Abstract
There is a large body of experimental evidence in research animals and in vitro models that opioids suppress the immune system. If this effect occurs in acute human disease, then patients cared for in Intensive Care Units (ICUs) would be a particularly vulnerable population. ICU patients have the most severe forms of acute infection, have the greatest risk of acquiring new infections in the hospital, and are exposed to high doses of opioids for long periods of time. We review the epidemiology of ICU infections and the pharmacoepidemiology of opioid use in critically ill patients. We critique the limited human research examining the relationship between opioids and infection and make recommendations on designing future clinical studies that could close the knowledge gap about the true hazards of opioid use in hospitalized patients.
Similar content being viewed by others
Introduction
There is a substantial experimental literature documenting the immunosuppressive effects of opioids at the receptor (Beagles et al. 2004; Tegeder and Geisslinger 2004) cell, (Hatsukari et al. 2006), organ (Wang et al. 2005), and organism (Asakura et al. 2006) level. Since infection is the most common consequence of immunosuppression, most studies have concentrated on one of three infectious models: (1) the effects of chronic opioid exposure on the severity or lethality of a new infectious or lipopolysaccharide (LPS) challenge (MacFarlane et al. 2000; Ocasio et al. 2004); (2) the effect of initiating opioid therapy in a previously infected animal (Chao et al. 1990); or (3) the course of an infection induced in an animal previously made tolerant to opioids and then acutely withdrawn during the infection (Feng et al. 2005). Generally, opioids have been found to have deleterious effects in all three infectious paradigms and across a broad range of pathogenic microorganisms: invasive intracellular (Asakura et al. 2006), extracellular (Wang et al. 2005), and enteric bacteria, (Hilburger et al. 1997), mycobacteria (Olin et al. 2007), protozoans (Chao et al. 1990), yeasts (Di Francesco et al. 1997), and viruses (Hu et al. 2005). Table 1 summarizes experimental animal studies that have reported mortality (Table 1). All of these studies used mice as the experimental animal and used morphine as the experimental opioid. The deleterious effects of morphine were least prominent in the viral infection models. The clinical relevance of the multiple studies that reported that a single large morphine dose after an established infection was fatal compared to equivalent doses in noninfected animals is unclear. It is well known that sicker or debilitated patients are more susceptible to adverse effects of opioids that would otherwise be tolerated by a healthy person. The most consistently lethal model was that of a relatively brief period of morphine exposure (1–3 weeks) followed by infectious challenge. This model would be analogous to ambulatory patients receiving chronic opioids who then develop a severe infection or patients already in the Intensive Care Unit (ICU) who are receiving high doses of opioids and subsequently contract a hospital-acquired infection. Two papers studied LPS challenge after opioid treatment. Because LPS challenge is not an infection but rather a discrete inflammatory stimulus, it may have limited relevance to human infection in the ICU.
Numerous mechanisms by which mu-opioid receptor agonists affect immune cells
Morphine has been demonstrated to modulate immune cell function, in part, through a cAMP mediated mechanism. While acute morphine inhibits adenylate cyclase, chronic morphine and morphine withdrawal results in super activation of adenylate cyclase with a resultant increase in intracellular cAMP (Wang et al. 2007). Several animal studies implicate elevated cAMP with persistent neuroinflammation (Ghavami et al. 2006; Reyes-Irisarri et al. 2007) and cAMP-reducing agents display a potent anti-inflammatory effect in vivo and in vitro studies. Chronic morphine treatment of murine macrophages shows a biphasic response in LPS and Streptococcus pneumoniae-induced proinflammatory cytokine synthesis (Wang et al. 2005). An early inhibitory phase (2–4 h following infection) is observed followed by a later prolonged proinflammatory phase. Chronic morphine treatment significantly and synergistically increase S. pneumoniae induced TNF-α, IL-6, and MCP-1 through modulation of toll-like receptor (TLR) signaling. Although initial studies suggested a simple relationship between different TLRs and exogenous ligands (e.g., TLR4 activated by LPS from gram-negative bacteria or TLR2 activated by peptidogylcan (PGN) from gram positive bacteria), it is now apparent that specific TLRs are activated by numerous exogenous and endogenous ligands and that the downstream effects of the TLR activation are modulated by many other molecules. Bonnet et al. showed that the effects of morphine on the TLR2 signaling pathway depended on the cell type—TNF and IL-6 production by normal human monocytes after peptidoglycan stimulation was inhibited by morphine via a mu-receptor-mechanism, but IL-6 production was not reduced after PGN stimulation of peripheral blood mononuclear cells and the TNF inhibition that was present did not involve mu receptors (Bonnet et al. 2008). Morphine, acting through mu receptors, causes an increase in nitric oxide production which leads to inhibition of several functions of human neutrophils (Welters et al. 2000a, b). Since morphine also causes a similar inhibition of LPS activation of NF-kB that is NO-release mediated (Welters et al. 2000a, b), it is apparent that opioid effects on TLRs and their downstream signaling pathways are complex. We are not aware of any human studies that have shown that opioids increase the susceptibility to gram-negative or gram-positive infections differently. And, opioids affect more than just the innate pathogen pattern-recognition pathway of the immune system; for instance, studies implicate the elevation of cAMP in morphine-induced Th1/Th2 skewing. While elevation of cAMP following chronic morphine in mice inhibits Th1 cytokines (Wang et al. 2003), this same response results in a sustained release of IL-4 and maintenance of the Th2 phenotype (Roy et al. 2005). Also, morphine exposure in vivo rapidly decreases the blood leukocyte gene expression and cell surface display of MHC class II molecules on murine B lymphocytes which could decrease B cell capacity to present antigen to CD4+ T lymphocytes (Beagles et al. 2004).
Finally, although there are numerous opioid pharmacological compounds that interact with the various opioid and immune cell surface receptors, most animal models have studied the opioids used clinically in human medicine: morphine, hydromorphone (Sacerdote et al. 1997), fentanyl (Flores et al. 1995; Yardeni et al. 2008), and methadone (McLachlan et al. 1993).
Considering the body of evidence describing the problem of opioid-induced immunosuppression that has accumulated in the last 20 years, clinicians and medical investigators should be concerned about circumstances or environments where high rates of opioid use intersect with high rates of severe infection. That intersection occurs in the Intensive Care Unit.
Critical illness and intensive care units
Intensive care units are specialized areas within acute care hospitals where patients who have developed organ failure are monitored and treated. Typical interventions include mechanical devices (e.g., ventilators, dialysis machines, blood, or intracranial pressure monitors); medications (e.g., arterial vasoconstrictors, cardiac inotropes, anti-seizure medications); as well as frequent nursing and medical care. There are approximately 5,000 acute care hospitals in the US, and the vast majority has at least a few intensive care beds. About four million people are admitted annually to an ICU (55,000 patients are in an ICU in the US today; Angus et al. 2006) although a substantial proportion are receiving only postoperative care or monitoring, and their ICU stay is only a day or two with a correspondingly low mortality or risk of acquiring a new infection—less than 5%.
