |
| Abdominal pain localized other | Elbow symptom/complaint | Tonsils symptom/complaint |
| Flatulence/gas/belching | Wrist symptom/complaint | Voice symptom/complaint |
| Nausea | Hand/finger symptom/complaint | Respiratory symptom/complaint other respiratory system |
| Vomiting | Hip symptom/complaint | Pain/tenderness of skin |
| Diarrhea | Leg/thigh symptom/complaint | Pruritus |
| Constipation | Knee symptom/complaint | Skin symptom/complaint other |
| Abdominal distention | Ankle symptom/complaint | Excessive thirst |
| Digestive symptoms/complaints on other digestive organs | Foot and toe symptom/complaint | Excessive appetite |
| Eye sensation abnormal | Muscle pain | Loss of appetite |
| Tinnitus/ringing/buzzing ears | Muscle symptom/complaint, not otherwise specified | Dysuria/painful urination |
| Heart pain | Joint symptoms/complaint | Urinary frequency/urgency |
| Pressure/tightness of heart | Headache | Genital pain female |
| Cardiovascular pain, not otherwise specified | Tension headache | Menstrual pain |
| Palpitations/awareness of heart | Pain face | Pain in penis |
| Irregular heartbeat, other | Restless legs | Pain in testis/scrotum |
| Prominent veins | Tingling fingers/feet/toes |
Pain general/multiple sites | Swollen ankles/edema | Disturbance smell/taste |
| Chills | Neck symptoms/complaints | Vertigo/dizziness |
| Weakness/tiredness general | Back symptoms/complaints | Neurologic symptom/complaint other neurologic system |
| Feeling ill | Low back symptoms/complaints without radiation | Pain respiratory system |
| Fainting/syncope | Chest symptom/complaint | Shortness of breath/dyspnea |
| Swelling | Back symptom/complaint | Wheezing |
| Sweating problem | Low back symptom/complaint | Breathing problem, other |
| Abdominal pain/cramps general | Chest symptom/complaint | Cough |
| Abdominal pain epigastric | Flank/axilla symptom/complaint | Sneezing/nasal congestion |
| Heartburn | Jaw symptom/complaint | Nose symptom/complaint other |
| Rectal/anal pain | Shoulder symptom/complaint | Sinus symptom/complaint |
| Perianal itching | Arm symptom/complaint | Throat symptom/complaint |
| Abdominal pain localized other | Elbow symptom/complaint | Tonsils symptom/complaint |
| Flatulence/gas/belching | Wrist symptom/complaint | Voice symptom/complaint |
| Nausea | Hand/finger symptom/complaint | Respiratory symptom/complaint other respiratory system |
| Vomiting | Hip symptom/complaint | Pain/tenderness of skin |
| Diarrhea | Leg/thigh symptom/complaint | Pruritus |
| Constipation | Knee symptom/complaint | Skin symptom/complaint other |
| Abdominal distention | Ankle symptom/complaint | Excessive thirst |
| Digestive symptoms/complaints on other digestive organs | Foot and toe symptom/complaint | Excessive appetite |
| Eye sensation abnormal | Muscle pain | Loss of appetite |
| Tinnitus/ringing/buzzing ears | Muscle symptom/complaint, not otherwise specified | Dysuria/painful urination |
| Heart pain | Joint symptoms/complaint | Urinary frequency/urgency |
| Pressure/tightness of heart | Headache | Genital pain female |
| Cardiovascular pain, not otherwise specified | Tension headache | Menstrual pain |
| Palpitations/awareness of heart | Pain face | Pain in penis |
| Irregular heartbeat, other | Restless legs | Pain in testis/scrotum |
| Prominent veins | Tingling fingers/feet/toes |
The titles and/or abstracts of the identified studies were screened by one of the authors to evaluate whether they met both the disaster criterion and the subject criterion (B. v. d. B.). When there was any doubt about the disaster criterion or the subject criterion, we asked for a full-text version of that study. In addition, we took a random sample of 50 studies that were rejected because of the disaster criterion or the subject criterion to evaluate whether they were indeed not relevant for the review. None of the rejected articles satisfied the criteria. Hard copies of publications that met the disaster criterion and the subject criterion were reviewed by two authors to evaluate whether MUPS was measured (B. v. d. B., L. G.). When there was no consensus between the two authors about the MUPS criterion, a third reviewer did an additional evaluation.
RESULTS
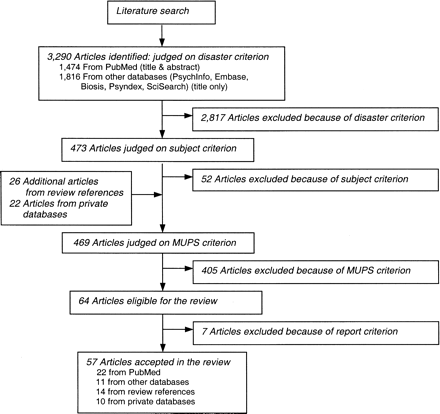
The database searches yielded 3,290 citations: 1,474 from PubMed and 1,816 from the other databases that were searched (figure 2). The citations from PubMed were complete with title and abstract; for the citations from the other databases, only a title was available. In total, 2,817 articles were excluded because they did not meet the disaster criterion, and 52 articles were excluded because of the subject criterion. The search for citations in the bibliographies of identified review articles yielded an additional 26 studies, and 22 eligible articles were found in private databases. We evaluated 469 hard copies with regard to the MUPS criterion (figure 2), of which 32 studies were also evaluated by a third reviewer. Most studies reported only psychological problems among survivors of disasters, such as posttraumatic stress symptoms or anxiety. Sixty-four studies were eligible for the review, of which seven were excluded because of the report criterion. Finally, we accepted 57 studies for this review: 33 cross-sectional studies mostly with a control group and 24 longitudinal studies of which most were retrospective, with four of the latter having a control group. Thirty-seven studies reported about MUPS among survivors of natural disasters, and 20 studies reported about those affected by man-made disasters (table 3). Some study populations were reported in different publications (18–29), but we considered these studies as one study; as a consequence, risk factors examined in these studies will be reported once as well.
Literature search to find articles on medically unexplained physical symptoms (MUPS) among survivors of disasters.
Characteristics and findings of studies examining medically unexplained physical symptoms
First author, year of publication (reference no.) . | Disaster and country . | . | . | . | Time since disaster . | . | . | . | Findings . | . | . | . | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| . | . | No. . | Response rate* (%) . | Measure† . | Predisaster . | <1 month . | 1 month– 1 year . | >1 year . | Prevalence range (%)‡ . | Δ Control group§ . | Δ Time¶ . | Risk factors . | |||||
| Anderson, 1994 (64) | Earthquake, United States | 211 | 90 | SCL-90-R | 24 hours | Yes | |||||||||||
| Bland, 1996 (70) | Earthquake, Italy | 772 | 80 | SCL-90-R | 7 years | Yes | |||||||||||
| Cardena, 1993 (30) | Earthquake, United States | 98 | 20 and 90 | Self- constructed | 1 week | 4 months | Three symptoms: time 1, 30–44; time 2, 13–28 | — | No | ||||||||
| Chen, 2001 (31) | Earthquake, Taiwan | 525 | CHQ-12 | 1 month | Three symptoms: 51–53 | No | |||||||||||
| Karanci, 1995 (58) | Earthquake, Turkey | 461/129# | SCL-40 | 1⅓ years | ND | Yes | |||||||||||
| Kitayama, 2000 (32) | Earthquake, Japan | 258** | Self- constructed | 12 months | 2 years | Three symptoms: time 1, 7–30; time 2, 6–24 | ND | No | |||||||||
| Lima, 1989 (33) | Earthquake, Ecuador | 150 | 100 | SRQ | 3 months | Six symptoms: 17–43 | No | ||||||||||
| Najarian, 2001 (45) | Earthquake, Armenia | 49/25# | SCL-90-R | 2½ years | ++ | Yes | |||||||||||
| Pynoos, 1993 (67) | Earthquake, Armenia | 231** | 100 | CPTSD-RI | 1½ years | Yes | |||||||||||
| Tainaka, 1998 (34) | Earthquake, Japan | 2,555 | 1 week | 3 months | 1½ years | Six symptoms: time 1, 15–89; time 2, 8–76; time 3, 4–49 | Yes | ||||||||||
| Wang, 2000 (43) | Earthquake, China | 335/172# | SCL-90 | 3 and 9 months | ++ | ND | Yes | ||||||||||
| Bravo, 1990 (18); Canino, 1990 (19) | Flood, Puerto Rico | 912 | 93 | DIS/DS | −1 year | 2 years | Yes | ||||||||||
| Cook, 1990 (74) | Flood, United States | 96 | 98 | BSI | 1 week | 1¼, 3, 4, and 5 months | Yes | ||||||||||
| Escobar, 1992 (35) | Flood, Puerto Rico | 375 | DIS/DS | −1 year | 2 years | 12 symptoms: 4–36 | No | ||||||||||
| Melick, 1985 (61) | Flood, United States | 122/45# | SCL-90 | 5 years | — | No | |||||||||||
| Phifer, 1988 (20); Phifer, 1989 (21) | Flood, United States | 222 | 70 | Self- constructed | −3 months | 3 and 9 months | 1¼, 1¾, and 4¼ years | Yes | |||||||||
| Phifer, 1990 (63) | Flood, United States | 222 | 64 | Self- constructed | −1 year | 1½ years | Yes | ||||||||||
| Smith, 1996 (22); Smith, 2000 (23) | Flood, United States | 131 | 27 | PSI | 1½ and 6 months | Yes | |||||||||||
| Solomon, 1987 (59) | Flood, United States | 360/183# | 84 | DIS/DS | 1¼ years | ND | Yes | ||||||||||
| Fairley, 1986 (46) | Hurricane, Fiji | 75/64# | 99 | GHQ and SSI | 2½ months | GHQ: ++; SSI: ++ | Yes | ||||||||||
| Guill, 2001 (36) | Hurricane, Honduras | 110 | Self- constructed | 4 months | Headache: 58 | No | |||||||||||
| Lutgendorf, 1995 (68) | Hurricane, United States | 49 | 58 | CFIDS | 3 months | Yes | |||||||||||
| Shannon, 1994 (65) | Hurricane, United States | 5,687** | RI | 3 months | Above cutoff: 13 | Yes | |||||||||||
| Shaw, 1995 (71) | Hurricane, United States | 106** | TRF | 2 months | 2½ years | Yes | |||||||||||
| Cowan, 1985 (66) | Volcanic eruption, United States | 119 | 85 | SCL-90-R | 12 months | Yes | |||||||||||
| Lima, 1987 (24); Lima, 1993 (25) | Volcanic eruption, Colombia | 113 | SRQ | 7 months | 5 years | Six symptoms: time 1, 20– 60; time 2, 13–36 | — | No | |||||||||
| Murphy, 1984 (26); Murphy, 1988 (27) | Volcanic eruption, United States | 155 | 80 | SCL-90-R | 11 months | 3 years | Yes | ||||||||||
| Clayer, 1985 (37) | Bushfires, Australia | 1,526/100# | 52 | Self- constructed | 12 months | Nerve problems: 30; palpitations: 7 | ++ | No | |||||||||
