Abstract
Purpose
The goal of this study was to assess the rehabilitation needs of young women breast cancer survivors under the age of 50 and to identify factors that may impact or prevent cancer rehabilitation utilization.
Methods
Utilizing a grounded theory methodology, 35 young breast cancer survivors were interviewed twice in four Atlantic Canadian provinces.
Results
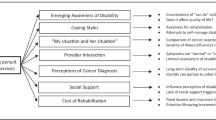
A considerable number of barriers exist to receiving rehabilitative care post-treatment for young breast cancer survivors. The systemic barriers include the lack of availability of services, travel issues, cost of services, and the lack of support to address the unique needs for this age group. However, the most complicated barriers to accessing rehabilitative care were personal barriers which related more to choice and circumstances, such as the lack of time due to family responsibilities and appointment fatigue. Many of these personal barriers were rooted in the complex set of gender roles of young women as patients, mothers, workers, and caregivers.
Conclusions
The contexts of young women’s lives can have a substantial impact on their decisions to seek and receive rehabilitative care after breast cancer treatment. The systemic barriers can be reduced by introducing more services or financial assistance; however, the personal barriers to rehabilitation services are difficult to ameliorate due to the complex set of roles within and outside the family for this group of young breast cancer survivors. Health care providers need to take into consideration the multiple contexts of women’s lives when developing and promoting breast cancer rehabilitation services and programs.

Similar content being viewed by others
References
Rejeneration: Mobile Cancer Rehabilitation (2011) http://rejeneration.ca/customized-cancer-rehabilitation-program. Accessed on March 31, 2011
Avis NE, Crawford S, Manuel J (2005) Quality of life among younger women with breast cancer. J Clin Oncol 23:3322–3330
Aziz NM (2007) Cancer survivorship research: state of knowledge, challenges and opportunities. Acta Oncol 46:417–432
Beattie A (2009) Detecting breast cancer in a general practice—like finding needles in a haystack? Aust Fam Physician 38:1003–1006
Bosompra K, Ashikaga T, O’Brien PJ, Nelson L, Skelly J (2002) Swelling, numbness, pain, and their relationship to arm function among breast cancer survivors: a disablement process model perspective. Breast J 8:338–348
Canadian Cancer Society’s Steering Committee (2010) Canadian cancer statistics 2010. Canadian Cancer Society, Toronto
Canadian Cancer Society’s Steering Committee (2007) Canadian cancer statistics 2007. Canadian Cancer Society, Toronto
Creswell JW (1997) Qualitative inquiry and research design: choosing among five traditions. Sage, London
DeLisa JA (2001) A history of cancer rehabilitation. Cancer 92(Suppl):970–974
Dunn J, Steginga SK (2000) Young women’s experience of breast cancer: defining young and identifying concerns. Psychooncology 9:137–146
Fitch MI, Allard M (2007) Perspectives of husbands of women with breast cancer: impact and response. Can Oncol Nurs J 17:66–78
Fors EA, Bertheussen GF, Thune I, Juvet LK, Elvsaas IK, Oldervoll L, Anker G, Falkmer U, Lundgren S, Leivseth G (2010) Psychosocial interventions as part of breast cancer rehabilitation programs? Results from a systematic review. Psychooncology. doi:10.1002/pon.1844
Ganz PA, Greendale GA, Petersen L, Kahn B, Bower JE (2003) Breast cancer in younger women: reproductive and late health effects of treatment. J Clin Oncol 21:4184–4193
Gerber LH (2001) Cancer rehabilitation into the future. Cancer 92:975–979
Grunfeld E (2009) Optimizing follow-up after breast cancer treatment. Curr Opin Obstet Gynecol 21:92–96
Hewitt M, Greenfield S, Stovall E (2006) From cancer patient to cancer survivor: lost in transition. National Academies, Washington, DC