ICUs admit a mix of patient types (medical and surgical) to a single unit or admit only specific patient types such as trauma, patients with cardiovascular disease such as myocardial infarction or open heart surgery, neurosciences (brain surgery, severe strokes, and seizures), or burn injury. Because respiratory failure and the need for mechanical ventilation is a major reason for admission to an ICU and because the incidence of respiratory failure increases 88-fold from ages 5–17 to 65–74 (Behrendt 2000), adult ICUs care for a predominantly older population with the mean age of patients with respiratory failure around 59 years old (Esteban et al. 2002).
Patients are frequently admitted to an ICU because an acute severe infection has led to acute organ failure resulting in arterial hypotension, hypoxemia, coma, or kidney failure. Even when infection is not the primary reason for ICU care, organ support often involves breaching the body’s barriers to invasion by microorganisms. This reduction in host defenses, exacerbated by the older and more chronically ill status of many ICU patients and the presence of resistant organisms in the hospital, increases the risk that the patient will acquire a serious infection during their ICU or hospital stay. Therefore, any medication that worsens the course of an established infection or increases the risk of acquiring a new infection should be viewed with concern. Should ICU clinicians be concerned about opioids?
Epidemiology of infections in the intensive care unit
The type of patients admitted to an ICU strongly influences the epidemiology of infection within the ICU—either infections that are the reason for ICU admission, or the frequency, severity and microbiology of infections acquired during the ICU stay. Severe acute infections, most of which are cared for in an ICU, are a major public health problem with the total number of deaths in the US (215,000 per year) comparable to the number of deaths due to acute myocardial infarction (Angus et al. 2001).
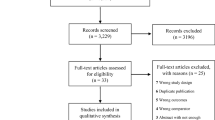
Alberti et al. described the epidemiology of infections in 28 ICUs in eight countries (Alberti et al. 2002). This descriptive epidemiology is important because it highlights the differences in how humans acquire severe infections compared to animal models that examine the effects of opioids on acute or chronic infections. Of 8,353 patients that stayed more than 1 day in the ICU, 3,564 (43%) had one of two types of infection: an infection that was already present at ICU admission (the patient contracted the infection from outside the hospital (n = 1504) or while already in the hospital in a non-ICU ward (n = 1192)); or a new infection that developed during ICU care in a previously noninfected patient (n = 868). Interestingly, 26.4% of patients already infected at ICU admission went on to develop a second infection during their ICU stay. Or, to state the problem in another way, about half of all ICU-acquired infections develop in patients that were already infected upon admission to the ICU. This “double infection” problem has design implications for investigators that wish to determine the effects of opioids on ICU infections and mortality. If the objective were to improve the mortality of patients entering the ICU with an infection, then about one third of ICU patients staying for >24 h would be eligible (this proportion would vary widely between ICU types). But, if the objective were to prevent the acquisition of infections during ICU care, then two thirds of initially noninfected patients would be eligible initially. But this would then exclude patients entering the ICU already infected and this group accounts for about half of ICU-acquired infections and have, in aggregate, a higher mortality (41% compared to 32%) than those entering the ICU without an infection.
Infections of the lung, gastrointestinal tract, urinary system, and bloodstream account for 80% of ICU infections. About a quarter of the infections were classified as severe sepsis which implies there was at least one organ failure attributed to the infection and 30% were classified as septic shock which is the most severe rating implying cardiovascular failure requiring intravenous vasoconstrictor medications to maintain arterial blood pressure.
Although crude infection prevalence rates (number of new or acquired infected patients/number of ICU admissions) of 43% are impressive, incidence-density statistics are a more accurate method of estimating risk over time in a study designed to prevent infections. In a review of studies that reported infection rates in five or more adult or pediatric ICUs, the incidence density ranged from 10.6 ICU-acquired infections/1,000 ICU days to 20.3/1,000 ICU days (Eggimann and Pittet 2001). About three quarters of these new infections were associated with an externally placed invasive medical device (urinary or venous catheter or endotracheal tube for mechanical ventilation). This causal mechanism differs substantially from the experimental animal inoculation protocols that test the effects of opioids on survival after infection or endotoxin exposure (MacFarlane et al. 2000; Ocasio et al. 2004; Wang et al. 2005; Asakura et al. 2006; Feng et al. 2006). Nevertheless, we can conclude that ICUs care for patients with a high incidence of severe infections and that a substantial proportion will develop a new infection, often related to invasive life support and monitoring devices.
Opioid use in the ICU
Opioids are widely used in the ICU because they are potent analgesics, have few clinically apparent adverse effects on other organ systems (gastrointestinal motility being a prominent exception), and have reliable pharmacokinetics in critically ill patients with altered drug metabolism and elimination. Morphine is the first-line analgesic recommended by the Society of Critical Care Medicine clinical practice guideline for mechanically ventilated patients (Jacobi et al. 2002). But, opioids are used for conditions other than pain control. That is because opioids are clinicians’ most reliable medication for relieving dyspnea and respiratory distress during respiratory failure and mechanical ventilation (Bruera et al. 1993; Mazzocato et al. 1999; Ben-Aharon et al. 2008). In addition, because pain assessment is difficult in patients that cannot talk and who are often confused or restrained, opioids are recommended as the first drug to administer when patients are agitated or restless. This is because of concern that unrecognized pain may be present and that the other sedative medications that patient may be receiving (propofol or benzodiazepines) have no analgesic activity.
Therefore, many patients receive parenteral opioids during mechanical ventilation. Clinicians administer sedative medications including opioids to ventilated patient for many reasons (see Table 2; Weinert and Chlan 2001) and since sedative medications achieve these goals with differing specificity, multidrug therapy is often used. The benefits of “co-sedation,” that is, combining medium doses of two sedatives from different pharmacological classes (including an opioid) rather than a high dose of a single sedative (e.g., propofol or a benzodiazepine), has been demonstrated in clinical trials (Richman et al. 2006), and this clinical reasoning probably accounts for the widespread use of opioids even in patients without an apparent need for potent analgesia.
For instance, in a detailed study of sedative therapy in 274 patients mechanically ventilated for at least 48 h, we showed that in 18,050 4-h intervals of mechanical ventilation, at least one of eight medications defined as a sedative was administered intravenously 85% of the time (Weinert and Calvin 2007). Propofol and morphine were the two most commonly administered medications (each about 35% of the time) with lorazepam, hydromorphone, and fentanyl in decreasing frequency. In all, opioids were three of the five most commonly administered sedative medications and were used in 56% of the time blocks in which a sedative was given. Two sedatives were given within the same 4-h interval 31% of the time and three were used in 6%. Thirty-seven percent of the time, the opioid was administered as a continuous infusion. The overall median dose was 0.023 mg/kg/h morphine equivalents which, based on the mean weight of the study patients, is equivalent to about 39 mg/day of parenteral morphine.
How do these doses compare to other studies of ICU patients? For this review, we abstracted data from 43 papers published from 1992 to 2008 that described the use of sedatives or analgesics in ICU patients. In 26 studies, the paper described the drug type, dose, and duration of opioid use in actual ICU patients. In 17 papers, the authors reported the proportion of patients receiving an opioid (but without dose or duration information) or the report described the general practice of sedation and analgesia in the ICU through surveys completed by nurse managers or ICU physicians.