| Maida, 1989 (38) | Bushfires, United States | 25 | DIS/DS | 3 months | Three symptoms: 8–20 | No | |||||||||||
| McFarlane, 1987 (62) | Bushfires, Australia | 808**/ 734#,** | 43 | RQ | 2 and 8 months | 2¼ years | Above cutoff: time 1, 1; time 2, 5; time 3, 7 | ++ | No | ||||||||
| McFarlane, 1997 (47) | Bushfires, Australia | 1,526/ 1,439†† | 77 | GHQ | 12 months | ++ | Yes | ||||||||||
| Dollinger, 1986 (39) | Lightning strike, United States | 29** | MCBC (expansion) | 2 months | Seven symptoms: 3–31 | No | |||||||||||
| Baum, 1983 (48) | Three Mile Island, United States | 38/83# | 70 | SCL-90 | 1½ years | ++ | No | ||||||||||
| Davidson, 1986 (49) | Three Mile Island, United States | 52/35# | 70 | SCL-90-R | 4⅔ years | ++ | Yes | ||||||||||
| Cleary, 1984 (50) | Three Mile Island, United States | 403/1,506# | Self- constructed | 4 and 10 months | ++ | Yes | |||||||||||
| Prince- Embury, 1988 (51) | Three Mile Island, United States | 108/974†† | 51 | SCL-90-R | 6 years | ++ | No | ||||||||||
| Bromet, 2000 (52) | Chernobyl accident, Ukraine | 300**/ 300** | 92/85‡ | CSI and CBCL | 11 years | CSI: ++; CBCL: ++ | Yes | ||||||||||
| Bromet, 2002 (53) | Chernobyl accident, Ukraine | 300/300# | 92/85‡ | SCL-90-R | 11 years | Above cutoff: 55 | ++ | No | |||||||||
| Cwikel, 1997 (44) | Chernobyl accident, Ukraine | 374/334# | 91 | SCL-90 | 8 and 10 years | ++ | ND | Yes | |||||||||
| Havenaar, 1997 (54) | Chernobyl accident, Ukraine | 265/184# | 92/88‡ | BrSI | 6½ years | Above cutoff: 51 | ++ | No | |||||||||
| Holen, 1990 (28); Holen, 1991 (29) | Industrial disaster, Norway | 73/89# | Self-reported symptoms | 5 weeks | 8 years | ++ | No | ||||||||||
| Weisaeth, 1989 (40) | Industrial disaster, Norway | 246 | 98 | PTSS-30 | 1 and 7 months | Time 2: muscle pain, 5–35; fatigue, 3–33 | Yes | ||||||||||
| Grace, 1993 (60) | Buffalo Creek dam collapse, United States | 199/50# | 39 | PEF and SCL-90-R | 14 years | ND | No | ||||||||||
| Shariat, 1999 (41) | Terrorist attack, United States | 494 | 54 | HSQ | 2⅔ years | Five symptoms: 22–44 | Yes | ||||||||||
| Trout, 2002 (42) | Terrorist attack, United States | 191/155# | 68/47‡ | Self- constructed | 3 months | 12 symptoms: 10–66 | ++ | No | |||||||||
| Yokoyama, 1998 (55) | Terrorist attack, Japan | 18/15# | 12 | POMS | 7 months | ++ | Yes | ||||||||||
| Creamer, 1990 (56) | Multiple, shooting, Australia | 446/338# | 53/57‡ | SCL-90-R | 4 months | ++ | No | ||||||||||
| Chung, 1999 (72) | Aircraft disaster, United Kingdom | 82 | 55 | GHQ | 6 months | Yes | |||||||||||
| Donker, 2002 (4) | Aircraft disaster, the Netherlands | 533 | Self-reported symptoms | 6 years | Six symptoms: 9–45 | No | |||||||||||
| Livingston, 1992 (69) | Aircraft disaster, United Kingdom | 55 | GHQ | 12 months | Yes | ||||||||||||
| Tyano, 1996 (57) | Bus-train collision, Israel | 306/83# | 68/82‡ | SCL-90 | 7 years | ++ | Yes | ||||||||||
First author, year of publication (reference no.) . | Disaster and country . | . | . | . | Time since disaster . | . | . | . | Findings . | . | . | . | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| . | . | No. . | Response rate* (%) . | Measure† . | Predisaster . | <1 month . | 1 month– 1 year . | >1 year . | Prevalence range (%)‡ . | Δ Control group§ . | Δ Time¶ . | Risk factors . | |||||
| Anderson, 1994 (64) | Earthquake, United States | 211 | 90 | SCL-90-R | 24 hours | Yes | |||||||||||
| Bland, 1996 (70) | Earthquake, Italy | 772 | 80 | SCL-90-R | 7 years | Yes | |||||||||||
| Cardena, 1993 (30) | Earthquake, United States | 98 | 20 and 90 | Self- constructed | 1 week | 4 months | Three symptoms: time 1, 30–44; time 2, 13–28 | — | No | ||||||||
| Chen, 2001 (31) | Earthquake, Taiwan | 525 | CHQ-12 | 1 month | Three symptoms: 51–53 | No | |||||||||||
| Karanci, 1995 (58) | Earthquake, Turkey | 461/129# | SCL-40 | 1⅓ years | ND | Yes | |||||||||||
| Kitayama, 2000 (32) | Earthquake, Japan | 258** | Self- constructed | 12 months | 2 years | Three symptoms: time 1, 7–30; time 2, 6–24 | ND | No | |||||||||
| Lima, 1989 (33) | Earthquake, Ecuador | 150 | 100 | SRQ | 3 months | Six symptoms: 17–43 | No | ||||||||||
| Najarian, 2001 (45) | Earthquake, Armenia | 49/25# | SCL-90-R | 2½ years | ++ | Yes | |||||||||||
| Pynoos, 1993 (67) | Earthquake, Armenia | 231** | 100 | CPTSD-RI | 1½ years | Yes | |||||||||||
| Tainaka, 1998 (34) | Earthquake, Japan | 2,555 | 1 week | 3 months | 1½ years | Six symptoms: time 1, 15–89; time 2, 8–76; time 3, 4–49 | Yes | ||||||||||
| Wang, 2000 (43) | Earthquake, China | 335/172# | SCL-90 | 3 and 9 months | ++ | ND | Yes | ||||||||||
| Bravo, 1990 (18); Canino, 1990 (19) | Flood, Puerto Rico | 912 | 93 | DIS/DS | −1 year | 2 years | Yes | ||||||||||
| Cook, 1990 (74) | Flood, United States | 96 | 98 | BSI | 1 week | 1¼, 3, 4, and 5 months | Yes | ||||||||||
| Escobar, 1992 (35) | Flood, Puerto Rico | 375 | DIS/DS | −1 year | 2 years | 12 symptoms: 4–36 | No | ||||||||||
| Melick, 1985 (61) | Flood, United States | 122/45# | SCL-90 | 5 years | — | No | |||||||||||
| Phifer, 1988 (20); Phifer, 1989 (21) | Flood, United States | 222 | 70 | Self- constructed | −3 months | 3 and 9 months | 1¼, 1¾, and 4¼ years | Yes | |||||||||
| Phifer, 1990 (63) | Flood, United States | 222 | 64 | Self- constructed | −1 year | 1½ years | Yes | ||||||||||
| Smith, 1996 (22); Smith, 2000 (23) | Flood, United States | 131 | 27 | PSI | 1½ and 6 months | Yes | |||||||||||
| Solomon, 1987 (59) | Flood, United States | 360/183# | 84 | DIS/DS | 1¼ years | ND | Yes | ||||||||||
| Fairley, 1986 (46) | Hurricane, Fiji | 75/64# | 99 | GHQ and SSI | 2½ months | GHQ: ++; SSI: ++ | Yes | ||||||||||
| Guill, 2001 (36) | Hurricane, Honduras | 110 | Self- constructed | 4 months | Headache: 58 | No | |||||||||||
| Lutgendorf, 1995 (68) | Hurricane, United States | 49 | 58 | CFIDS | 3 months | Yes | |||||||||||
| Shannon, 1994 (65) | Hurricane, United States | 5,687** | RI | 3 months | Above cutoff: 13 | Yes | |||||||||||
| Shaw, 1995 (71) | Hurricane, United States | 106** | TRF | 2 months | 2½ years | Yes | |||||||||||
| Cowan, 1985 (66) | Volcanic eruption, United States | 119 | 85 | SCL-90-R | 12 months | Yes | |||||||||||
| Lima, 1987 (24); Lima, 1993 (25) | Volcanic eruption, Colombia | 113 | SRQ | 7 months | 5 years | Six symptoms: time 1, 20– 60; time 2, 13–36 | — | No | |||||||||
| Murphy, 1984 (26); Murphy, 1988 (27) | Volcanic eruption, United States | 155 | 80 | SCL-90-R | 11 months | 3 years | Yes | ||||||||||
| Clayer, 1985 (37) | Bushfires, Australia | 1,526/100# | 52 | Self- constructed | 12 months | Nerve problems: 30; palpitations: 7 | ++ | No | |||||||||
| Maida, 1989 (38) | Bushfires, United States | 25 | DIS/DS | 3 months | Three symptoms: 8–20 | No | |||||||||||
| McFarlane, 1987 (62) | Bushfires, Australia | 808**/ 734#,** | 43 | RQ | 2 and 8 months | 2¼ years | Above cutoff: time 1, 1; time 2, 5; time 3, 7 | ++ | No | ||||||||
| McFarlane, 1997 (47) | Bushfires, Australia | 1,526/ 1,439†† | 77 | GHQ | 12 months | ++ | Yes | ||||||||||
| Dollinger, 1986 (39) | Lightning strike, United States | 29** | MCBC (expansion) | 2 months | Seven symptoms: 3–31 | No | |||||||||||
| Baum, 1983 (48) | Three Mile Island, United States | 38/83# | 70 | SCL-90 | 1½ years | ++ | No | ||||||||||
| Davidson, 1986 (49) | Three Mile Island, United States | 52/35# | 70 | SCL-90-R | 4⅔ years | ++ | Yes | ||||||||||
| Cleary, 1984 (50) | Three Mile Island, United States | 403/1,506# | Self- constructed | 4 and 10 months | ++ | Yes | |||||||||||
| Prince- Embury, 1988 (51) | Three Mile Island, United States | 108/974†† | 51 | SCL-90-R | 6 years | ++ | No | ||||||||||
| Bromet, 2000 (52) | Chernobyl accident, Ukraine | 300**/ 300** | 92/85‡ | CSI and CBCL | 11 years | CSI: ++; CBCL: ++ | Yes | ||||||||||
| Bromet, 2002 (53) | Chernobyl accident, Ukraine | 300/300# | 92/85‡ | SCL-90-R | 11 years | Above cutoff: 55 | ++ | No | |||||||||
| Cwikel, 1997 (44) | Chernobyl accident, Ukraine | 374/334# | 91 | SCL-90 | 8 and 10 years | ++ | ND | Yes | |||||||||
| Havenaar, 1997 (54) | Chernobyl accident, Ukraine | 265/184# | 92/88‡ | BrSI | 6½ years | Above cutoff: 51 | ++ | No | |||||||||
| Holen, 1990 (28); Holen, 1991 (29) | Industrial disaster, Norway | 73/89# | Self-reported symptoms | 5 weeks | 8 years | ++ | No | ||||||||||
| Weisaeth, 1989 (40) | Industrial disaster, Norway | 246 | 98 | PTSS-30 | 1 and 7 months | Time 2: muscle pain, 5–35; fatigue, 3–33 | Yes | ||||||||||
| Grace, 1993 (60) | Buffalo Creek dam collapse, United States | 199/50# | 39 | PEF and SCL-90-R | 14 years | ND | No | ||||||||||
| Shariat, 1999 (41) | Terrorist attack, United States | 494 | 54 | HSQ | 2⅔ years | Five symptoms: 22–44 | Yes | ||||||||||
| Trout, 2002 (42) | Terrorist attack, United States | 191/155# | 68/47‡ | Self- constructed | 3 months | 12 symptoms: 10–66 | ++ | No | |||||||||
| Yokoyama, 1998 (55) | Terrorist attack, Japan | 18/15# | 12 | POMS | 7 months | ++ | Yes | ||||||||||
| Creamer, 1990 (56) | Multiple, shooting, Australia | 446/338# | 53/57‡ | SCL-90-R | 4 months | ++ | No | ||||||||||
| Chung, 1999 (72) | Aircraft disaster, United Kingdom | 82 | 55 | GHQ | 6 months | Yes | |||||||||||
| Donker, 2002 (4) | Aircraft disaster, the Netherlands | 533 | Self-reported symptoms | 6 years | Six symptoms: 9–45 | No | |||||||||||
| Livingston, 1992 (69) | Aircraft disaster, United Kingdom | 55 | GHQ | 12 months | Yes | ||||||||||||
| Tyano, 1996 (57) | Bus-train collision, Israel | 306/83# | 68/82‡ | SCL-90 | 7 years | ++ | Yes | ||||||||||
Response rates of the first measurement time are reported for longitudinal studies. When response rates of different exposure groups were given, the lowest percentage is reported.
