Abstract
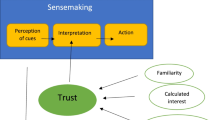
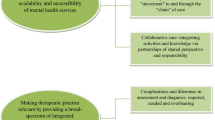
Objective To develop understandings of the nature and influence of trust in the safe management of medication within mental health services. Setting Mental health services in the UK. Method Qualitative methods were applied through focus groups across three different categories of service user—older adult, adults living in the community and forensic services. An inductive thematic analysis was carried out, using the method of constant comparison derived from grounded theory. Main Outcome Measure Participants’ views on the key factors influencing trust and the role of trust in safe medication management. Results The salient factors impacting trust were: the therapeutic relationship; uncertainty and vulnerability; and social control. Users of mental health services may be particularly vulnerable to adverse events and these can damage trust. Conclusion Safe management of medication is facilitated by trust. However, this trust may be difficult to develop and maintain, exposing service users to adverse events and worsening adherence. Practice and policy should be oriented towards developing trust.
Similar content being viewed by others

References
Möllering G. Trust: reason, routine and reflexivity. Oxford: Elsevier. 2006. ISBN 0080448550.
Hall MA, Dugan E, Zheng B, Mishra AK. Trust in physicians and medical institutions: what is it, can it be measured and does it matter. Milbank Q. 2001;79:613–39.
Calnan M, Rowe R, Entwistle V. Trust relations in health care: an agenda for future research. J Health Organ Manag. 2006;20:477–84.
Entwistle VA, Quick O. Trust in the context of patient safety problems. J Health Organ Manag. 2006;20:397–416.
Brown P, Calnan M, Scrivener A, Szmukler G. Trust in mental health services: a neglected concept. J Mental Health. 2009;18:449–58.
Mechanic D, Meyer S. Concepts of trust among patients with serious illness. Soc Sci Med. 2000;51:657–68.
Nunes V, Neilson J, O’Flynn N et al. Clinical guidelines and evidence review for medicines adherence: involving patients in decisions about prescribed medicines and supporting adherence. London: National Collaborating Centre for Primary Care and Royal College of General Practitioners. 2009. Available on http://www.nice.org.uk/nicemedia/pdf/CG76FullGuideline.pdf. Accessed 7 Mar 2011.
Seale C, Chaplin R, Lelliott P, Quirk A. Sharing decisions in consultations involving anti-psychotic medication: a qualitative study of psychiatrists’ experiences. Soc Sci Med. 2006;62:2861–73.
Safran DG, Taira DA, Rogers WH, Kosinski M, Ware JE, Tarlov AR. Linking primary care performance to outcomes of care. J Fam Pract. 1998;47:213–20.
EMERGE (Erice Medication Errors Research Group). Medication errors: problems and recommendations from a consensus meeting. Br J Clin Pharmacol. 2009;67:592–8.
Vassilev I, Pilgrim D. Risk, trust and mental health services. J Mental Health. 2007;16:347–57.
Maidment ID, Paton C, Lelliott P. A review of medication errors in mental health care. Qual Saf Health Care. 2006;15:409–13.
Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19:349–57.
Buston K, Parry-Jones W, Livingston M, Bogan A, Wood S. Qualitative Research. Br J Psychiatry. 1998;172:197–9.
Department of Health. No health without mental health: a cross-government mental health outcomes strategy for people of all ages. London. Department of Health. 2011. http://www.dh.gov.uk/en/Publicationsandstatistics/Publications/PublicationsPolicyAndGuidance/DH_123766. Accessed 7 Mar 2011.
Department of Health. Mental health national service framework (and the NHS Plan) workforce planning, education and training underpinning programme: adult mental health services: final report by the workforce action team special report. London: Department of Health. 2011. http://www.dh.gov.uk/prod_consum_dh/groups/dh_digitalassets/@dh/@en/documents/digitalasset/dh_4058912.pdf. Accessed 7 Mar 2011.
Charmaz K. Constructing grounded theory—a practical guide through qualitative analysis. London: Sage Publications; 2006. ISBN 9780761973539.
Wilder CM, Elbogen EB, Moser LL, Swanson JW, Swartz MS. Medication preferences and adherence among individuals with severe mental illness and psychiatric advance directives. Psychiatr Serv. 2010;61:380–5.
Maidment ID, Haw C, Stubbs J, Fox C, Katona C, Franklin BD. Medication errors in older people with mental health problems: a review. Int J Geriatr Psychiatry. 2008;23:564–73.
Brownlie J, Howson A. Leaps of faith and MMR: an empirical study of trust. Sociology. 2005;39:221–39.
Kadam UT, Croft P, McLeod J, Hutchinson M. A qualitative study of patients’ views on anxiety and depression. Br J Gen Pract. 2001;51:375–80.
Warner L, on behalf the Sainsbury Centre for Mental Health. Briefing 21—choice in mental health care. 2006. Available on http://www.scmh.org.uk/pdfs/briefing31_choice_in_mental_health_care.pdf. Assessed on 7 Mar 2011.
Goodwin S. Independence, risk and compulsion: conflicts in mental health policy. Soc Pol Admin. 1997;31:260–73.
Altice FL, Mostashari F, Friedland GH. Trust and the acceptance of and adherence to antiretroviral therapy. J Acquir Immune Defic Syndr. 2001;28:47–58.
Bollini P, Tibaldi G, Testa C, Munizza C. Understanding treatment adherence in affective disorders: a qualitative study. J Psychiatr Ment Health Nurs. 2004;11:668–74.
Fogarty JS. Reactance theory and patient non-compliance. Soc Sci Med. 1997;45:1277–88.
Sellwood W, Tarrier N. Reactance and treatment compliance in schizophrenia. Acta Psych Scand. 2002;106:s 413. doi:10.1034/j.1600-0447.106.s413.1_127.x.
Reason J. Human error. Cambridge: University of Cambridge; 1990. ISBN—9780521314190.
Watt I, Birks Y, Entwistle V et al. Patient safety research programme PS/034—a review of strategies to promote patient involvement, a study to explore patient’s views and attitudes and a pilot study to evaluate the acceptability of selected patient involvement strategies. University of York, May 2009. Available on—http://www.haps.bham.ac.uk/publichealth/psrp/documents/PS034_-_Final_report_2009.pdf. Accessed 9 Mar 2011.
Acknowledgments
We acknowledge the co-operation of service users from Kent and Medway NHS and Social Care Partnership Trust in this research project.
Funding
None.
Conflicts of interest
IM has undertaken consultancy for pharmaceutical companies that produce medication used within mental health services including Eli Lilly, BMS, Lundbeck, Servier and Astra Zenecca. PB and MC none.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix
Focus group semi-structured interview guide
-
Do you feel able to talk openly to your clinicians and tell them accurate and complete information about your medication?
-
Are you told the important potential adverse events?
-
When the adverse events of medication are discussed are your views listened to within the consultation?
-
Do you think that your clinicians give you a balanced picture about the risks, including adverse events, and benefits of treatment?
-
Have you ever received medication against your will? If yes, what impact did this have on your relationship with clinicians?
-
Have you ever come across a medication error in mental health?
-
How important do you think trust is in ensuring the safe use of medication?
-
Do you trust your clinicians to tell you the truth about medication?
-
Does trust, in relation to the use of medicines, exist in mental health?
-
What does it mean for you to trust your doctor about medication?
Rights and permissions
About this article
Cite this article
Maidment, I.D., Brown, P. & Calnan, M. An exploratory study of the role of trust in medication management within mental health services. Int J Clin Pharm 33, 614–620 (2011). https://doi.org/10.1007/s11096-011-9510-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-011-9510-5