The 43 study designs ranged widely from clinical trials and cohort studies to retrospective cases series and included medical, surgical, or trauma ICUs and ranged from single-center studies to nationwide surveys of hundreds of ICUs. The paper may have described all ICU patients or only mechanically ventilated patients or only those with specific diagnoses such as acute lung injury. The most commonly used opioids were fentanyl and morphine and, if doses were reported, we converted doses to morphine equivalents (10 mg = 100 mcg fentanyl). We then divided the mean daily dose by the reported mean body weight of the subjects, or, if weight was not reported, we imputed 70 kg.
Figure 1 shows the distribution of morphine equivalent doses in mg/kg/day in 26 studies. The median dose was 0.7 mg/kg/day or about 49 mg/day for a patient weighing 70 kg (Sun et al. 1992; Carrasco et al. 1993; Sun and Weissman 1994; Ronan et al. 1995; Kress et al. 1996; Barrientos-Vega et al. 1997; Devlin et al. 1997; McLeod et al. 1997; Watling et al. 1997; Weinbroum et al. 1997; Cammarano et al. 1998; Sanchez-Izquierdo-Riera et al. 1998; Brook et al. 1999; Devlin et al. 1999; Swart et al. 1999; Fraser et al. 2000; Kress et al. 2000; Brandl et al. 2001; Ely et al. 2001; Payen et al. 2001; Ely et al. 2003; De Jonghe et al. 2005; Kahn et al. 2005; Carson et al. 2006; Wolthuis et al. 2007; Girard et al. 2008).
In 17 surveys or practice pattern studies (Fig. 2), the median proportion of ICU or mechanically ventilated patients that received opioids or were “frequently” or “routinely” administered opioids was 80% (Hansen-Flaschen et al. 1991; Dasta et al. 1994; Magarey 1997; Kollef et al. 1998; Christensen and Thunedborg 1999; Murdoch and Cohen 2000; Soliman et al. 2001; Freire et al. 2002; Rhoney and Murry 2003; Samuelson et al. 2003; Guldbrand et al. 2004; Jaber et al. 2005; Martin et al. 2005; Egerod et al. 2006; Martin et al. 2006; Mehta et al. 2006; Richman et al. 2006).
We can conclude that the almost all patients in Intensive Care Units receive opioids and that patients are exposed to substantial intravenous doses of opioids during mechanical ventilation, which, for most critically ill patients, ranges from a few days to several weeks.
Relationship between opioid exposure and infection in hospitalized patients
In standard adult medical–surgical ICUs, there are no clinical studies that have examined the role of opioid exposure in worsening outcomes in infected patients. Three studies in hospitalized patients have examined the effects of opioid therapy, but we have excluded the study by Horn and colleagues because it did not specifically address the role of opioids but rather the association between patient-controlled analgesia pumps and the development of postoperative infection after major intestinal surgery (Horn et al. 2002).
Schwacha and colleagues performed a single-center nested-case control study in burn injury. Cases (n = 187) were patients that developed an infection after thermal injury, and controls (n = 187) were noninfected burn patients that had been in the hospital as long as the cases were at the time of their first infection and were matched for age and total body surface area burned (Schwacha et al. 2006). Aggregate opioid doses in the days prior to the first infection were converted to opioid equivalents (OE) similar to 10 mg of intravenous morphine. The median OE were greater for cases (14 versus ten for controls, p = 0.06) and cases had a longer mean duration of opioid use (approximately 5 days longer) than controls (p < 0.001). The opioid dose differences were greater in less severely burned patients. The authors hypothesized that because large burns are inherently immunosuppressive, the weaker additive effect of opioid immunosuppression was not apparent in more severe thermal injury. However, case-control studies are susceptible to many kinds of bias and results from this type of study design would have to be replicated in different settings before we can conclude that opioids have detrimental effects on infection in thermal injury.
The NEOPAIN trial is the only trial to our knowledge in which large numbers of patients were randomly assigned to liberal morphine exposure versus minimal morphine exposure (Anand et al. 2004). However, the study population of premature infants requiring mechanical ventilation for lung prematurity is a very specialized sample that has a very low rate of infection on admission to the neonatal ICU. Also, the study goal was not to examine infectious complications but to assess the effects of preemptive continuous morphine analgesia on death, brain intraventricular hemorrhage and periventricular leukomalacia. There was no difference in the incidence of these conditions in patient groups assigned to morphine infusions versus those allowed only intermittent open-label morphine. Rates of acquiring new infections were not separately reported. Presumably if there had been significant differences in infectious complications, the authors would have presented the data even if it was not the primary endpoint.
Opioid withdrawal and infection
Although most studies have focused on the adverse effects of chronic opioid therapy, research has also shown that abrupt withdrawal of opioids from tolerant animals has deleterious immunological effects (Feng et al. 2005; Feng et al. 2006). Since the withdrawal model has not been studied as extensively as the chronic opioid model, it is not certain which paradigm causes a more profound immunosuppressed state. In critically ill patients, estimating the incidence of opioid withdrawal is difficult because abstinence symptoms are often indistinguishable from symptoms caused by organ failure, surgery, or adverse effects from other medications commonly administered to hospitalized patients. Nevertheless, rates of symptomatic opioid withdrawal as high as 32% (Cammarano et al. 1998), 53% (Dominguez et al. 2003), and 57% (Katz et al. 1994) have been reported. Not surprisingly, withdrawal symptoms occurred mostly in patients that had received higher doses of opioids for longer periods of time. However, with continuous infusions of potent opioids such as fentanyl, tolerance can occur within 1 week. This high rate of withdrawal, which is probably under recognized in clinical practice, makes designing clinical trials more difficult. If there is an increased rate of late infections in ICU patients, this is due to the presence of opioids or because of the acute decrease in opioid dosing that commonly occurs when patients are removed from mechanical ventilation?
Non-opioid therapies and ICU conditions that cause immunosuppression
Although the focus of this paper is on the clinically relevant immunosuppressive effects of opioids, it is important to recognize that other medications and conditions commonly seen in ICUs have also been shown to negatively affect cellular and humoral aspects of the immune system.
For instance, midazolam, a widely used benzodiazepine sedative, depresses N-formyl-methionyl-leucyl-phenylalanine-induced neutrophil chemiluminescence (Weiss et al. 1993) and neutrophil chemotaxis and phagocytosis in vitro (Nishina et al. 1998). Propofol inhibits several functions of neutrophils that are essential for microbial killing (Mikawa et al. 1998). Both propofol and midazolam inhibit IL-8 secretion (but not intracellular production) from isolated human neutrophils (Galley et al. 1998). In a study conducted in critically ill septic patients, midazolam caused a greater decrease in pro-inflammatory cytokines (IL-1β, IL-6, and TNF-α) during 48 h of drug infusion compared to propofol. However, that study did not have a control group not receiving a sedative so no conclusions can be made on the independent effects of sedative drugs on immune cytokine levels (Helmy and Al-Attiyah 2001).