SCL-90 (SCL-90-R/SCL-40), Symptom Checklist somatization subscale; CHQ-12, Chinese Health Questionnaire; SRQ, Self-reporting Questionnaire; CPTSD-RI, Children's Posttraumatic Stress Disorder Reaction Index; DIS/DS, Diagnostic Interview Schedule/Disaster Supplement; BSI, Brief Symptom Inventory; PSI, Physical Symptoms Index; GHQ, General Health Questionnaire; SSI, Somatic Symptom Inventory; CFIDS, chronic fatigue immune dysfunction symptoms; RI, Frederick's Reaction Index for Children; TRF, Teacher's Report Form; RQ, Rutter's Questionnaire (parent and teacher); MCBC, Missouri Children's Behavior Checklist; CSI, Children's Somatization Inventory; CBCL, Child Behavior Checklist; BrSI, Bradford Somatic Inventory; PTSS-30, Posttraumatic Stress Scale 30; PEF, Psychiatric Evaluation Form; HSQ, Health Status Questionnaire; POMS, Profile of Mood States fatigue subscale.
Prevalence range of group of medically unexplained symptoms.
Statistically significant difference in score on scale between survivors and controls; “ND” means there is no difference in reported medically unexplained physical symptoms between survivors and controls, “++” means survivors reported more medically unexplained physical symptoms than did controls, and “—” means survivors reported less medically unexplained physical symptoms than did controls.
Statistically significant difference in reported medically unexplained physical symptoms between two time points; “—” means survivors reported less medically unexplained physical symptoms at the second assessment compared with the first assessment, “ND” means there is no difference in reported medically unexplained physical symptoms between the two assessments, and “++” means survivors reported more medically unexplained physical symptoms at the second assessment compared with the first assessment.
Control group.
Children.
Referent data.
Characteristics and findings of studies examining medically unexplained physical symptoms
First author, year of publication (reference no.) . | Disaster and country . | . | . | . | Time since disaster . | . | . | . | Findings . | . | . | . | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| . | . | No. . | Response rate* (%) . | Measure† . | Predisaster . | <1 month . | 1 month– 1 year . | >1 year . | Prevalence range (%)‡ . | Δ Control group§ . | Δ Time¶ . | Risk factors . | |||||
| Anderson, 1994 (64) | Earthquake, United States | 211 | 90 | SCL-90-R | 24 hours | Yes | |||||||||||
| Bland, 1996 (70) | Earthquake, Italy | 772 | 80 | SCL-90-R | 7 years | Yes | |||||||||||
| Cardena, 1993 (30) | Earthquake, United States | 98 | 20 and 90 | Self- constructed | 1 week | 4 months | Three symptoms: time 1, 30–44; time 2, 13–28 | — | No | ||||||||
| Chen, 2001 (31) | Earthquake, Taiwan | 525 | CHQ-12 | 1 month | Three symptoms: 51–53 | No | |||||||||||
| Karanci, 1995 (58) | Earthquake, Turkey | 461/129# | SCL-40 | 1⅓ years | ND | Yes | |||||||||||
| Kitayama, 2000 (32) | Earthquake, Japan | 258** | Self- constructed | 12 months | 2 years | Three symptoms: time 1, 7–30; time 2, 6–24 | ND | No | |||||||||
| Lima, 1989 (33) | Earthquake, Ecuador | 150 | 100 | SRQ | 3 months | Six symptoms: 17–43 | No | ||||||||||
| Najarian, 2001 (45) | Earthquake, Armenia | 49/25# | SCL-90-R | 2½ years | ++ | Yes | |||||||||||
| Pynoos, 1993 (67) | Earthquake, Armenia | 231** | 100 | CPTSD-RI | 1½ years | Yes | |||||||||||
| Tainaka, 1998 (34) | Earthquake, Japan | 2,555 | 1 week | 3 months | 1½ years | Six symptoms: time 1, 15–89; time 2, 8–76; time 3, 4–49 | Yes | ||||||||||
| Wang, 2000 (43) | Earthquake, China | 335/172# | SCL-90 | 3 and 9 months | ++ | ND | Yes | ||||||||||
| Bravo, 1990 (18); Canino, 1990 (19) | Flood, Puerto Rico | 912 | 93 | DIS/DS | −1 year | 2 years | Yes | ||||||||||
| Cook, 1990 (74) | Flood, United States | 96 | 98 | BSI | 1 week | 1¼, 3, 4, and 5 months | Yes | ||||||||||
| Escobar, 1992 (35) | Flood, Puerto Rico | 375 | DIS/DS | −1 year | 2 years | 12 symptoms: 4–36 | No | ||||||||||
| Melick, 1985 (61) | Flood, United States | 122/45# | SCL-90 | 5 years | — | No | |||||||||||
| Phifer, 1988 (20); Phifer, 1989 (21) | Flood, United States | 222 | 70 | Self- constructed | −3 months | 3 and 9 months | 1¼, 1¾, and 4¼ years | Yes | |||||||||
| Phifer, 1990 (63) | Flood, United States | 222 | 64 | Self- constructed | −1 year | 1½ years | Yes | ||||||||||
| Smith, 1996 (22); Smith, 2000 (23) | Flood, United States | 131 | 27 | PSI | 1½ and 6 months | Yes | |||||||||||
| Solomon, 1987 (59) | Flood, United States | 360/183# | 84 | DIS/DS | 1¼ years | ND | Yes | ||||||||||
| Fairley, 1986 (46) | Hurricane, Fiji | 75/64# | 99 | GHQ and SSI | 2½ months | GHQ: ++; SSI: ++ | Yes | ||||||||||
| Guill, 2001 (36) | Hurricane, Honduras | 110 | Self- constructed | 4 months | Headache: 58 | No | |||||||||||
| Lutgendorf, 1995 (68) | Hurricane, United States | 49 | 58 | CFIDS | 3 months | Yes | |||||||||||
| Shannon, 1994 (65) | Hurricane, United States | 5,687** | RI | 3 months | Above cutoff: 13 | Yes | |||||||||||
| Shaw, 1995 (71) | Hurricane, United States | 106** | TRF | 2 months | 2½ years | Yes | |||||||||||
| Cowan, 1985 (66) | Volcanic eruption, United States | 119 | 85 | SCL-90-R | 12 months | Yes | |||||||||||
| Lima, 1987 (24); Lima, 1993 (25) | Volcanic eruption, Colombia | 113 | SRQ | 7 months | 5 years | Six symptoms: time 1, 20– 60; time 2, 13–36 | — | No | |||||||||
| Murphy, 1984 (26); Murphy, 1988 (27) | Volcanic eruption, United States | 155 | 80 | SCL-90-R | 11 months | 3 years | Yes | ||||||||||
| Clayer, 1985 (37) | Bushfires, Australia | 1,526/100# | 52 | Self- constructed | 12 months | Nerve problems: 30; palpitations: 7 | ++ | No | |||||||||
| Maida, 1989 (38) | Bushfires, United States | 25 | DIS/DS | 3 months | Three symptoms: 8–20 | No | |||||||||||
| McFarlane, 1987 (62) | Bushfires, Australia | 808**/ 734#,** | 43 | RQ | 2 and 8 months | 2¼ years | Above cutoff: time 1, 1; time 2, 5; time 3, 7 | ++ | No | ||||||||
| McFarlane, 1997 (47) | Bushfires, Australia | 1,526/ 1,439†† | 77 | GHQ | 12 months | ++ | Yes | ||||||||||
| Dollinger, 1986 (39) | Lightning strike, United States | 29** | MCBC (expansion) | 2 months | Seven symptoms: 3–31 | No | |||||||||||
| Baum, 1983 (48) | Three Mile Island, United States | 38/83# | 70 | SCL-90 | 1½ years | ++ | No | ||||||||||
| Davidson, 1986 (49) | Three Mile Island, United States | 52/35# | 70 | SCL-90-R | 4⅔ years | ++ | Yes | ||||||||||
| Cleary, 1984 (50) | Three Mile Island, United States | 403/1,506# | Self- constructed | 4 and 10 months | ++ | Yes | |||||||||||
| Prince- Embury, 1988 (51) | Three Mile Island, United States | 108/974†† | 51 | SCL-90-R | 6 years | ++ | No | ||||||||||
| Bromet, 2000 (52) | Chernobyl accident, Ukraine | 300**/ 300** | 92/85‡ | CSI and CBCL | 11 years | CSI: ++; CBCL: ++ | Yes | ||||||||||
| Bromet, 2002 (53) | Chernobyl accident, Ukraine | 300/300# | 92/85‡ | SCL-90-R | 11 years | Above cutoff: 55 | ++ | No | |||||||||
| Cwikel, 1997 (44) | Chernobyl accident, Ukraine | 374/334# | 91 | SCL-90 | 8 and 10 years | ++ | ND | Yes | |||||||||
| Havenaar, 1997 (54) | Chernobyl accident, Ukraine | 265/184# | 92/88‡ | BrSI | 6½ years | Above cutoff: 51 | ++ | No | |||||||||
| Holen, 1990 (28); Holen, 1991 (29) | Industrial disaster, Norway | 73/89# | Self-reported symptoms | 5 weeks | 8 years | ++ | No | ||||||||||
| Weisaeth, 1989 (40) | Industrial disaster, Norway | 246 | 98 | PTSS-30 | 1 and 7 months | Time 2: muscle pain, 5–35; fatigue, 3–33 | Yes | ||||||||||
| Grace, 1993 (60) | Buffalo Creek dam collapse, United States | 199/50# | 39 | PEF and SCL-90-R | 14 years | ND | No | ||||||||||
| Shariat, 1999 (41) | Terrorist attack, United States | 494 | 54 | HSQ | 2⅔ years | Five symptoms: 22–44 | Yes | ||||||||||
| Trout, 2002 (42) | Terrorist attack, United States | 191/155# | 68/47‡ | Self- constructed | 3 months | 12 symptoms: 10–66 | ++ | No | |||||||||
| Yokoyama, 1998 (55) | Terrorist attack, Japan | 18/15# | 12 | POMS | 7 months | ++ | Yes | ||||||||||
| Creamer, 1990 (56) | Multiple, shooting, Australia | 446/338# | 53/57‡ | SCL-90-R | 4 months | ++ | No | ||||||||||
| Chung, 1999 (72) | Aircraft disaster, United Kingdom | 82 | 55 | GHQ | 6 months | Yes | |||||||||||
| Donker, 2002 (4) | Aircraft disaster, the Netherlands | 533 | Self-reported symptoms | 6 years | Six symptoms: 9–45 | No | |||||||||||
