Abstract
Objective
To estimate the extent, prevalence, and trends in non-prescription antibiotic use in Hungary between 2000 and 2004 at national and regional levels. To identify determinants of nonprescription antibiotic use.
Method
Data on non-prescription sales of systemic antibiotics (Anatomical Therapeutic Chemical (ATC) class J01) were analyzed over a five-year period. The 2004 version of the World Health Organisation ATC/defined daily dose (DDD) methodology was used to quantify antibiotic consumption. Non-prescription antibiotic sales were expressed as number of DDD per 1,000 inhabitants per day and as a percentage (%) of total antibiotic use. Further measurement units were introduced for better understanding of consumption and to seek an association between price, prescription antibiotic use, and non-prescription antibiotic use.
Results
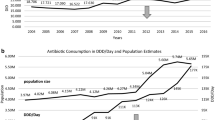
During the study period nationwide non-prescription sales of antibiotics increased threefold and reached nearly 2% prevalence in 2004. Substantial interregional differences were detected in both the level and the share of non-prescription antibiotics sales. Ten drugs were responsible for 90% of non-prescription antibiotic sales in 2004 (doxycyline, co-amoxiclav, co-trimoxazole, penamecillin, ampicillin, amoxicillin, clindamycin, clarithromycin, norfloxacin, and cefuroxime); of these, doxycycline was the number one nonprescription antibiotic in all five years. A relationship was found between price and non-prescription antibiotic use (R = −0.732, P = 0.016).
Conclusion
Despite the prescription-only status of antibiotics in Hungary, non-prescription sales occur. A further increase in non-prescription sales of antibiotics could be prevented by strict law enforcement, price augmentation, and intervention focusing on pharmacist and the general public. More detailed studies are needed to identify other sources and causes of self-medication.

Similar content being viewed by others
References
Bronzwaer SL, Cars O, Buchholz U, Molstad S, Goettsch W, Veldhuijzen IK, et al. A European study on the relationship between antimicrobial use and antimicrobial resistance. Emerg Infect Dis. 2002;8(3):278–82.
Goossens H, Ferech M, Vander Stichele R, Elseviers M. Outpatient antibiotic use in Europe and association with resistance: a cross-national database study Lancet 2005;365(9459):579–87.
Bojalil R, Calva JJ. Antibiotic misuse in diarrhea. A household survey in a Mexican community. J Clin Epidemiol. 1994;47(2):147–56.
Okumura J, Wakai S, Umenai T. Drug utilisation and self-medication in rural communities in Vietnam Soc Sci Med. 2002;54(12):1875–86.
Grigoryan L, Haaijer-Rysjamp FM, Burgerhof JG, Mechtler R, Deschepper R, Tambic-Andrasevic A, et al. Self-medication with antimicrobial drugs in Europe. Emerg Infect Dis. 2006;12(3):452–9.
Simon T. Antibiotics in households. Gyógyszereink 1997;47:177–80. Hungarian.
Grigoryan L, Burgerhof JG, Haaijer-Ruskamp FM, Degener JE, Deschepper R, Monnet DL, et al. Is self-medication with antibiotics in Europe driven by prescribed use? J Antimicrob Chemother. 2007;59(1):152–6.
Svensson E, Haaijer-Ruskamp FM, Lundborg CS. Self-medication with antibiotics in a Swedish general population. Scand J Infect Dis. 2004;36(6–7):450–2.
Muscat M, Monnet DL, Klemmensen T, Grigoryan L, Jensen MH, Andersen M, et al. Patterns of antibiotic use in the community in Denmark Scand J Infect Dis. 2006;38(8):597–603.
Acknowlegement
This study was financed by the 5N048 University Research Fund
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Matuz, M., Benko, R., Doro, P. et al. Non-prescription antibiotic use in Hungary. Pharm World Sci 29, 695–698 (2007). https://doi.org/10.1007/s11096-007-9132-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-007-9132-0