The tissue injury associated with surgery causes a pro-inflammatory and then a counter-regulatory cascade. This effect can be modulated by the type of pain management (Beilin et al. 2003) or dose of fentanyl administrated to the postoperative patient (Yardeni et al. 2008). Even sleep deprivation, common in ICU patients, affects numerous soluble and cell-mediated immune functions (Rogers et al. 2001).
Transfusion of erythrocytes for anemia occurs in more than 40% of ICU patients, and transfused patients received, on average, five units of erythrocytes and having a transfusion in the ICU was associated with an increased mortality rate (Vincent et al. 2002; Corwin et al. 2004). Although there are more clinical data examining the risk of infection in transfusions than for opioids, the pathophysiological mechanisms remain ill-defined for transfusion-related immunosuppression (Vamvakas and Blajchman 2007). Multiple observational studies show that adults and children have an increased risk of acquiring an ICU infection if they received erythrocyte transfusions (Shorr et al. 2005; Elward and Fraser 2006; Taylor et al. 2006). However, a trial that randomized non-bleeding ICU patients to a restrictive transfusion strategy (no transfusion until hemoglobin fell below 7 g/dl) or a liberal strategy (transfuse when hemoglobin was less than 10 g/dl) showed no difference between groups in the proportion developing a new infection (pneumonia, bacteremia, or septic shock; Hebert et al. 1999).
The underlying assumption of this review is that immunosuppression is harmful because it causes more infections or increases the severity of an established infection. This may be an incorrect hypothesis in certain clinical settings. In a recent review of infectious diseases, judicious use of corticosteroids, a model immunosuppressive medication especially for lymphocytes, was shown to decrease patient mortality in bacterial and tuberculous meningitis, tuberculous pericarditis, typhoid fever, tetanus, and pneumocystis pneumonia. Only in viral hepatitis and cerebral malaria were corticosteroids harmful (McGee and Hirschmann 2008). This discrepancy highlights the difficulty in extrapolating animal models of immunosuppression, infection, and sepsis to human disease (Buras et al. 2005). This extrapolation is likely particularly hazardous in models of endotoxemia or experiments that focus only on early mediators of the inflammatory response (Marshall 2008).
Future clinical research directions
The experimental animal data regarding the deleterious effects of some opioid medications on infection is compelling. Opioids are used frequently and administered in high doses for the most severely ill patients. Ongoing and acquired infections are a major cause of multi-organ failure and death in ICU patients. But, the extent to which opioids are an independent cause of infectious morbidity and mortality in ICU patients remains uncertain. And, because opioids are such valuable medications, clinical practice should be changed only if high-quality research consistently demonstrates that opioids cause a worsening of meaningful endpoints such as mortality or hospital length of stay. In addition, the study design and patient sample should be optimized to answer two different research questions: (1) what is the effect of opioids on infectious diseases causing admission to the ICU and (2) what is the effect of opioids on the risk of acquiring a new infection? Which study designs could answer these questions with a high level of certainty?
Cohort studies are a common observational study design in ICU research. A cohort study would identify every infected patient admitted to the ICU and then record the dose and duration of opioid medications prescribed by the clinical team and then record the subject’s mortality status (usually 28 or 60 days after ICU admission) or length of stay. Then, the investigators would statistically model the relationship between the independent variable of opioid exposure (converted into morphine equivalents as clinical practice often uses several different opioid medications) and the dependent variable of mortality. However, because there is a strong likelihood that opioids are given to patients for reasons that are also associated with the dependent variable of mortality (e.g., need for mechanical ventilation, severity of respiratory failure, surgical procedure), these factors would have to be included into a multivariable model to “adjust” for potentially confounding variables. But statistical adjustment is always incomplete especially when there is incomplete measurement of factors that are associated with the use of opioid therapy. The advantage of this study design is that an analysis could be performed on a extant database as long as there is accurate recording of opioid doses administered, there is the ability to determine whether patients were infected at the time of ICU admission (these data can be difficult to abstract from databases used only for clinical care) and that there is complete endpoint ascertainment. Most of the studies examining the association between erythrocyte transfusion and infection have used a cohort design.
However, because of the need for strong evidence that opioids (and which opioids, specifically) worsen infectious outcomes, a study design that conclusively controls for bias and potentially confounding variables is needed. A randomized trial of sufficient size (probably more than 1,000 patients) could have adequate statistical power to determine if, for example, opioid exposure increases 28-day mortality of infected ICU patients by 10%. But it is unlikely that a conceptually attractive trial could be completed in adults in which one group is assigned to receive no opioids. The clinical practice of co-sedation is increasingly standard practice and caregivers and patients’ families have strong expectations that the patient will not experience any pain during their illness. This makes it unlikely that clinicians or families would allow a patient to be enrolled into a clinical study where one arm receives no opioids. For ethical and feasibility reason, the designers of the NEOPAIN study had to allow intermittent open-label morphine for patients not assigned to the continuous morphine infusion arm. In that study, 55% of the babies were given open-label morphine.
There is another reason not to conduct a trial with a no-opioid arm. Suppose the group randomized to opioids had a 10% increase in mortality. Would this difference be ascribed to the immunosuppressive effects of opioids, or to their deleterious effects on bowel function thereby leading to more malnutrition or to their respiratory depressant effects thereby impairing cough, removal of lung secretions during mechanical ventilation and delayed removal from the ventilator because of excessive sedation? Or would the alternative medication given to the non-opioid group for analgesia have been responsible for the difference in mortality? For instance, ibuprofen inhibition of arachadonic acid metabolism was, at one time, hypothesized to be a treatment for severe sepsis (Bernard et al. 1997). Therefore, the ideal trial would compare two different opioids that experimentally have been shown to have significant differences in immunosuppressive properties but have otherwise similar clinical effects on analgesia, bowel function and relief of dyspnea. For instance, morphine and hydromorphone are both used clinically but in mouse models morphine has greater immunosuppressive activity, as measured by ex vivo tests of splenocyte proliferation, natural killer cell activity and IL-2 production performed 1 h after subcutaneous injection of the test opioids (Sacerdote et al. 1997). It would be relatively simple to prepare identical-appearing infusion bags or syringes with differing concentrations of morphine and hydromorphone such that an equivalent volume, say 1 ml, would deliver an equi-analgesic dose. Any differences in infection rates or mortality could then be more confidently attributed to immunosuppression rather than non-specific opioid effects.
Designing a study to estimate the effects of opioids on infection rates in the outpatient setting has advantages and disadvantages that differ from an ICU study. Certainly the number of patients taking chronic opioids is much larger in the ambulatory setting but, on the other hand, the incidence of new infections is lower. Perhaps a select population that is already immunocompromised, such as cancer patients, would have a sufficiently high risk of infection to increase statistical power. But, in the absence of randomization to opioids or non-opioid analgesics, the same problem with potentially confounding variables would bias the interpretation of the results. In the ambulatory setting, the “opioid exposure” variable would differ compared to the ICU setting: the former exposes patient to relatively low doses but for months and years of duration; the latter exposes patients to very high doses but for durations of only days to weeks. Almost all animal infection models use opioid exposure durations of less than 3 weeks, but, on the other hand, this is of sufficient duration that tolerance develops thereby mimicking the clinical model of chronic human opioid exposure.