Hurny C, Bernhard J, Coates AS, Castiglione-Gertsch M, Peterson HF, Gelber RD, Forbes JF, Rudenstam CM, Simoncini E, Crivellari D, Goldhirsch A, Senn HJ (1996) Impact of adjuvant therapy on quality of life in women with node-positive operable breast cancer. International Breast Cancer Study Group. Lancet 347:1279–1284
Jenkins CL (1997) Women, work, and caregiving: how do these roles affect women’s well-being? J Women Aging 9:27–45
Johansen C (2007) Rehabilitation of cancer patients—research perspectives. Acta Oncol 46:441–445
Johnsson A, Tenenbaum A, Westerlund H (2011) Improvements in physical and mental health following a rehabilitation programme for breast cancer patients. Eur J Oncol Nurs 15(1):12–15
Kornblith AB, Powell M, Regan MM, Bennett S, Krasner C, Moy B, Younger J, Goodman A, Berkowitz R, Winer E (2007) Long-term psychosocial adjustment of older vs younger survivors of breast and endometrial cancer. Psychooncology 16:895–903
Kroenke CH, Rosner B, Chen WY, Kawachi I, Colditz GA, Holmes MD (2004) Functional impact of breast cancer by age at diagnosis. J Clin Oncol 22:1849–1856
Luker KA, Beaver K, Leinster SJ, Owens RG (1996) Meaning of illness for women with breast cancer. J Adv Nurs 23:1194–1201
Lundgren H, Bolund C (2007) Body experience and reliance in some women diagnosed with cancer. Cancer Nurs 30:16–23
Miedema B, Hamilton R, Easley J (2007) From “invincibility” to “normalcy”: coping strategies of young adults during the cancer journey. Palliat Support Care 5:41–49
Moen P, Robinson J, Dempster-McClain D (1995) Caregiving and women’s well-being: a life course approach. J Health Soc Behav 36:259–273
Mongabay World Statistics (2011) http://www.mongabay.com/igapo/world_statistics_by_area.htm. Accessed on March 31, 2011
National Rehabilitation Hospital (2011) Breast cancer rehabilitation. http://www.nrhrehab.org/Patient+Care/Programs+and+Service+Offerings/Outpatient+Services/Service_Page.aspx?id=10. Accessed on March 31, 2011
Revenson TA, Pranikoff JR (2005) A contextual approach to treatment decision making among breast cancer survivors. Health Psychol 24:S93–S98
Ronson A, Body JJ (2002) Psychosocial rehabilitation of cancer patients after curative therapy. Support Care Cancer 10:281–291
Semple CJ, McCance T (2010) Parents’ experience of cancer who have young children: a literature review. Cancer Nurs 33:110–118
Shannon C, Smith IE (2003) Breast cancer in adolescents and young women. Eur J Cancer 39:2632–2642
Statisics Canada (2009) Population urban and rural by province and teritory. Available from http://www40.statcan.ca/l01/cst01/demo62a-eng.htm. Accessed on March 31, 2011
Thibodeau J, MacRae J (1997) Breast cancer survival: a phenomenological inquiry. ANS Adv Nurs Sci 19:65–74
Thomas-MacLean R, Miedema B, Tatemichi SR (2005) Breast cancer-related lymphedema: women’s experiences with an underestimated condition. Can Fam Physician 51:246–247
Thomas DC, Ragnarsson KT (2009) Principles of cancer rehabilitation medicine. In: Hong WK, BastJr RC, Hait WN, Kufe DW, Pollock RE, Weichselbaum RR, Gansler TS, Holland JF, Frei E III (eds) Holland-Frei cancer medicine. People’s Medical, Shelton, CT
Vanhuyse M, Bedard PL, Sheiner J, Fitzgerald B, Clemons M (2007) Transfer of follow-up care to family physicians for early-stage breast cancer. Clin Oncol (R Coll Radiol) 19:172–176
Wenzel LB, Fairclough DL, Brady MJ, Cella D, Garrett KM, Kluhsman BC, Crane LA, Marcus AC (1999) Age-related differences in the quality of life of breast carcinoma patients after treatment. Cancer 86:1768–1774
Yankaskas BC (2005) Epidemiology of breast cancer in young women. Breast Dis 23:3–8
Acknowledgements
We would like to thank Naomi Tschirhart, Tashina Van Vlack, and Miles Clayden for their assistance with this project. Financial support for the study was provided by the Canadian Breast Cancer Foundation—Atlantic Chapter.
Conflicts of interest
The authors have no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Miedema, B., Easley, J. Barriers to rehabilitative care for young breast cancer survivors: a qualitative understanding. Support Care Cancer 20, 1193–1201 (2012). https://doi.org/10.1007/s00520-011-1196-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-011-1196-7