| Livingston, 1992 (69) | Aircraft disaster, United Kingdom | 55 | GHQ | 12 months | Yes | ||||||||||||
| Tyano, 1996 (57) | Bus-train collision, Israel | 306/83# | 68/82‡ | SCL-90 | 7 years | ++ | Yes | ||||||||||
First author, year of publication (reference no.) . | Disaster and country . | . | . | . | Time since disaster . | . | . | . | Findings . | . | . | . | |||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| . | . | No. . | Response rate* (%) . | Measure† . | Predisaster . | <1 month . | 1 month– 1 year . | >1 year . | Prevalence range (%)‡ . | Δ Control group§ . | Δ Time¶ . | Risk factors . | |||||
| Anderson, 1994 (64) | Earthquake, United States | 211 | 90 | SCL-90-R | 24 hours | Yes | |||||||||||
| Bland, 1996 (70) | Earthquake, Italy | 772 | 80 | SCL-90-R | 7 years | Yes | |||||||||||
| Cardena, 1993 (30) | Earthquake, United States | 98 | 20 and 90 | Self- constructed | 1 week | 4 months | Three symptoms: time 1, 30–44; time 2, 13–28 | — | No | ||||||||
| Chen, 2001 (31) | Earthquake, Taiwan | 525 | CHQ-12 | 1 month | Three symptoms: 51–53 | No | |||||||||||
| Karanci, 1995 (58) | Earthquake, Turkey | 461/129# | SCL-40 | 1⅓ years | ND | Yes | |||||||||||
| Kitayama, 2000 (32) | Earthquake, Japan | 258** | Self- constructed | 12 months | 2 years | Three symptoms: time 1, 7–30; time 2, 6–24 | ND | No | |||||||||
| Lima, 1989 (33) | Earthquake, Ecuador | 150 | 100 | SRQ | 3 months | Six symptoms: 17–43 | No | ||||||||||
| Najarian, 2001 (45) | Earthquake, Armenia | 49/25# | SCL-90-R | 2½ years | ++ | Yes | |||||||||||
| Pynoos, 1993 (67) | Earthquake, Armenia | 231** | 100 | CPTSD-RI | 1½ years | Yes | |||||||||||
| Tainaka, 1998 (34) | Earthquake, Japan | 2,555 | 1 week | 3 months | 1½ years | Six symptoms: time 1, 15–89; time 2, 8–76; time 3, 4–49 | Yes | ||||||||||
| Wang, 2000 (43) | Earthquake, China | 335/172# | SCL-90 | 3 and 9 months | ++ | ND | Yes | ||||||||||
| Bravo, 1990 (18); Canino, 1990 (19) | Flood, Puerto Rico | 912 | 93 | DIS/DS | −1 year | 2 years | Yes | ||||||||||
| Cook, 1990 (74) | Flood, United States | 96 | 98 | BSI | 1 week | 1¼, 3, 4, and 5 months | Yes | ||||||||||
| Escobar, 1992 (35) | Flood, Puerto Rico | 375 | DIS/DS | −1 year | 2 years | 12 symptoms: 4–36 | No | ||||||||||
| Melick, 1985 (61) | Flood, United States | 122/45# | SCL-90 | 5 years | — | No | |||||||||||
| Phifer, 1988 (20); Phifer, 1989 (21) | Flood, United States | 222 | 70 | Self- constructed | −3 months | 3 and 9 months | 1¼, 1¾, and 4¼ years | Yes | |||||||||
| Phifer, 1990 (63) | Flood, United States | 222 | 64 | Self- constructed | −1 year | 1½ years | Yes | ||||||||||
| Smith, 1996 (22); Smith, 2000 (23) | Flood, United States | 131 | 27 | PSI | 1½ and 6 months | Yes | |||||||||||
| Solomon, 1987 (59) | Flood, United States | 360/183# | 84 | DIS/DS | 1¼ years | ND | Yes | ||||||||||
| Fairley, 1986 (46) | Hurricane, Fiji | 75/64# | 99 | GHQ and SSI | 2½ months | GHQ: ++; SSI: ++ | Yes | ||||||||||
| Guill, 2001 (36) | Hurricane, Honduras | 110 | Self- constructed | 4 months | Headache: 58 | No | |||||||||||
| Lutgendorf, 1995 (68) | Hurricane, United States | 49 | 58 | CFIDS | 3 months | Yes | |||||||||||
| Shannon, 1994 (65) | Hurricane, United States | 5,687** | RI | 3 months | Above cutoff: 13 | Yes | |||||||||||
| Shaw, 1995 (71) | Hurricane, United States | 106** | TRF | 2 months | 2½ years | Yes | |||||||||||
| Cowan, 1985 (66) | Volcanic eruption, United States | 119 | 85 | SCL-90-R | 12 months | Yes | |||||||||||
| Lima, 1987 (24); Lima, 1993 (25) | Volcanic eruption, Colombia | 113 | SRQ | 7 months | 5 years | Six symptoms: time 1, 20– 60; time 2, 13–36 | — | No | |||||||||
| Murphy, 1984 (26); Murphy, 1988 (27) | Volcanic eruption, United States | 155 | 80 | SCL-90-R | 11 months | 3 years | Yes | ||||||||||
| Clayer, 1985 (37) | Bushfires, Australia | 1,526/100# | 52 | Self- constructed | 12 months | Nerve problems: 30; palpitations: 7 | ++ | No | |||||||||
| Maida, 1989 (38) | Bushfires, United States | 25 | DIS/DS | 3 months | Three symptoms: 8–20 | No | |||||||||||
| McFarlane, 1987 (62) | Bushfires, Australia | 808**/ 734#,** | 43 | RQ | 2 and 8 months | 2¼ years | Above cutoff: time 1, 1; time 2, 5; time 3, 7 | ++ | No | ||||||||
| McFarlane, 1997 (47) | Bushfires, Australia | 1,526/ 1,439†† | 77 | GHQ | 12 months | ++ | Yes | ||||||||||
| Dollinger, 1986 (39) | Lightning strike, United States | 29** | MCBC (expansion) | 2 months | Seven symptoms: 3–31 | No | |||||||||||
| Baum, 1983 (48) | Three Mile Island, United States | 38/83# | 70 | SCL-90 | 1½ years | ++ | No | ||||||||||
| Davidson, 1986 (49) | Three Mile Island, United States | 52/35# | 70 | SCL-90-R | 4⅔ years | ++ | Yes | ||||||||||
| Cleary, 1984 (50) | Three Mile Island, United States | 403/1,506# | Self- constructed | 4 and 10 months | ++ | Yes | |||||||||||
| Prince- Embury, 1988 (51) | Three Mile Island, United States | 108/974†† | 51 | SCL-90-R | 6 years | ++ | No | ||||||||||
| Bromet, 2000 (52) | Chernobyl accident, Ukraine | 300**/ 300** | 92/85‡ | CSI and CBCL | 11 years | CSI: ++; CBCL: ++ | Yes | ||||||||||
| Bromet, 2002 (53) | Chernobyl accident, Ukraine | 300/300# | 92/85‡ | SCL-90-R | 11 years | Above cutoff: 55 | ++ | No | |||||||||
| Cwikel, 1997 (44) | Chernobyl accident, Ukraine | 374/334# | 91 | SCL-90 | 8 and 10 years | ++ | ND | Yes | |||||||||
| Havenaar, 1997 (54) | Chernobyl accident, Ukraine | 265/184# | 92/88‡ | BrSI | 6½ years | Above cutoff: 51 | ++ | No | |||||||||
| Holen, 1990 (28); Holen, 1991 (29) | Industrial disaster, Norway | 73/89# | Self-reported symptoms | 5 weeks | 8 years | ++ | No | ||||||||||
| Weisaeth, 1989 (40) | Industrial disaster, Norway | 246 | 98 | PTSS-30 | 1 and 7 months | Time 2: muscle pain, 5–35; fatigue, 3–33 | Yes | ||||||||||
| Grace, 1993 (60) | Buffalo Creek dam collapse, United States | 199/50# | 39 | PEF and SCL-90-R | 14 years | ND | No | ||||||||||
| Shariat, 1999 (41) | Terrorist attack, United States | 494 | 54 | HSQ | 2⅔ years | Five symptoms: 22–44 | Yes | ||||||||||
| Trout, 2002 (42) | Terrorist attack, United States | 191/155# | 68/47‡ | Self- constructed | 3 months | 12 symptoms: 10–66 | ++ | No | |||||||||
| Yokoyama, 1998 (55) | Terrorist attack, Japan | 18/15# | 12 | POMS | 7 months | ++ | Yes | ||||||||||
| Creamer, 1990 (56) | Multiple, shooting, Australia | 446/338# | 53/57‡ | SCL-90-R | 4 months | ++ | No | ||||||||||
| Chung, 1999 (72) | Aircraft disaster, United Kingdom | 82 | 55 | GHQ | 6 months | Yes | |||||||||||
| Donker, 2002 (4) | Aircraft disaster, the Netherlands | 533 | Self-reported symptoms | 6 years | Six symptoms: 9–45 | No | |||||||||||
| Livingston, 1992 (69) | Aircraft disaster, United Kingdom | 55 | GHQ | 12 months | Yes | ||||||||||||
| Tyano, 1996 (57) | Bus-train collision, Israel | 306/83# | 68/82‡ | SCL-90 | 7 years | ++ | Yes | ||||||||||
Response rates of the first measurement time are reported for longitudinal studies. When response rates of different exposure groups were given, the lowest percentage is reported.
SCL-90 (SCL-90-R/SCL-40), Symptom Checklist somatization subscale; CHQ-12, Chinese Health Questionnaire; SRQ, Self-reporting Questionnaire; CPTSD-RI, Children's Posttraumatic Stress Disorder Reaction Index; DIS/DS, Diagnostic Interview Schedule/Disaster Supplement; BSI, Brief Symptom Inventory; PSI, Physical Symptoms Index; GHQ, General Health Questionnaire; SSI, Somatic Symptom Inventory; CFIDS, chronic fatigue immune dysfunction symptoms; RI, Frederick's Reaction Index for Children; TRF, Teacher's Report Form; RQ, Rutter's Questionnaire (parent and teacher); MCBC, Missouri Children's Behavior Checklist; CSI, Children's Somatization Inventory; CBCL, Child Behavior Checklist; BrSI, Bradford Somatic Inventory; PTSS-30, Posttraumatic Stress Scale 30; PEF, Psychiatric Evaluation Form; HSQ, Health Status Questionnaire; POMS, Profile of Mood States fatigue subscale.
Prevalence range of group of medically unexplained symptoms.
Statistically significant difference in score on scale between survivors and controls; “ND” means there is no difference in reported medically unexplained physical symptoms between survivors and controls, “++” means survivors reported more medically unexplained physical symptoms than did controls, and “—” means survivors reported less medically unexplained physical symptoms than did controls.