Conclusion
There are compelling animal data documenting the immunosuppressive effects of opioids and their causal relationship to worse outcomes during an infectious challenge. However, opioids are an effective therapy for many human patient problems in the ICU. Therefore, research has to definitively demonstrate that opioids worsen meaningful patient outcomes before changes in routine clinical practice can be recommended. This means that clinical researchers need to increase awareness within the medical system about the potential health hazards of opioid use in acute care medicine and then design and obtain support for clinical trials that can investigate this important topic.
References
Alberti C, Brun-Buisson C, Burchardi H, Martin C, Goodman S, Artigas A et al (2002) Epidemiology of sepsis and infection in ICU patients from an international multicentre cohort study. Intensive Care Med 28:108–121 doi:10.1007/s00134-001-1143-z
Anand KJ, Hall RW, Desai N, Shephard B, Bergqvist LL, Young TE et al (2004) Effects of morphine analgesia in ventilated preterm neonates: primary outcomes from the NEOPAIN randomised trial. Lancet 363:1673–1682 doi:10.1016/S0140-6736(04)16251-X
Angus D, Linde-Zwirble W, Lidicker J, Clermont G, Carcillo J, Pinsky M (2001) Epidemiology of severe sepsis in the United States: Analysis of incidence, outcomes and associated costs of care. Crit Care Med 29:1303–1310 doi:10.1097/00003246-200107000-00002
Angus DC, Shorr AF, White A, Dremsizov TT, Schmitz RJ, Kelley MA (2006) Critical care delivery in the United States: distribution of services and compliance with Leapfrog recommendations. Crit Care Med 34:1016–1024 doi:10.1097/01.CCM.0000206105.05626.15
Asakura H, Watarai M, Shirahata T, Makino S (2002) Viable but nonculturable Salmonella species recovery and systemic infection in morphine-treated mice. J Infect Dis 186:1526–1529 doi:10.1086/344353
Asakura H, Kawamoto K, Igimi S, Yamamoto S, Makino S (2006) Enhancement of mice susceptibility to infection with Listeria monocytogenes by the treatment of morphine. Microbiol Immunol 50:543–547
Barrientos-Vega R, Sanchez-Soria M, Morales-Garcia C, Robas-Gomez A, Cuena-Boy R, Ayensa-Rincon A (1997) Prolonged sedation of critically ill patients with midazolam or propofol: Impact on weaning and costs. Crit Care Med 25:33–40 doi:10.1097/00003246-199701000-00009
Beagles K, Wellstein A, Bayer B (2004) Systemic morphine administration suppresses genes involved in antigen presentation. Mol Pharmacol 65:437–442 doi:10.1124/mol.65.2.437
Behrendt C (2000) Acute respiratory failure in the United States: incidence and 31-day survival. Chest 118:1100–1105 doi:10.1378/chest.118.4.1100
Beilin B, Shavit Y, Trabekin E, Mordashev B, Mayburd E, Zeidel A et al (2003) The effects of postoperative pain management on immune response to surgery. Anesth Analg 97:822–827 doi:10.1213/01.ANE.0000078586.82810.3B
Ben-Aharon I, Gafter-Gvili A, Paul M, Leibovici L, Stemmer SM (2008) Interventions for alleviating cancer-related dyspnea: a systematic review. J Clin Oncol 26:2396–2404 doi:10.1200/JCO.2007.15.5796
Bernard GR, Wheeler AP, Russell JA, Schein R, Summer WR, Steinberg KP et al (1997) The effects of ibuprofen on the physiology and survival of patients with sepsis. The Ibuprofen in Sepsis Study Group. N Engl J Med 336:912–918 doi:10.1056/NEJM199703273361303
Bonnet MP, Beloeil H, Benhamou D, Mazoit JX, Asehnoune K (2008) The mu opioid receptor mediates morphine-induced tumor necrosis factor and interleukin-6 inhibition in toll-like receptor 2-stimulated monocytes. Anesth Analg 106:1142–1149
Brandl K, Langley K, Riker R, Dork L, Qualls C, Levy H (2001) Confirming the reliability of the Sedation-Agitation Scale administered by ICU nurses without experience in its use. Pharmacotherapy 21:431–436 doi:10.1592/phco.21.5.431.34487
Brook AD, Ahrens TS, Schaiff R, Prentice D, Sherman G, Shannon W et al (1999) Effect of a nursing-implemented sedation protocol on the duration of mechanical ventilation. Crit Care Med 27:2609–2615 doi:10.1097/00003246-199912000-00001
Bruera E, MacEachern T, Ripamonti C, Hanson J (1993) Subcutaneous morphine for dyspnea in cancer patients. Ann Intern Med 119:906–907
Buras JA, Holzmann B, Sitkovsky M (2005) Animal models of sepsis: setting the stage. Nat Rev Drug Discov 4:854–865 doi:10.1038/nrd1854
Cammarano WB, Pittet J-F, Weitz S, Schlobohm RM, Marks JD (1998) Acute withdrawal syndrome related to the administration of analgesic and sedative medications in adult intensive care unit patients. Crit Care Med 26:676–684 doi:10.1097/00003246-199804000-00015
Carrasco G, Molina R, Costa J, Soler J, Cabre L (1993) Propofol vs midazolam in short-, medium-, and long-term sedation of critically ill patients. A cost-benefit analysis. Chest 103:557–564 doi:10.1378/chest.103.2.557
Carson S, Kress J, Rodgers J, Vinayak A, Campbell-Bright S, Levitt J et al (2006) A randomized trial of intermittent lorazepam versus propofol with daily interruption in mechanically ventilated patients. Crit Care Med 34:1326–1332 doi:10.1097/01.CCM.0000215513.63207.7F
Chao CC, Sharp BM, Pomeroy C, Filice GA, Peterson PK (1990) Lethality of morphine in mice infected with Toxoplasma gondii. J Pharmacol Exp Ther 252:605–609
Christensen BV, Thunedborg LP (1999) Use of sedatives, analgesics and neuromuscular blocking agents in Danish ICUs 1996/97. A national survey. Intensive Care Med 25:186–191 doi:10.1007/s001340050814
Corwin HL, Gettinger A, Pearl RG, Fink MP, Levy MM, Abraham E et al (2004) The CRIT Study: Anemia and blood transfusion in the critically ill–current clinical practice in the United States. Crit Care Med 32:39–52 doi:10.1097/01.CCM.0000104112.34142.79
Dasta JF, Furham TM, McCandles C (1994) Patterns of prescribing and administering drugs for agitation and pain in patients in a surgical intensive care unit. Crit Care Med 22:974–980
De Jonghe B, Bastuji-Garin S, Fangio P, Lacherade JC, Jabot J, Appere-De-Vecchi C et al (2005) Sedation algorithm in critically ill patients without acute brain injury. Crit Care Med 33:120–127 doi:10.1097/01.CCM.0000150268.04228.68
