Abstract
Background
No studies have been conducted in the UK context to date that categorise medications in terms of appropriateness for patients with advanced dementia, or that examine medication use in these vulnerable patients.
Objectives
The objectives of this study were to categorise the appropriateness of a comprehensive list of medications and medication classes for use in patients with advanced dementia; examine the feasibility of conducting a longitudinal prospective cohort study to collect clinical and medication use data; and determine the appropriateness of prescribing for nursing home residents with advanced dementia in Northern Ireland (NI), using the categories developed.
Methods
A three-round Delphi consensus panel survey of expert clinicians was used to categorise the appropriateness of medications for patients with advanced dementia [defined as having Functional Assessment Staging (FAST) scores ranging from 6E to 7F]. This was followed by a longitudinal prospective cohort feasibility study that was conducted in three nursing homes in NI. Clinical and medication use for participating residents with advanced dementia (FAST scores ranging from 6E to 7F) were collected and a short test of dementia severity administered. These data were collected at baseline and every 3 months for up to 9 months or until death. For those residents who died during the study period, data were also collected within 14 days of death. The appropriateness ratings from the consensus panel survey were retrospectively applied to residents’ medication data at each data collection timepoint to determine the appropriateness of medications prescribed for these residents.
Results
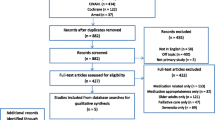
Consensus was achieved for 87 (90 %) of the 97 medications and medication classes included in the survey. Fifteen residents were recruited to participate in the longitudinal prospective cohort feasibility study, four of whom died during the data collection period. Mean numbers of medications prescribed per resident were 16.2 at baseline, 19.6 at 3 months, 17.4 at 6 months and 16.1 at 9 months. Fourteen residents at baseline were taking at least one medication considered by the consensus panel to be never appropriate, and approximately 25 % of medications prescribed were considered to be never appropriate. Post-death data collection indicated a decrease in the proportion of never appropriate medications and an increase in the proportion of always appropriate medications for those residents who died.
Conclusions
This study is the first to develop and apply medication appropriateness indicators for patients with advanced dementia in the UK setting. The Delphi consensus panel survey of expert clinicians was a suitable method of developing such indicators. It is feasible to collect information on quality of life, functional performance, physical comfort, neuropsychiatric symptoms and cognitive function for this subpopulation of nursing home residents with advanced dementia.
Similar content being viewed by others
References
Mitchell SL, Teno JM, Kiely DK, et al. The clinical course of advanced dementia. N Engl J Med. 2009;361(16):1529–38.
Tjia J, Briesacher BA, Peterson D, et al. Use of medications of questionable benefit in advanced dementia. JAMA Intern Med. Epub 2014 Sep 8. doi: 10.1001/jamainternmed.2014.4103.
Currow DCB, Stevenson JP, Abernethy AP, et al. Prescribing in palliative care as death approaches. J Am Geriatr Soc. 2007;55(4):590–5.
Fahlman C, Lynn J, Finch M, et al. Potentially inappropriate medication use by Medicaid Choice beneficiaries in the last year of life. J Palliat Med. 2007;10(3):686–95.
Spinewine A, Schmader KE, Barber N, et al. Appropriate prescribing in elderly people: how well can it be measured and optimised? Lancet. 2007;370(9582):173–84.
Holmes HM. Rational prescribing for patients with a reduced life expectancy. Clin Pharmacol Ther. 2009;85(1):103–7.
O’Mahony D, O’Connor MN. Pharmacotherapy at the end of life. Age Ageing. 2011;40:419–22.
Cruz-Jentoft AJ, Boland B, Rexach L. Drug therapy optimization at the end of life. Drugs Aging. 2012;29:511–21.
Hajjar ER, Cafiero AC, Hanlon JT. Polypharmacy in elderly patients. Am J Geriatr Pharmacother. 2007;5(4):345–51.
Laroche ML, Charmes JP, Bouthier F, et al. Inappropriate medications in the elderly. Clin Pharmacol Ther. 2008;85(1):94–7.