Statistically significant difference in reported medically unexplained physical symptoms between two time points; “—” means survivors reported less medically unexplained physical symptoms at the second assessment compared with the first assessment, “ND” means there is no difference in reported medically unexplained physical symptoms between the two assessments, and “++” means survivors reported more medically unexplained physical symptoms at the second assessment compared with the first assessment.
Control group.
Children.
Referent data.
Response rates were given in 33 studies, ranging from 12 percent to 100 percent. In the 57 relevant studies, 21 different questionnaires were used to measure MUPS. The SCL-90 somatization subscale was used most often (16 studies). It measured headache, dizziness, pain in the chest or heart, pain in the lower back, nausea or upset stomach, soreness of muscles, difficulty breathing, hot or cold spells, numb or tingling feelings, lump in the throat, feeling bodily washed out, and having a heavy feeling in the arms or legs. In nine studies, MUPS was measured by self-constructed questionnaires.
What is the prevalence rate of MUPS among survivors of disasters at different points in time?
Percentages
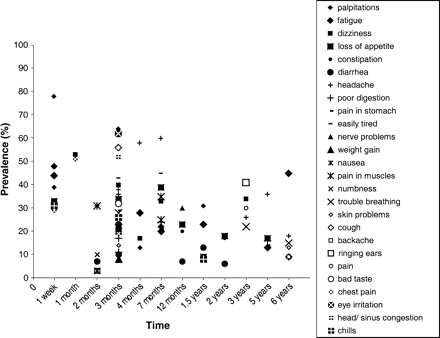
Fifteen studies, primarily after natural disasters, examined the percentage of survivors that reported MUPS (4, 25, 30–42). Table 3 shows for each study the range of the different symptoms that were measured. The prevalence rates of the individual symptoms that were measured are shown in figure 3. The majority of symptoms were measured 3 months after the disaster. This figure shows that there is large variation in the prevalence of different symptoms at the same measurement time, as well as in the prevalence of the same symptoms at different measurement times. For example, the prevalence rate of headache, which was measured in eight studies, varies considerably, with 36 percent 3 months after an earthquake in Ecuador (33), 58 percent 4 months after a hurricane in Honduras (36), and 18 percent 6 years after a plane crash in the Netherlands (4). Fatigue was measured in seven studies; 44 percent of survivors in the United States (30) and 48 percent of survivors in Japan (34) reported fatigue 1 week after an earthquake. Five years after a volcanic eruption in Colombia, 13 percent of survivors reported fatigue (25). Some symptoms, such as eye irritation and skin problems, were rarely measured, and thus little is known about the prevalence rates of these symptoms.
Prevalence rates of individual medically unexplained physical symptoms.
Mean score
Twenty-two studies compared mean scores on scales of MUPS between survivors and controls. Of these studies, 14 were performed after man-made disasters, and the SCL-90 somatization subscale was used most often to measure MUPS (11 studies). In 18 studies, survivors reported a significantly higher mean score than control subjects did (29, 37, 42–57), with risk ratios ranging from 1.1 for the Chernobyl accident after 10 years (44) to 10.6 for the attack on the World Trade Center in New York after 3 months (42). Compared with control subjects, survivors reported more MUPS both shortly after disasters and during a longer term; 11 years after the Chernobyl accident, affected mothers perceived their children as substantially more symptomatic than did mothers in the comparison group (52). The mothers themselves were also more symptomatic than mothers in the control group (odds ratio = 2.4) (53). Three studies did not find a difference in MUPS between survivors and controls, of which two studies were performed about 1 year after a natural disaster (58, 59) and one study was performed 14 years after the Buffalo Creek dam collapse (60). In contrast, in one study 5 years after a flood, less MUPS were found among survivors compared with controls (61).
Course over time
Although figure 3 might suggest that MUPS became less prevalent as the time after the disaster increased, some prevalence rates of MUPS were still high years after a disaster (4). Follow-up studies show inconsistent results about the course of MUPS over time; MUPS significantly decreased between 1 week and 4 months after an earthquake (30) and between 7 months and 5 years after a volcanic eruption (25). In addition, the percentage of survivors reporting MUPS after an earthquake in Japan seemed to decrease as well (34). In contrast, after the Australian bushfires, the percentage of children with MUPS scores above a cutoff value increased between 2 and 8 months after the disaster (62). The prevalence of MUPS did not change among child survivors of an earthquake between 1 and 2 years after the earthquake (32) and among adult survivors of an earthquake between 3 and 9 months (43). Finally, there was no change in the prevalence of MUPS between 8 and 10 years after the Chernobyl accident (44).
Which factors are associated with MUPS among survivors of disasters?
In this section, we will describe factors that were associated with MUPS in the reviewed studies. Biologic markers, such as cortisol level, that cannot be measured by means of questionnaires, will not be described in this section. Most factors were examined in just one single study; in this section, we report on factors that were examined in at least two different studies, using a model with predisposing, precipitating, and perpetuating factors (the 3-P model) (table 4).
Predisposing, precipitating, and perpetuating factors for medically unexplained physical symptoms in survivors of disasters
. | Positive association . | . | Negative association (reference no.)* . | No difference . | . | ||
|---|---|---|---|---|---|---|---|
. | Reference no.* . | Adjustment(s) . | . | Reference no.* . | Adjustment(s) . | ||
| Predisposing factors | |||||||
| Predisaster symptoms | 18† | Gender, age, education, report effect, exposure level | |||||
| 20† | Gender, age, education, employment, marital status | ||||||
| 63† | Gender, age, education, employment, marital status, exposure level | ||||||
| Female gender | 18 | Age, education, predisaster symptoms, report effect, exposure level | 22† | Age, education, income, church attendance, religious salience | |||
| 47 | 63 | Age, education, employment, marital status, predisaster symptoms, exposure level | |||||
| 58 | Age, education, feel secure at home | 67 | |||||
| 59 | |||||||
| 64 | |||||||
| 65 | |||||||
| 66 | Age, stressful life events, social support | ||||||
| High age | 58 | Gender, education, feel secure at home | 65 | 18 | Gender, education, predisaster symptoms, report effect, exposure level | ||
| 68 | 22† | Gender, education, income, church attendance, religious salience | |||||
| 63 | Gender, education, employment, marital status, predisaster symptoms, exposure level | ||||||
| 66 | Gender, stressful life events, social support | ||||||
| 69 | |||||||
| Married | 63 | Gender, age, education, employment, predisaster symptoms, exposure level | |||||
| Low income | 22† | Gender, age, education, church attendance, religious salience | |||||
| Low occupational status | 63 | Gender, age, education, marital status, predisaster symptoms, exposure level | |||||
| Low education | 18 | Gender, age, predisaster symptoms, report effect, exposure level | 22† | Gender, age, income, church attendance, religious salience | |||
| 58 | |||||||
| 63 | Gender, age, employment, marital status, predisaster symptoms, exposure level | ||||||
| Church attendance | 22† | Gender, age, education, income, religious salience | |||||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| Religious salience | 22† | Gender, age, education, income, church attendance | |||||
| Precipitating factors | |||||||
| High physical damage | 18 | Gender, age, education, predisaster symptoms, report effect | 59 | Predisaster symptoms | |||
| 20† | Gender, age, education, employment, marital status, predisaster symptoms | 67 | |||||
| 22† | Gender, age, education, employment, income, church attendance, religious salience | 68 | |||||
| 26 | 71 | ||||||
| 34 | |||||||
| 40† | |||||||
| 45 | |||||||
| 57 | Education, income | ||||||
| 63 | Gender, age, education, employment, marital status, predisaster symptoms | ||||||
| 68 | Age | ||||||
| 70 | |||||||
| High exposure to substances | 44† | ||||||
| High disruption | 68 | Age | |||||
| Importance of deceased person | 66 | Gender, age, social support, self-efficacy | |||||
| Preventability of death | 66 | Gender, age, social support, importance of deceased person | |||||
| Hospitalized/treated | 40 | ||||||
| Financial loss | 70 | Exposure level | |||||
| Relocation | 43 | 45 | |||||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| 70 | Exposure level | ||||||
| Perpetuating factors | |||||||
| Posttraumatic stress disorder symptomatology | 49 | ||||||
| 52 | |||||||
| 55 | Gender, age, education, alcohol consumption, smoking, serum cholinesterase activity | ||||||
| 67 | |||||||
| 72 | |||||||
| Depression | 66 | 68 | |||||
| Psychiatric morbidity | 46 | ||||||
| Psychological distress | 23 | ||||||
| 68 | Age, level of disruption | ||||||
| Active coping | 22† | Gender, age, education, income, church attendance, religious salience, exposure level, avoidant coping | |||||
| 57 | |||||||
| Avoidant coping | 50 | Medically unexplained physical symptoms at previous measurement time, self-esteem, psychotropic drug use | 22† | Gender, age, education, income, church attendance, religious salience, exposure level, active coping | |||
| Optimism | 68 | Age, psychological distress, level of disruption | |||||
| Introspection | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Low self-esteem | 50 | Medically unexplained physical symptoms at previous measurement time, psychotropic drug use, avoidant coping | |||||
| Heavy social burden | 59 | Predisaster symptoms | |||||
| Low social support | 59 | Predisaster symptoms | 27 | Level of exposure, self-efficacy | |||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| 66 | Gender, age, stressful life events | ||||||
| 68 | Age, psychological distress, level of disruption | ||||||
| 73 | |||||||
| Low self-efficacy | 27 | Exposure level, social support | 50 | Medically unexplained physical symptoms at previous measurement time | |||
| Psychotropic drug use | 50 | Medically unexplained physical symptoms at previous measurement time, self-esteem, avoidant coping | |||||
| Drinking | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Smoking | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Bad physical health | 66 | ||||||
| Stressful life events | 66 | Gender, age, social support | |||||
. | Positive association . | . | Negative association (reference no.)* . | No difference . | . | ||
|---|---|---|---|---|---|---|---|
. | Reference no.* . | Adjustment(s) . | . | Reference no.* . | Adjustment(s) . | ||
| Predisposing factors | |||||||
| Predisaster symptoms | 18† | Gender, age, education, report effect, exposure level | |||||
| 20† | Gender, age, education, employment, marital status | ||||||
| 63† | Gender, age, education, employment, marital status, exposure level | ||||||
| Female gender | 18 | Age, education, predisaster symptoms, report effect, exposure level | 22† | Age, education, income, church attendance, religious salience | |||
| 47 | 63 | Age, education, employment, marital status, predisaster symptoms, exposure level | |||||
| 58 | Age, education, feel secure at home | 67 | |||||
| 59 | |||||||
| 64 | |||||||
| 65 | |||||||
| 66 | Age, stressful life events, social support | ||||||
| High age | 58 | Gender, education, feel secure at home | 65 | 18 | Gender, education, predisaster symptoms, report effect, exposure level | ||
| 68 | 22† | Gender, education, income, church attendance, religious salience | |||||
| 63 | Gender, education, employment, marital status, predisaster symptoms, exposure level | ||||||
| 66 | Gender, stressful life events, social support | ||||||
| 69 | |||||||
| Married | 63 | Gender, age, education, employment, predisaster symptoms, exposure level | |||||
| Low income | 22† | Gender, age, education, church attendance, religious salience | |||||
| Low occupational status | 63 | Gender, age, education, marital status, predisaster symptoms, exposure level | |||||
| Low education | 18 | Gender, age, predisaster symptoms, report effect, exposure level | 22† | Gender, age, income, church attendance, religious salience | |||
| 58 | |||||||
| 63 | Gender, age, employment, marital status, predisaster symptoms, exposure level | ||||||
| Church attendance | 22† | Gender, age, education, income, religious salience | |||||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| Religious salience | 22† | Gender, age, education, income, church attendance | |||||
| Precipitating factors | |||||||
| High physical damage | 18 | Gender, age, education, predisaster symptoms, report effect | 59 | Predisaster symptoms | |||
| 20† | Gender, age, education, employment, marital status, predisaster symptoms | 67 | |||||
| 22† | Gender, age, education, employment, income, church attendance, religious salience | 68 | |||||
| 26 | 71 | ||||||
| 34 | |||||||
| 40† | |||||||
| 45 | |||||||
| 57 | Education, income | ||||||
| 63 | Gender, age, education, employment, marital status, predisaster symptoms | ||||||
| 68 | Age | ||||||
| 70 | |||||||
| High exposure to substances | 44† | ||||||
| High disruption | 68 | Age | |||||
| Importance of deceased person | 66 | Gender, age, social support, self-efficacy | |||||
| Preventability of death | 66 | Gender, age, social support, importance of deceased person | |||||
| Hospitalized/treated | 40 | ||||||
| Financial loss | 70 | Exposure level | |||||
| Relocation | 43 | 45 | |||||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| 70 | Exposure level | ||||||
| Perpetuating factors | |||||||
| Posttraumatic stress disorder symptomatology | 49 | ||||||
| 52 | |||||||
| 55 | Gender, age, education, alcohol consumption, smoking, serum cholinesterase activity | ||||||
| 67 | |||||||
| 72 | |||||||
| Depression | 66 | 68 | |||||
| Psychiatric morbidity | 46 | ||||||
| Psychological distress | 23 | ||||||
| 68 | Age, level of disruption | ||||||
| Active coping | 22† | Gender, age, education, income, church attendance, religious salience, exposure level, avoidant coping | |||||
| 57 | |||||||
| Avoidant coping | 50 | Medically unexplained physical symptoms at previous measurement time, self-esteem, psychotropic drug use | 22† | Gender, age, education, income, church attendance, religious salience, exposure level, active coping | |||
| Optimism | 68 | Age, psychological distress, level of disruption | |||||
| Introspection | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Low self-esteem | 50 | Medically unexplained physical symptoms at previous measurement time, psychotropic drug use, avoidant coping | |||||
| Heavy social burden | 59 | Predisaster symptoms | |||||
| Low social support | 59 | Predisaster symptoms | 27 | Level of exposure, self-efficacy | |||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| 66 | Gender, age, stressful life events | ||||||
| 68 | Age, psychological distress, level of disruption | ||||||
| 73 | |||||||
| Low self-efficacy | 27 | Exposure level, social support | 50 | Medically unexplained physical symptoms at previous measurement time | |||
| Psychotropic drug use | 50 | Medically unexplained physical symptoms at previous measurement time, self-esteem, avoidant coping | |||||
| Drinking | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Smoking | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Bad physical health | 66 | ||||||
| Stressful life events | 66 | Gender, age, social support | |||||
Risk factors reported in the accepted studies; reference numbers correspond with the reference numbers in table 3 and the list of references.