Devlin JW, Holbrook AM, Fuller HD (1997) The effect of ICU sedation guidelines and pharmacist interventions on clinical outcomes and drug cost. Ann Pharmacother 31:689–695
Devlin JW, Boleski G, Mlynarek M, Nerenz DR, Peterson E, Jankowski M et al (1999) Motor activity assessment scale: a valid and reliable sedation scale for use with mechanically ventilated patients in an adult surgical intensive care unit. Crit Care Med 27:1271–1275 doi:10.1097/00003246-199907000-00008
Di Francesco P, Gaziano R, Casalinuovo IA, Palamara AT, Favalli C, Garaci E (1997) Antifungal and immunoadjuvant properties of fluconazole in mice immunosuppressed with morphine. Chemotherapy 43:198–203
Dominguez KD, Lomako DM, Katz RW, Kelly HW (2003) Opioid withdrawal in critically ill neonates. Ann Pharmacother 37:473–477 doi:10.1345/aph.1C324
Egerod I, Christensen BV, Johansen L (2006) Nurses’ and physicians’ sedation practices in Danish ICUs in 2003 A national survey. Intensive Crit Care Nurs 22:22–31 doi:10.1016/j.iccn.2005.02.003
Eggimann P, Pittet D (2001) Infection control in the ICU. Chest 120:2059–2093 doi:10.1378/chest.120.6.2059
Elward AM, Fraser VJ (2006) Risk factors for nosocomial primary bloodstream infection in pediatric intensive care unit patients: a 2-year prospective cohort study. Infect Contr Hosp Epi 27:553–560 doi:10.1086/505096
Ely E, Inouye S, Bernard G, Gordon S, Francis J, May L et al (2001) Delirium in mechanically ventilated patients. Validity and reliability of the Confusion Assessment Method for the Intensive Care Unit (CAM-ICU). JAMA 286:2703–2710 doi:10.1001/jama.286.21.2703
Ely EW, Truman B, Shintani A, Thomason JW, Wheeler AP, Gordon S et al (2003) Monitoring sedation status over time in ICU patients: reliability and validity of the Richmond Agitation-Sedation Scale (RASS). JAMA 289:2983–2991 doi:10.1001/jama.289.22.2983
Esteban A, Anzueto A, Frutos F, Alia I, Brochard L, Stewart T et al (2002) Characteristics and outcomes in adult patients receiving mechanical ventilation. JAMA 287:345–355 doi:10.1001/jama.287.3.345
Feng P, Wilson QM, Meissler JJ Jr, Adler MW, Eisenstein TK (2005) Increased sensitivity to Salmonella enterica serovar Typhimurium infection in mice undergoing withdrawal from morphine is associated with suppression of interleukin-12. Infect Immun 73:7953–7959 doi:10.1128/IAI.73.12.7953-7959.2005
Feng P, Truant AL, Meissler JJ Jr, Gaughan JP, Adler MW, Eisenstein TK (2006) Morphine withdrawal lowers host defense to enteric bacteria: spontaneous sepsis and increased sensitivity to oral Salmonella enterica serovar Typhimurium infection. Infect Immun 74:5221–5226 doi:10.1128/IAI.00208-06
Flores LR, Wahl SM, Bayer BM (1995) Mechanisms of morphine-induced immunosuppression: effect of acute morphine administration on lymphocyte trafficking. J Pharmacol Exp Ther 272:1246–1251
Fraser GL, Prato BS, Riker RR, Berthiaume D, Wilkins ML (2000) Frequency, severity and treatment of agitation in young versus elderly patients in the ICU. Pharmacotherapy 20:75–82 doi:10.1592/phco.20.1.75.34663
Freire AX, Afessa B, Cawley P, Phelps S, Bridges L (2002) Characteristics associated with analgesia ordering in the intensive care unit and relationships with outcome. Crit Care Med 30:2468–2472 doi:10.1097/00003246-200211000-00011
Galley HF, Dubbels AM, Webster NR (1998) The effect of midazolam and propofol on interleukin-8 from human polymorphonuclear leukocytes. Anesth Analg 86:1289–1293 doi:10.1097/00000539-199806000-00030
Ghavami A, Hirst WD, Novak TJ (2006) Selective phosphodiesterase (PDE)-4 inhibitors: a novel approach to treating memory deficit. Drugs R D 7:63–71 doi:10.2165/00126839-200607020-00001
Girard TD, Kress JP, Fuchs BD, Thomason JW, Schweickert WD, Pun BT et al (2008) Efficacy and safety of a paired sedation and ventilator weaning protocol for mechanically ventilated patients in intensive care (Awakening and Breathing Controlled trial): a randomised controlled trial. Lancet 371:126–134 doi:10.1016/S0140-6736(08)60105-1
Guldbrand P, Berggren L, Brattebo G, Malstam J, Ronholm E, Winso O, Scandinavian Critical Care Trials G (2004) Survey of routines for sedation of patients on controlled ventilation in Nordic intensive care units. Acta Anaesthesiol Scand 48:944–950 doi:10.1111/j.1399-6576.2004.00445.x
Hansen-Flaschen JH, Brazinsky S, Basile C, Lanken PN (1991) Use of sedating drugs and neuromuscular blocking agents in patients requiring mechanical ventilation for respiratory failure. A national survey. JAMA 266:2870–2875 doi:10.1001/jama.266.20.2870
Hatsukari I, Hitosugi N, Dinda A, Singhal PC (2006) Morphine modulates monocyte-macrophage conversion phase. Cell Immunol 239:41–48 doi:10.1016/j.cellimm.2006.03.004
Hebert PC, Wells G, Blajchman MA, Marshall J, Martin C, Pagliarello G et al (1999) A multicenter, randomized, controlled clinical trial of transfusion requirements in critical care. Transfusion requirements in critical care investigators, Canadian Critical Care Trials Group. N Engl J Med 340:409–417 doi:10.1056/NEJM199902113400601
Helmy SA, Al-Attiyah RJ (2001) The immunomodulatory effects of prolonged intravenous infusion of propofol versus midazolam in critically ill surgical patients. Anaesthesia 56:4–8 doi:10.1046/j.1365-2044.2001.01713.x
Hilburger ME, Adler MW, Truant AL, Meissler JJ Jr, Satishchandran V, Rogers TJ et al (1997) Morphine induces sepsis in mice. J Infect Dis 176:183–188 doi:10.1086/513791
Horn SD, Wright HL, Couperus JJ, Rhodes RS, Smout RJ, Roberts KA et al (2002) Association between patient-controlled analgesia pump use and postoperative surgical site infection in intestinal surgery patients. Surg Infect (Larchmt) 3:109–118 doi:10.1089/109629602760105772
Hu S, Sheng WS, Lokensgard JR, Peterson PK (2005) Morphine potentiates HIV-1 gp120-induced neuronal apoptosis. J Infect Dis 191:886–889 doi:10.1086/427830
Jaber S, Chanques G, Altairac C, Sebbane M, Vergne C, Perrigault PF et al (2005) A prospective study of agitation in a medical-surgical ICU: incidence, risk factors, and outcomes. Chest 128:2749–2757 doi:10.1378/chest.128.4.2749