Thorpe JM, Thorpe CT, Kennelty KA, et al. The impact of family caregivers on potentially inappropriate medication use in non-institutionalized older adults with dementia. Am J Geriatr Pharmacother. 2012;10(4):230–41.
Mitchell SL, Kiely DK, Hamel MB. Dying with advanced dementia in the nursing home. Arch Intern Med. 2004;164(3):321–6.
McCarthy M, Addington-Hall J, Altmann D. The experience of dying with dementia: a retrospective study. Int J Geriatr Psychiatry. 1997;12(3):404–9.
Bayer A. Death with dementia—the need for better care. Age Ageing. 2006;35(2):101–2.
Black BS, Finucane T, Baker A, et al. Health problems and correlates of pain in nursing home residents with advanced dementia. Alzheimer Dis Assoc Disord. 2006;20:283–90.
Shega JW, Hougham GW, Stocking CB, et al. Patients dying with dementia: experience at the end of life and impact of hospice care. J Pain Symptom Manage. 2008;35:499–507.
Di Giulio P, Toscani F, Villani D, et al. Dying with advanced dementia in long-term care geriatric institutions. J Palliat Med. 2008;11:1023–8.
Shega J, Tozer C. Improving the care of people with dementia at the end of life: the role of hospice and the US experience. Dementia. 2009;8(3):377–89.
Hendriks SA, Smalbrugge M, Hertogh CMPM, et al. Dying with dementia: symptoms, treatment, and quality of life in the last week of life. J Pain Symptom Manage. 2014;47:710–20.
Blass DM, Black BS, Phillips H, et al. Medication use in nursing home residents with advanced dementia. Int J Geriatr Psychiatry. 2008;23(5):490–6.
Holmes HM, Sachs GA, Shega JW, et al. Integrating palliative medicine into the care of persons with advanced dementia: identifying appropriate medication use. J Am Geriatr Soc. 2008;56(7):1306–11.
Tjia J, Rothman MR, Kiely DK, et al. Daily medication use in nursing home residents with advanced dementia. J Am Geriatr Soc. 2010;58:880–8.
Toscani F, Di Giulio P, Villani D, et al. Treatments and prescriptions in advanced dementia patients residing in long-term care institutions and at home. J Palliat Med. 2013;16(1):31–7.
Mitchell SL, Kiely DK, Jones RN, et al. Advanced dementia research in the nursing home: the CASCADE study. Alzheimer Dis Assoc Disord. 2006;20:166–75.
Molist Brunet N, Sevilla-Sánchez D, Amblàs Novellas J, et al. Optimizing drug therapy in patients with advanced dementia: a patient-centered approach. Eur Geriatr Med. 2014;5:66–71.
Holmes HM, Hayley DC, Alexander GC, et al. Reconsidering medication appropriateness for patients late in life. Arch Intern Med. 2006;166:605–9.
Parsons C, Hughes CM, Passmore AP, et al. Withholding, discontinuing and withdrawing medications in dementia patients at the end of life: a neglected problem in the disadvantaged dying? Drugs Aging. 2010;27(6):435–49.
British National Formulary. Vol 60. London: BMJ Group and Pharmaceutical Press; 2010.
Reisberg B. Functional Assessment Staging (FAST). Psychopharmacol Bull. 1988;24:653–9.
Burns A, Lawlor B, Craig S. Assessment scales in old age psychiatry. 2nd ed. London: Martin Dunitz Ltd; 2004.
Powell C. The Delphi technique: myths and realities. J Adv Nurs. 2003;41(4):376–82.
Charlson ME, Pompei P, Ales KL, et al. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chron Dis. 1987;40(5):373–83.
Pearson Education. SIB-S manual. Oxford: Pearson Assessment; 2008.
Cummings JL, Mega M, Gray K, et al. The Neuropsychiatric Inventory: comprehensive assessment of psychopathology in dementia. Neurology. 1994;44:2308–14.