Factors were longitudinally analyzed.
Predisposing, precipitating, and perpetuating factors for medically unexplained physical symptoms in survivors of disasters
. | Positive association . | . | Negative association (reference no.)* . | No difference . | . | ||
|---|---|---|---|---|---|---|---|
. | Reference no.* . | Adjustment(s) . | . | Reference no.* . | Adjustment(s) . | ||
| Predisposing factors | |||||||
| Predisaster symptoms | 18† | Gender, age, education, report effect, exposure level | |||||
| 20† | Gender, age, education, employment, marital status | ||||||
| 63† | Gender, age, education, employment, marital status, exposure level | ||||||
| Female gender | 18 | Age, education, predisaster symptoms, report effect, exposure level | 22† | Age, education, income, church attendance, religious salience | |||
| 47 | 63 | Age, education, employment, marital status, predisaster symptoms, exposure level | |||||
| 58 | Age, education, feel secure at home | 67 | |||||
| 59 | |||||||
| 64 | |||||||
| 65 | |||||||
| 66 | Age, stressful life events, social support | ||||||
| High age | 58 | Gender, education, feel secure at home | 65 | 18 | Gender, education, predisaster symptoms, report effect, exposure level | ||
| 68 | 22† | Gender, education, income, church attendance, religious salience | |||||
| 63 | Gender, education, employment, marital status, predisaster symptoms, exposure level | ||||||
| 66 | Gender, stressful life events, social support | ||||||
| 69 | |||||||
| Married | 63 | Gender, age, education, employment, predisaster symptoms, exposure level | |||||
| Low income | 22† | Gender, age, education, church attendance, religious salience | |||||
| Low occupational status | 63 | Gender, age, education, marital status, predisaster symptoms, exposure level | |||||
| Low education | 18 | Gender, age, predisaster symptoms, report effect, exposure level | 22† | Gender, age, income, church attendance, religious salience | |||
| 58 | |||||||
| 63 | Gender, age, employment, marital status, predisaster symptoms, exposure level | ||||||
| Church attendance | 22† | Gender, age, education, income, religious salience | |||||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| Religious salience | 22† | Gender, age, education, income, church attendance | |||||
| Precipitating factors | |||||||
| High physical damage | 18 | Gender, age, education, predisaster symptoms, report effect | 59 | Predisaster symptoms | |||
| 20† | Gender, age, education, employment, marital status, predisaster symptoms | 67 | |||||
| 22† | Gender, age, education, employment, income, church attendance, religious salience | 68 | |||||
| 26 | 71 | ||||||
| 34 | |||||||
| 40† | |||||||
| 45 | |||||||
| 57 | Education, income | ||||||
| 63 | Gender, age, education, employment, marital status, predisaster symptoms | ||||||
| 68 | Age | ||||||
| 70 | |||||||
| High exposure to substances | 44† | ||||||
| High disruption | 68 | Age | |||||
| Importance of deceased person | 66 | Gender, age, social support, self-efficacy | |||||
| Preventability of death | 66 | Gender, age, social support, importance of deceased person | |||||
| Hospitalized/treated | 40 | ||||||
| Financial loss | 70 | Exposure level | |||||
| Relocation | 43 | 45 | |||||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| 70 | Exposure level | ||||||
| Perpetuating factors | |||||||
| Posttraumatic stress disorder symptomatology | 49 | ||||||
| 52 | |||||||
| 55 | Gender, age, education, alcohol consumption, smoking, serum cholinesterase activity | ||||||
| 67 | |||||||
| 72 | |||||||
| Depression | 66 | 68 | |||||
| Psychiatric morbidity | 46 | ||||||
| Psychological distress | 23 | ||||||
| 68 | Age, level of disruption | ||||||
| Active coping | 22† | Gender, age, education, income, church attendance, religious salience, exposure level, avoidant coping | |||||
| 57 | |||||||
| Avoidant coping | 50 | Medically unexplained physical symptoms at previous measurement time, self-esteem, psychotropic drug use | 22† | Gender, age, education, income, church attendance, religious salience, exposure level, active coping | |||
| Optimism | 68 | Age, psychological distress, level of disruption | |||||
| Introspection | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Low self-esteem | 50 | Medically unexplained physical symptoms at previous measurement time, psychotropic drug use, avoidant coping | |||||
| Heavy social burden | 59 | Predisaster symptoms | |||||
| Low social support | 59 | Predisaster symptoms | 27 | Level of exposure, self-efficacy | |||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| 66 | Gender, age, stressful life events | ||||||
| 68 | Age, psychological distress, level of disruption | ||||||
| 73 | |||||||
| Low self-efficacy | 27 | Exposure level, social support | 50 | Medically unexplained physical symptoms at previous measurement time | |||
| Psychotropic drug use | 50 | Medically unexplained physical symptoms at previous measurement time, self-esteem, avoidant coping | |||||
| Drinking | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Smoking | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Bad physical health | 66 | ||||||
| Stressful life events | 66 | Gender, age, social support | |||||
. | Positive association . | . | Negative association (reference no.)* . | No difference . | . | ||
|---|---|---|---|---|---|---|---|
. | Reference no.* . | Adjustment(s) . | . | Reference no.* . | Adjustment(s) . | ||
| Predisposing factors | |||||||
| Predisaster symptoms | 18† | Gender, age, education, report effect, exposure level | |||||
| 20† | Gender, age, education, employment, marital status | ||||||
| 63† | Gender, age, education, employment, marital status, exposure level | ||||||
| Female gender | 18 | Age, education, predisaster symptoms, report effect, exposure level | 22† | Age, education, income, church attendance, religious salience | |||
| 47 | 63 | Age, education, employment, marital status, predisaster symptoms, exposure level | |||||
| 58 | Age, education, feel secure at home | 67 | |||||
| 59 | |||||||
| 64 | |||||||
| 65 | |||||||
| 66 | Age, stressful life events, social support | ||||||
| High age | 58 | Gender, education, feel secure at home | 65 | 18 | Gender, education, predisaster symptoms, report effect, exposure level | ||
| 68 | 22† | Gender, education, income, church attendance, religious salience | |||||
| 63 | Gender, education, employment, marital status, predisaster symptoms, exposure level | ||||||
| 66 | Gender, stressful life events, social support | ||||||
| 69 | |||||||
| Married | 63 | Gender, age, education, employment, predisaster symptoms, exposure level | |||||
| Low income | 22† | Gender, age, education, church attendance, religious salience | |||||
| Low occupational status | 63 | Gender, age, education, marital status, predisaster symptoms, exposure level | |||||
| Low education | 18 | Gender, age, predisaster symptoms, report effect, exposure level | 22† | Gender, age, income, church attendance, religious salience | |||
| 58 | |||||||
| 63 | Gender, age, employment, marital status, predisaster symptoms, exposure level | ||||||
| Church attendance | 22† | Gender, age, education, income, religious salience | |||||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| Religious salience | 22† | Gender, age, education, income, church attendance | |||||
| Precipitating factors | |||||||
| High physical damage | 18 | Gender, age, education, predisaster symptoms, report effect | 59 | Predisaster symptoms | |||
| 20† | Gender, age, education, employment, marital status, predisaster symptoms | 67 | |||||
| 22† | Gender, age, education, employment, income, church attendance, religious salience | 68 | |||||
| 26 | 71 | ||||||
| 34 | |||||||
| 40† | |||||||
| 45 | |||||||
| 57 | Education, income | ||||||
| 63 | Gender, age, education, employment, marital status, predisaster symptoms | ||||||
| 68 | Age | ||||||
| 70 | |||||||
| High exposure to substances | 44† | ||||||
| High disruption | 68 | Age | |||||
| Importance of deceased person | 66 | Gender, age, social support, self-efficacy | |||||
| Preventability of death | 66 | Gender, age, social support, importance of deceased person | |||||
| Hospitalized/treated | 40 | ||||||
| Financial loss | 70 | Exposure level | |||||
| Relocation | 43 | 45 | |||||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| 70 | Exposure level | ||||||
| Perpetuating factors | |||||||
| Posttraumatic stress disorder symptomatology | 49 | ||||||
| 52 | |||||||
| 55 | Gender, age, education, alcohol consumption, smoking, serum cholinesterase activity | ||||||
| 67 | |||||||
| 72 | |||||||
| Depression | 66 | 68 | |||||
| Psychiatric morbidity | 46 | ||||||
| Psychological distress | 23 | ||||||
| 68 | Age, level of disruption | ||||||
| Active coping | 22† | Gender, age, education, income, church attendance, religious salience, exposure level, avoidant coping | |||||
| 57 | |||||||
| Avoidant coping | 50 | Medically unexplained physical symptoms at previous measurement time, self-esteem, psychotropic drug use | 22† | Gender, age, education, income, church attendance, religious salience, exposure level, active coping | |||
| Optimism | 68 | Age, psychological distress, level of disruption | |||||
| Introspection | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Low self-esteem | 50 | Medically unexplained physical symptoms at previous measurement time, psychotropic drug use, avoidant coping | |||||
| Heavy social burden | 59 | Predisaster symptoms | |||||
| Low social support | 59 | Predisaster symptoms | 27 | Level of exposure, self-efficacy | |||
| 50 | Medically unexplained physical symptoms at previous measurement time | ||||||
| 66 | Gender, age, stressful life events | ||||||
| 68 | Age, psychological distress, level of disruption | ||||||
| 73 | |||||||
| Low self-efficacy | 27 | Exposure level, social support | 50 | Medically unexplained physical symptoms at previous measurement time | |||
| Psychotropic drug use | 50 | Medically unexplained physical symptoms at previous measurement time, self-esteem, avoidant coping | |||||
| Drinking | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Smoking | 50 | Medically unexplained physical symptoms at previous measurement time | |||||
| Bad physical health | 66 | ||||||
| Stressful life events | 66 | Gender, age, social support | |||||
Risk factors reported in the accepted studies; reference numbers correspond with the reference numbers in table 3 and the list of references.