Jacobi J, Fraser GL, Coursin DB, Riker RR, Fontaine D, Wittbrodt ET, Chalfin DB, Masica MF, Bjerke HS, Coplin WM, Crippen DW, Fuchs BD, Kelleher RM, Marik PE, Nasraway SA Jr, Murray MJ, Peruzzi WT, Lumb PD, Task Force of the American College of Critical Care Medicine of the Society of Critical Care Medicine (2002) Clinical practice guidelines for the sustained use of sedatives and analgesics in the critically ill adult. Crit Care Med 30:119–141 doi:10.1097/00003246-200201000-00020
Kahn JM, Andersson L, Karir V, Polissar NL, Neff MJ, Rubenfeld GD (2005) Low tidal volume ventilation does not increase sedation use in patients with acute lung injury. Crit Care Med 33:766–771 doi:10.1097/01.CCM.0000157786.41506.24
Katz R, Kelly HW, Hsi A (1994) Prospective study on the occurrence of withdrawal in critically ill children who receive fentanyl by continuous infusion. Crit Care Med 22:763–767 doi:10.1097/00003246-199405000-00009
Kollef MH, Levy NT, Ahrens TS, Schaiff R, Prentice D, Sherman G (1998) The use of continuous IV sedation is associated with prolongation of mechanical ventilation. Chest 114:541–548 doi:10.1378/chest.114.2.541
Kress JP, O’Connor MF, Pohlman AS, Olson D, Lavoie A, Toledano A et al (1996) Sedation of critically ill patients during mechanical ventilation. A comparison of propofol and midazolam. Am J Respir Crit Care Med 153:1012–1018
Kress J, Pohlman A, O’Connor M, Hall J (2000) Daily interruption of sedative infusions in critically ill patients undergoing mechanical ventilation. N Engl J Med 342:1471–1477 doi:10.1056/NEJM200005183422002
MacFarlane AS, Peng X, Meissler JJ Jr, Rogers TJ, Geller EB, Adler MW et al (2000) Morphine increases susceptibility to oral Salmonella typhimurium infection. J Infect Dis 181:1350–1358 doi:10.1086/315403
Magarey J (1997) Sedation of adult critically ill ventilated patients in intensive care units: a national survey. Aust Crit Care 10:90–93 doi:10.1016/S1036-7314(97)70406-5
Marshall JC (2008) Sepsis: rethinking the approach to clinical research. J Leukoc Biol 83:471–482 doi:10.1189/jlb.0607380
Martin J, Parsch A, Franck M, Wernecke KD, Fischer M, Spies C (2005) Practice of sedation and analgesia in German intensive care units: results of a national survey. Crit Care 9:R117–R123 doi:10.1186/cc3035
Martin J, Franck M, Fischer M, Spies C (2006) Sedation and analgesia in German intensive care units: how is it done in reality? Results of a patient-based survey of analgesia and sedation. Intensive Care Med 32:1137–1142 doi:10.1007/s00134-006-0214-6
Mazzocato C, Buclin T, Rapin CH (1999) The effects of morphine on dyspnea and ventilatory function in elderly patients with advanced cancer: a randomized double-blind controlled trial. Ann Oncol 10:1511–1514 doi:10.1023/A:1008337624200
McGee S, Hirschmann J (2008) Use of corticosteroids in treating infectious diseases. Arch Intern Med 168:1034–1046 doi:10.1001/archinte.168.10.1034
McLachlan C, Crofts N, Wodak A, Crowe S (1993) The effects of methadone on immune function among injecting drug users: a review. Addiction 88:257–263 doi:10.1111/j.1360-0443.1993.tb00809.x
McLeod G, Wallis C, Dick J, Cox C, Patterson A, Colvin J (1997) Use of 2% propofol to produce diurnal sedation in critically ill patients. Int Care Med 23:428–434 doi:10.1007/s001340050352
Mehta S, Burry L, Fischer S, Martinez-Motta JC, Hallett D, Bowman D, Wong C, Meade MO, Stewart TE, Cook DJ, Canadian Critical Care Trials G (2006) Canadian survey of the use of sedatives, analgesics, and neuromuscular blocking agents in critically ill patients. Crit Care Med 34:374–380 doi:10.1097/01.CCM.0000196830.61965.F1
Mikawa K, Akamatsu H, Nishina K, Shiga M, Maekawa N, Obara H et al (1998) Propofol inhibits human neutrophil functions. Anesth Analg 87:695–700 doi:10.1097/00000539-199809000-00039
Murdoch S, Cohen A (2000) Intensive care sedation: a review of current British practice. Intensive Care Med 26:922–928 doi:10.1007/s001340051282
Nishina K, Akamatsu H, Mikawa K, Shiga M, Maekawa N, Obara H et al (1998) The inhibitory effects of thiopental, midazolam, and ketamine on human neutrophil functions. Anesth Analg 86:159–165 doi:10.1097/00000539-199801000-00032
Ocasio FM, Jiang Y, House SD, Chang SL (2004) Chronic morphine accelerates the progression of lipopolysaccharide-induced sepsis to septic shock. J Neuroimmunol 149:90–100 doi:10.1016/j.jneuroim.2003.12.016
Olin MR, Choi K, Lee J, Peterson PK, Molitor TW (2007) Morphine modulates gammadelta lymphocytes cytolytic activity following BCG vaccination. Brain Behav Immun 21:195–201 doi:10.1016/j.bbi.2006.06.003
Payen J-F, Bru O, Bosson J-L, Lagrasta A, Novel E, Deschaux I et al (2001) Assessing pain in critically ill sedated patients by using a behavioral pain scale. Crit Care Med 29:2258–2263 doi:10.1097/00003246-200112000-00004
Reyes-Irisarri E, Sanchez AJ, Garcia-Merino JA, Mengod G (2007) Selective induction of cAMP phosphodiesterase PDE4B2 expression in experimental autoimmune encephalomyelitis. J Neuropathol Exp Neurol 66:923–931
Rhoney DH, Murry KR (2003) National survey of the use of sedating drugs, neuromuscular blocking agents, and reversal agents in the intensive care unit. J Intensive Care Med 18:139–145 doi:10.1177/0885066603251200
Richman PS, Baram D, Varela M, Glass PS (2006) Sedation during mechanical ventilation: a trial of benzodiazepine and opiate in combination. Crit Care Med 34:1395–1401 doi:10.1097/01.CCM.0000215454.50964.F8
Rogers NL, Szuba MP, Staab JP, Evans DL, Dinges DF (2001) Neuroimmunologic aspects of sleep and sleep loss. Semin Clin Neuropsychiatry 6:295–307 doi:10.1053/scnp.2001.27907
Ronan KP, Gallagher TJ, George B, Hamby B (1995) Comparison of propofol and midazolam for sedation in intensive care unit patients. Crit Care Med 23:286–293 doi:10.1097/00003246-199502000-00014
Roy S, Cain KJ, Charboneau RG, Barke RA (1998) Morphine accelerates the progression of sepsis in an experimental sepsis model. Adv Exp Med Biol 437:21–31
Roy S, Wang J, Charboneau R, Loh HH, Barke RA (2005) Morphine induces CD4+ T cell IL-4 expression through an adenylyl cyclase mechanism independent of the protein kinase A pathway. J Immunol 175:6361–6367