Lange RT, Hopp GA, Kang N. Psychometric properties and factor structure of the Neuropsychiatric Inventory Nursing Home version in an elderly neuropsychiatric population. Int J Geriatr Psychiatry. 2004;19(5):440–8.
Weiner MF, Martin-Cook K, Svetlik DA, et al. The quality of life in late-stage dementia (QUALID) scale. J Am Med Dir Assoc. 2000;1(3):114–6.
Kiely DK, Volicer L, Teno J, et al. The validity and reliability of scales for the evaluation of end-of-life care in advanced dementia. Alzheimer Dis Assoc Disord. 2006;20(3):176–81.
Volicer L, Hurley AC, Blasi ZV. Scales for evaluation of end-of-life care in dementia. Alzheimer Dis Assoc Disord. 2001;15(4):194–200.
Listone HA, Turoff M. The delphi method: techniques and applications. Reading: Addison-Wesley Publishing Company; 1975.
Campbell SM, Cantrill JA. Consensus methods in prescribing research. J Clin Pharm Ther. 2001;26:5–14.
Parsons C, McCorry N, Murphy K, et al. Assessment of factors that influence physician decision making regarding medication use in patients with dementia at the end of life. Int J Geriatr Psychiatry. 2014;29(3):281–90.
Brown MA, Sampson EL, Jones L, et al. Prognostic indicators of 6-month mortality in elderly people with advanced dementia: a systematic review. Palliat Med. 2013;7(5):389–400.
Vetrano DL, Tosato M, Colloca G, et al. Polypharmacy in nursing home residents with severe cognitive impairment: results from the SHELTER study. Alzheimers Dement. 2013;9:587–93.
Butler DB, Kowall NW, Lawler E, et al. Underuse of diagnostic codes for specific dementias in the veterans affairs New England healthcare system. J Am Geriatr Soc. 2012;60:910–5.
Maddison AR, Fisher J, Johnston G. Preventive medication use among persons with limited life expectancy. Prog Palliat Care. 2011;19:15–21.
Garfinkel D, Zur-Gil S, Ben-Israel J. The war against polypharmacy. A new, cost effective geriatric—palliative approach for improving drug therapy in disabled elderly people. Israel Med Assoc J. 2007;9:430–4.
Garfinkel D, Mangin D. Feasibility study of a new systematic approach for discontinuation of multiple medications in older adults: addressing polypharmacy. Arch Intern Med. 2010;170:1648–54.
Funding sources
The authors had financial support from the Alzheimer’s Society and the Bupa Foundation for the submitted work (grant reference 137). The authors’ work was independent of the funders; the Alzheimer’s Society and the Bupa Foundation did not contribute to the study design; the collection, analysis, or interpretation of data; the writing of the report; or the decision to submit the article for publication.
Conflicts of interest
Peter Passmore has received funding (educational grants) from Napp and Grünenthal and has spoken at and/or chaired meetings for these companies. Napp and Grünenthal had no role in the development, analysis and reporting of this study. The other authors have no conflicts to report.
Author contributions
Carole Parsons, Carmel Hughes, Peter Passmore: study design, analysis, interpretation of data and preparation of the manuscript. Laura McCann: acquisition of data, analysis, interpretation of data and preparation of the manuscript.
Other contributions
The authors wish to thank Dr. Chris Cardwell (School of Medicine, Dentistry and Biomedical Sciences, Queen’s University Belfast, Northern Ireland, UK), and Dr. Holly Holmes (The University of Texas MD Anderson Cancer Center, Houston, TX, USA) for their advice regarding study design. The authors would also like to thank the physicians who participated in the Delphi consensus panel survey, and the residents, their relatives and care home staff who participated in the feasibility study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Parsons, C., McCann, L., Passmore, P. et al. Development and Application of Medication Appropriateness Indicators for Persons with Advanced Dementia: A Feasibility Study. Drugs Aging 32, 67–77 (2015). https://doi.org/10.1007/s40266-014-0226-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40266-014-0226-9