Factors were longitudinally analyzed.
Predisposing factors
Predisposing factors already exist before the disaster and are typically risk factors for MUPS in the general population (figure 1). A group that might be at relatively greater risk for MUPS after disasters would be those with preexisting MUPS; three flood studies found, after controlling for demographic characteristics and level of exposure, a positive association between pre- and postflood symptoms (18, 20, 63).
In line with general population studies, women reported higher rates of MUPS in seven studies after natural disasters in which this association was examined (18, 47, 58, 59, 64–66). Three studies did not find an association between reported MUPS and gender (22, 63, 67).
High age, examined in eight studies, was not consistently found to be a risk factor for MUPS. One study among earthquake survivors showed that older subjects reported more MUPS (58). After a hurricane, older survivors reported a greater worsening of chronic fatigue symptoms compared with younger survivors (68). A study among child survivors of a hurricane showed that late adolescents reported less MUPS compared with younger groups (65). Five studies did not find any association between age and MUPS (18, 22, 63, 66, 69).
Education, occupational status, and income are often considered to be indicators of socioeconomic status; these factors were not often examined as a risk factor for MUPS in the reviewed literature. A low educational level was found to be positively associated with MUPS in three studies after natural disasters (58), of which two adjusted for other demographic characteristics, predisaster symptoms, and level of exposure (18, 63). One study did not find this association (22).
Precipitating factors
Involvement in the disaster can manifest itself in different ways. One way is the magnitude of physical damage to oneself, loved ones, and/or property. Another way may consist of exposure to toxic agents, radiation, or biologic agents. A third way is the possible psychological trauma experienced.
High involvement in the disaster defined as the magnitude of damage seems to be an important risk factor for the development of MUPS. Fifteen studies examined this association: 11 studies showed that a high degree of physical damage was positively associated with MUPS (18, 20, 22, 26, 34, 40, 45, 57, 63, 68, 70), and four studies did not find such an association (59, 67, 68, 71).
Three studies that examined the association between relocation and MUPS did not find higher levels of MUPS among those who were relocated (45, 50, 70). In one study, relocated subjects reported less MUPS than those who were not relocated (43). Important to consider in this study was that those who were not relocated experienced significant aftershocks when they returned to their damaged houses, and they received less social support from agencies than did those who were relocated.
Perpetuating factors
Psychological problems are common after disasters and might be important risk factors for MUPS in those affected by disasters. For example, posttraumatic stress symptoms were positively associated with MUPS in five cross-sectional studies (49, 55, 72), of which two were performed among children (52, 67). In addition, two studies found a positive association between psychological distress and MUPS (23, 68).
Coping styles, which refer to the specific way people act in a stressful situation, might be associated with MUPS as well. Two general coping strategies have been distinguished: 1) problem-focused coping or active coping involves the effort to do something active to alleviate stressful circumstances and 2) emotion-focused coping involves the effort to regulate the emotional consequences of stressful events (73). The association between MUPS and active coping was considered in two studies, but no association was found (22, 57). Avoidant coping, engaging in a substitute task, was found to be associated with MUPS among those affected by the Three Mile Island accident (50) but not among survivors of a flood (22).
A study among survivors of a severe flood showed that those who experienced low social support reported more MUPS (59). Five other studies that examined social support did not, however, find this association (27, 50, 66, 68, 74).
DISCUSSION
This review showed that MUPS are common in survivors of disasters and are more prevalent in those affected by disasters compared with the general population. Regardless of the type of disaster, a higher proportion of survivors compared with controls suffer from MUPS both immediately after and in the years following a disaster. In addition, a few consistent risk factors for MUPS, such as female gender as a predisposing factor, high physical damage as a precipitating factor, and posttraumatic stress symptoms as a perpetuating factor, were identified.
Since there is no clear-cut distinction between a major incident and a disaster, we included the keywords “traumatic events” and “life events” in our search strategy. The search identified 3,290 articles: 1,474 in PubMed and 1,816 in other databases. As a result of using the disaster criterion, 86 percent of the studies, mostly performed after individual traumatic events or after war situations, were excluded. This indicates that keywords such as “life events” and “traumatic events” were too general. This was confirmed by a replication of the search in PubMed in which we included solely the keyword “disasters,” without “life events” and “traumatic events”; this search yielded 671 papers.
The prevalence rates of MUPS in the reviewed studies are in accordance with results of studies among people affected by individual traumatic events (75, 76), and among war veterans (15, 77) it is therefore not likely that the results of this review would have been different when we included studies about individual traumatic events and war situations.
Studies about relief workers were excluded on the basis of the subject criterion. Because relief workers, like war veterans, are predominately young (male) adults and more healthy compared with residents, it is likely that studies among relief workers would have yielded lower prevalence rates of MUPS. We accepted studies about child survivors of disasters. Since children seem to report the same symptom patterns as their parents (78), the inclusion of these studies would probably not have affected the results of this review.
Finally, 469 studies were judged on the MUPS criterion. The majority of these studies measured psychological problems, such as posttraumatic stress disorder and depression; we found 57 articles in which MUPS were measured. We excluded studies in which symptoms were likely to be the result of exposure to toxic substances. However, information on dose-response relations for the substance is typically insufficient to make a clear distinction between symptoms from toxicologic effects and MUPS. Therefore, MUPS may also be prevalent after exposure to toxic substances (9, 79).
Few consistent risk factors were observed in the reviewed studies. It is unclear how our selection criteria may have affected the answers to our second research question. The literature on risk factors for MUPS after disasters was even more limited than that on the prevalence rate of MUPS; most risk factors were examined in only one study. However, the identified risk factors for MUPS after disasters were similar to those found in studies among the general population, Gulf War veterans, and victims of sexual assault. For example, female gender was found to be a risk factor for MUPS in the general population (10, 16) and in studies among Gulf War veterans (77, 80). The perpetuating factors posttraumatic stress symptoms and psychological distress were associated with MUPS among survivors of disasters, and this association has also been found in community studies (10, 13), among Gulf War veterans (81, 82), and among victims of sexual assault (76). This indicates that, in particular, predisposing and perpetuating risk factors for MUPS are likely to be similar across different kinds of traumatic events. Precipitating factors might, however, differ across different kinds of traumatic events, and therefore we excluded studies among survivors of individual traumatic events and wartime exposure.
Although this review shows that survivors of disasters report more MUPS compared with controls, we found substantial variation in the reported prevalence rates of MUPS. This variation might have resulted from differences in study characteristics, which make adequate comparison difficult. First, the time of measurement since the disaster differed among studies. Some studies measured MUPS in the months after the disaster, but other studies were performed for the first time years after the disaster. Second, the number of participants as well as the response rate differed among studies. The majority of studies reporting prevalence rates had a low response rate (<60 percent) or did not report any rate. For interpreting the prevalence rate, a high response rate is needed, so that selection bias is limited. Third, the study populations were often not chosen randomly, which might have introduced some bias. However, the use of a random sample is difficult in studies that are performed shortly after a disaster, and therefore convenience samples are frequently used. For convenience samples, information about who did or did not participate in the study is often lacking, and thus the results can either be an under- or overestimation of the true health problems. However, selective participation can also occur in studies that used random sampling. Moreover, after disasters, it is difficult to identify all the eligible survivors, since the affected area as well as the denominator of the affected population cannot always be defined. Fourth, many different questionnaires were used to measure MUPS: 21 different questionnaires in 57 accepted studies. As a result, the number and the type of symptoms that were measured differed among studies. Because of these limitations in the study designs, we cannot draw a definite conclusion about the prevalence rates of MUPS in survivors of disasters.
In contrast to risk factors for MUPS, risk factors for posttraumatic stress disorder have often been studied. Low socioeconomic status, history of psychiatric disorders, and stressful life events have been shown to be risk factors for posttraumatic stress disorder (83), but such an association with MUPS has rarely been studied. In addition, little is known about how different factors interact over time. Nevertheless, three factors seem to be associated with MUPS: the predisposing factor female gender, the precipitating factor high physical damage, and the perpetuating factor posttraumatic stress symptoms.
Since female gender is also a risk factor for MUPS in the general population, the question is whether female gender modifies the effect of the disaster by increasing MUPS after the disaster or whether females already reported more MUPS before the disaster. Because most accepted studies were retrospective, this question cannot be answered; more prospective studies, preferably with a predisaster measurement, are needed to answer this question.
Damage to house or property, injury to oneself or others, serious threat to one's own or one's family member's life, and loss of a loved one were, in most studies, combined into a single exposure variable. Therefore, we reported these factors as the precipitating factor high physical damage in this review. However, the individual exposure variables might be associated with MUPS differently. Future research should consider these factors as different precipitating factors.
Since most studies that examined risk factors for MUPS were cross-sectional or used cross-sectional analyses, we cannot draw a conclusion about causality. For the identification of perpetuating factors (such as posttraumatic stress symptoms and depression) in particular, more longitudinal studies after disasters are needed to answer the question about whether these factors are risk factors or intermediate factors for MUPS.
In conclusion, this review shows that survivors of disasters report more MUPS compared with controls. However, since there is much diversity in study designs among studies, no definite conclusion can be drawn about the prevalence rate of MUPS at different time points after disasters. In addition, a few possible risk factors for MUPS were identified: female gender, high physical damage, and posttraumatic stress symptoms. Many risk factors for MUPS, such as a history of psychiatric disorders and stressful life events, were often studied among the general population or Gulf War veterans, but these factors were rarely studied in survivors of disasters. Therefore, more epidemiologic research after large-scale disasters is needed. To facilitate and prepare epidemiologic studies after disasters, the Dutch Ministry of Welfare, Public Health, and Sports set up the Centre for Health Impact Assessment of Disasters at the National Institute for Public Health and the Environment. Since MUPS impair people's functioning and can be very persistent over time, these future studies must focus on risk factors for MUPS, such as predisaster MUPS or mental health problems and the contribution of individual disaster-related factors, so that survivors at risk for the development of MUPS can be more easily identified.