Sacerdote P, Manfredi B, Mantegazza P, Panerai AE (1997) Antinociceptive and immunosuppressive effects of opiate drugs: a structure-related activity study. Br J Pharmacol 121:834–840 doi:10.1038/sj.bjp.0701138
Samuelson KA, Larsson S, Lundberg D, Fridlund B (2003) Intensive care sedation of mechanically ventilated patients: a national Swedish survey. Intensive Crit Care Nurs 19:350–362 doi:10.1016/S0964-3397(03)00065-X
Sanchez-Izquierdo-Riera JA, Caballero-Cubedo RE, Perez-Vela JL, Ambros-Checa A, Cantalapiedra-Santiago JA, Alted-Lopez E (1998) Propofol versus midazolam: safety and efficacy for sedating the severe trauma patient. Anesth Analg 86:1219–1224 doi:10.1097/00000539-199806000-00016
Schwacha MG, McGwin G Jr, Hutchinson CB, Cross JM, Maclennan PA, Rue LW 3rd (2006) The contribution of opiate analgesics to the development of infectious complications in burn patients. Am J Surg 192:82–86 doi:10.1016/j.amjsurg.2006.01.001
Shorr AF, Jackson WL, Kelly KM, Fu M, Kollef MH (2005) Transfusion practice and blood stream infections in critically ill patients. Chest 127:1722–1728 doi:10.1378/chest.127.5.1722
Soliman H, Melot C, Vincent J (2001) Sedative and analgesic practice in the intensive care unit: the results of a European survey. Br J Anaesth 87:186–192 doi:10.1093/bja/87.2.186
Starec M, Rouveix B, Sinet M, Chau F, Desforges B, Pocidalo JJ et al (1991) Immune status and survival of opiate- and cocaine-treated mice infected with Friend virus. J Pharmacol Exp Ther 259:745–750
Sun X, Weissman C (1994) The use of analgesics and sedatives in critically ill patients: Physicians' orders versus medications administered. Heart Lung 23:169–176
Sun X, Quinn T, Weissman C (1992) Patterns of sedation and analgesia in the postoperative ICU patient. Chest 101:1625–1632 doi:10.1378/chest.101.6.1625
Swart EL, Strack van Schijndel RJM, van Loenen AC, Thijs LG (1999) Continuous infusion of lorazepam versus midazolam in patients in the intensive care unit: Sedation with lorazepam is easier to manage and is more cost-effective. Crit Care Med 27:1461–1465 doi:10.1097/00003246-199908000-00009
Taylor RW, O’Brien J, Trottier SJ, Manganaro L, Cytron M, Lesko MF et al (2006) Red blood cell transfusions and nosocomial infections in critically ill patients. Crit Care Med 34:2302–2308 doi:10.1097/01.CCM.0000234034.51040.7F
Tegeder I, Geisslinger G (2004) Opioids as modulators of cell death and survival–unraveling mechanisms and revealing new indications. Pharmacol Rev 56:351–369 doi:10.1124/pr.56.3.2
Vamvakas EC, Blajchman MA (2007) Transfusion-related immunomodulation (TRIM): an update. Blood Rev 21:327–348 doi:10.1016/j.blre.2007.07.003
Veyries ML, Sinet M, Desforges B, Rouveix B (1995) Effects of morphine on the pathogenesis of murine Friend retrovirus infection. J Pharmacol Exp Ther 272:498–504
Vincent JL, Baron JF, Reinhart K, Gattinoni L, Thijs L, Webb A et al (2002) Anemia and blood transfusion in critically ill patients. JAMA 288:1499–1507 doi:10.1001/jama.288.12.1499
Wang J, Barke RA, Charboneau R, Loh HH, Roy S (2003) Morphine negatively regulates interferon-gamma promoter activity in activated murine T cells through two distinct cyclic AMP-dependent pathways. JBC 278:37622–37631 doi:10.1074/jbc.M301224200
Wang J, Barke RA, Charboneau R, Roy S (2005) Morphine impairs host innate immune response and increases susceptibility to Streptococcus pneumoniae lung infection. J Immunol 174:426–434
Wang J, Barke RA, Roy S (2007) Transcriptional and epigenetic regulation of interleukin-2 gene in activated T cells by morphine. JBC 282:7164–7171 doi:10.1074/jbc.M604367200
Watling SM, Dasta JF, Seidl EC (1997) Sedatives, analgesics and paralytics in the ICU. Ann Pharmacother 31:148–153
Weinbroum AA, Halpern P, Rudick V, Sorkine P, Freedman M, Geller E (1997) Midazolam versus propofol for long-term sedation in the ICU: a randomized prospective comparison. Intensive Care Med 23:1258–1263 doi:10.1007/s001340050495
Weinert C, Calvin A (2007) Epidemiology of sedation for mechanically ventilated patients. Crit Care Med 35:393–401 doi:10.1097/01.CCM.0000254339.18639.1D
Weinert C, Chlan L (2001) Sedating critically ill patients: factors affecting nurses’ delivery of sedative therapy. Am J Crit Care 10:156–167
Weiss M, Mirow N, Birkhahn A, Schneider M, Wernet P (1993) Benzodiazepines and their solvents influence neutrophil granulocyte function. Br J Anaesth 70:317–321 doi:10.1093/bja/70.3.317
Welters ID, Menzebach A, Goumon Y, Cadet P, Menges T, Hughes TK et al (2000a) Morphine inhibits NF-kappaB nuclear binding in human neutrophils and monocytes by a nitric oxide-dependent mechanism. Anesthesiology 92:1677–1684 doi:10.1097/00000542-200006000-00027
Welters ID, Menzebach A, Goumon Y, Langefeld TW, Teschemacher H, Hempelmann G et al (2000b) Morphine suppresses complement receptor expression, phagocytosis, and respiratory burst in neutrophils by a nitric oxide and mu(3) opiate receptor-dependent mechanism. J Neuroimmunol 111:139–145 doi:10.1016/S0165-5728(00)00401-X
Wolthuis EK, Veelo DP, Choi G, Determann RM, Korevaar JC, Spronk PE et al (2007) Mechanical ventilation with lower tidal volumes does not influence the prescription of opioids or sedatives. Crit Care 11:R77 doi:10.1186/cc5969
Yardeni IZ, Beilin B, Mayburd E, Alcalay Y, Bessler H (2008) Relationship between fentanyl dosage and immune function in the postoperative period. J Opioid Manag 4:27–33
Author information
Authors and Affiliations
Corresponding author
Additional information
Grant support for S Roy: NIH RO1 DA12104, RO1 DA022935, KO2 DA015349, P50 DA11806, and T32 DA0709 (codirector). Presented in a shortened version as an oral presentation at the Society for Neuroimmune Pharmacology meeting in Charleston, SC, USA in March 2008.
Rights and permissions
About this article
Cite this article
Weinert, C.R., Kethireddy, S. & Roy, S. Opioids and Infections in the Intensive Care Unit Should Clinicians and Patients be Concerned?. J Neuroimmune Pharmacol 3, 218–229 (2008). https://doi.org/10.1007/s11481-008-9124-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11481-008-9124-4