The authors thank Wim ten Have for helping them with the development of the search strategy and for searching the different databases. They would like to thank Dr. Anja Dirkzwager for evaluating studies on which no consensus could be reached. They would also like to thank Dr. Marc Ruijten for his advice on the studies in which survivors were possibly exposed to toxic substances.
References
Bromet EJ, Havenaar JM. Mental health consequences of disasters. In: Sartorius N, Gaebel W, Lopez-Ibor JJ, et al, eds. Psychiatry in society. New York, NY: John Wiley & Sons, Ltd,
Norris FH, Friedman MJ, Watson PJ, et al. 60,000 disaster victims speak. Part I. An empirical review of the empirical literature, 1981–2001.
Yzermans J, Gersons BPR. The chaotic aftermath of an airplane crash in Amsterdam. In: Havenaar JM, Cwikel JG, Bromet EJ, eds. Toxic turmoil: psychological and societal consequences of ecological disasters. New York, NY: Kluwer Academic/Plenum Publishers,
Donker GA, Yzermans CJ, Spreeuwenberg P, et al. Symptom attribution after a plane crash: comparison between self-reported symptoms and GP records.
van Kamp I, Van der Velden PG, Anyo G, et al. Firework disaster Enschede: physical and mental health and experiences of the disaster. (In Dutch). Bilthoven/Zaltbommel, the Netherlands: National Institute for Public Health and the Environment (RIVM)/Institute for Psychotrauma (IvP),
Van der Velden PG, Grievink L, Dusseldorp A, et al. Firework disaster Enschede: physical and mental health 18 months after the disaster. (In Dutch). Bilthoven/Zaltbommel, the Netherlands: National Institute for Public Health and the Environment (RIVM)/Institute for Psychotrauma (IvP),
Boin A, van Duin M, Heyse L. Toxic fear: the management of uncertainty in the wake of the Amsterdam air crash.
Engel CC, Adkins JA, David NC. Caring for medically unexplained physical symptoms after toxic environmental exposures: effects of contested causation.
Kroenke K, Price RK. Symptoms in the community. Prevalence, classification, and psychiatric comorbidity.
Van der Linden MW, Westert GP, de Bakker DH, et al. Tweede nationale studie naar ziekten en verrichtingen in de huisartsenpraktijk: klachten en aandoeningen in de bevolking in de huisartsenpraktijk. (In Dutch). Utrecht/Bilthoven, the Netherlands: National Institute for Health Services Research/National Institute for Public Health and the Environment,
Kroenke K, Mangelsdorff AD. Common symptoms in ambulatory care: incidence, evaluation, therapy, and outcome.
van Hemert AM, Hengeveld MW, Bolk JH, et al. Psychiatric disorders in relation to medical illness among patients of a general medical out-patient clinic.
Mayou R, Farmer A. ABC of psychological medicine: functional somatic symptoms and syndromes.
Fukuda K, Nisenbaum R, Stewart G, et al. Chronic multisymptom illness affecting Air Force veterans of the Gulf War.
Feder A, Olfson M, Gameroff M, et al. Medically unexplained symptoms in an urban general medicine practice.
Cullinan P, Acquilla SD, Dhara VR. Long term morbidity in survivors of the 1984 Bhopal gas leak.
Bravo M, Rubio-Stipec M, Canino G, et al. The psychological sequelae of disaster stress prospectively and retrospectively evaluated.
Canino G, Bravo M, Rubio-Stipec M, et al. The impact of disaster on mental health: prospective and retrospective analyses.
Phifer J, Kaniasty K, Norris F. The impact of natural disaster on the health of older adults: a multiwave prospective study.
Phifer J, Norris F. Psychological symptoms in older adults following natural disasters: nature, timing, duration, and course.
Smith BW. Coping as a predictor of outcomes following the 1993 Midwest flood.
Smith BW, Freedy JR. Psychosocial resource loss as a mediator of the effects of flood exposure on psychological distress and physical symptoms.
Lima BR, Pai S, Santacruz H, et al. Screening for the psychological consequences of a major disaster in a developing country: Armero, Colombia.
Lima BR, Pai S, Toledo V, et al. Emotional distress in disaster victims: a follow-up study.
Murphy SA. Stress levels and health status of victims of a natural disaster.
Murphy SA. Mediating effects of intrapersonal and social support on mental health 1 and 3 years after a natural disaster.
Holen A. Occurrence and persistence of post-traumatic health problems. In: Holen A, ed. A long-term outcome study of survivors from a disaster. Oslo, Norway: University of Oslo Press,
Holen A. A longitudinal study of the occurrence and persistence of post-traumatic health problems in disaster survivors.
Cardena E, Spiegel D. Dissociative reactions to the San Francisco Bay area earthquake of 1989.
Chen CC, Yeh TL, Yang YK, et al. Psychiatric morbidity and post-traumatic symptoms among survivors in the early stage following the 1999 earthquake in Taiwan.
Kitayama S, Okada Y, Takumi T, et al. Psychological and physical reactions on children after the Hanshin-Awaji earthquake disaster.
Lima BR, Chavez H, Samaniego N, et al. Disaster severity and emotional disturbance: implications for primary mental health care in developing countries.
Tainaka H, Oda H, Nakamura S, et al. Workers' stress after Hanshin-Awaji earthquake in 1995—symptoms related to stress after 18 months. (In Japanese).
Escobar JC, Canino G, Rubio-Stipec M, et al. Somatic symptoms after a natural disaster: a prospective study.
Guill CK, Shandera WX. The effects of hurricane Mitch on a community in northern Honduras.
Clayer JR, Bookless-Pratz C, Harris RL. Some health consequences of a natural disaster.
Maida CA, Gordon NS, Steinberg A, et al. Psychosocial impact of disasters: victims of the Baldwin hills fire.
Dollinger SJ. The measurement of children's sleep disturbances and somatic complaints following a disaster.
Weisaeth L. The stressors and the post-traumatic stress syndrome after an industrial disaster.
Shariat S, Mallonee S, Kruger E, et al. A prospective study of long-term health outcomes among Oklahoma City bombing survivors.
Trout D, Nimgade A, Mueller C, et al. Health effects and occupational exposures among office workers near the World Trade Center disaster site.
Wang X, Gao L, Zhang H, et al. Post-earthquake quality of life and psychological well-being: longitudinal evaluation in a rural community sample in northern China.
Cwikel J, Abdelgani A, Goldsmith JR, et al. Two-year follow up study of stress-related disorders among immigrants to Israel from the Chernobyl area.
Najarian LM, Goenjian AK, Pelcovitz D, et al. The effect of relocation after a natural disaster.
Fairley M, Langeluddecke P, Tennant C. Psychological and physical morbidity in the aftermath of a cyclone.
McFarlane AC, Clayer JR, Bookless FCL. Psychiatric morbidity following a natural disaster: an Australian bushfire.
Baum A, Gatchel RJ, Schaeffer MA. Emotional, behavioral, and physiological effects of chronic stress at Three Mile Island.
Davidson LM, Baum A. Chronic stress and posttraumatic stress disorders.
Cleary PD, Houts PS. The psychological impact of the Three Mile Island incident.
Prince-Embury S, Rooney JF. Psychological symptoms of residents in the aftermath of the Three Mile Island nuclear accident and restart.
Bromet EJ, Goldgaber D, Carlson G, et al. Children's well-being 11 years after the Chornobyl catastrophe.
Bromet EJ, Gluzman S, Schwartz JE, et al. Somatic symptoms in women 11 years after the Chernobyl accident: prevalence and risk factors.
Havenaar J, Rumyantzeva G, van den Brink W, et al. Long-term mental health effects of the Chernobyl disaster: an epidemiologic survey in two former Soviet regions.
Yokoyama K, Araki S, Murata M, et al. Chronic neurobehavioral effects of Tokyo subway sarin poisoning in relation to posttraumatic stress disorder.
Creamer M, Burgess P, Pattison P. Cognitive processing in post-trauma reactions: some preliminary findings.
Tyano S, Iancu I, Solomon Z, et al. Seven-year follow-up of child survivors of a bus-train collision.
Karanci AN, Rustemli A. Psychological consequences of the 1992 Erzincan (Turkey) earthquake.
Solomon SD, Smith EM, Robins L. Social involvement as a mediator of disaster-induced stress.
Grace MC, Green BL, Lindy JD, et al. The Buffalo Creek disaster: a 14-year follow-up. In: Wilson JP, Raphael B, eds. International handbook of traumatic stress syndromes. New York, NY: Plenum Press,
Melick ME, Logue JN. The effect of disaster on the health and well-being of older women.
McFarlane AC, Policansky SK, Irwin C. A longitudinal study of the psychological morbidity in children due to a natural disaster.
Phifer JF. Psychological distress and somatic symptoms after natural disaster: differential vulnerability among older adults.
Anderson KM, Manuel G. Gender differences in reported stress response to the Loma Pietra earthquake.
Shannon MP, Lonigan CJ, Finch AJ Jr, et al. Children exposed to disaster. I. Epidemiology of post-traumatic symptoms and symptom profiles.
Cowan ME, Murphy SA. Identification of postdisaster bereavement risk predictors.
Pynoos RS, Goenjian A, Tashjian M, et al. Post-traumatic stress reactions in children after the 1988 Armenian earthquake.
Lutgendorf SK, Antoni MH, Ironson G, et al. Physical symptoms of chronic fatigue syndrome are exacerbated by the stress of Hurricane Andrew.
Livingston HM. Elderly survivors of the Lockerbie air disaster.
Bland S, O'Leary E, Farinaro E, et al. Long-term psychological effects of natural disasters.
Shaw JA, Tanner S, Perez D, et al. Psychological effects of Hurricane Andrew on an elementary school population.
Chung MC, Easthope Y, Chung C, et al. The relationship between trauma and personality in victims of the Boeing 737-2D6C crash in Coventry.
Folkman S, Lazarus RS. An analysis of coping in a middle-aged community sample.
Cook JD, Bickman L. Social support and psychological symptomatology following a natural disaster.
Flett RA, Kazantzis N, Long NR, et al. Traumatic events and physical health in a New Zealand community sample.
Clum GA, Calhoun KS, Kimerling R. Associations among symptoms of depression and posttraumatic stress disorder and self-reported health in sexually assaulted women.
Gray GC, Reed RJ, Kaiser KS, et al. Self-reported symptoms and medical conditions among 11,868 Gulf War-era veterans: the Seabee Health Study.
Yzermans CJ, Oskam SB. Clustering, continuiteit en comorbiditeit in de huisartsenpraktijk. (In Dutch). (Dissertation). Amsterdam, the Netherlands: University of Amsterdam,
Dayal HH, Baranowski T, Li YH, et al. Hazardous chemicals: psychological dimensions of the health sequelae of a community exposure in Texas.
Storzbach D, Campbell KA, Binder LM, et al. Psychological differences between veterans with and without Gulf War unexplained symptoms.
Barrett DH, Doebbeling CC, Schwartz DA, et al. Posttraumatic stress disorder and self-reported physical health status among U.S. military personnel serving during the Gulf War period: a population-based study.
Wolfe J, Proctor SP, Erickson DJ, et al. Relationship of psychiatric status to Gulf War veterans' health problems.