Abstract
Purpose
This study examined symptoms reported by patients after open-ended questioning vs those systematically assessed using a 48-question survey.
Materials and methods
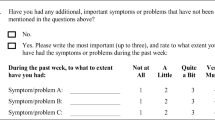
Consecutive patients referred to the palliative medicine program at the Cleveland Clinic Foundation were screened. Open-ended questions were asked initially followed by a 48-item investigator-developed symptom checklist. Each symptom was rated for severity as mild, moderate, or severe. Symptom distress was also evaluated. Data were collected using standardized pre-printed forms.
Results
Two hundred and sixty-five patients were examined and 200 were eligible for assessment. Of those assessed, the median age was 65 years (range 17–90), and median ECOG performance status was 2 (range 1–4). A total of 2,397 symptoms were identified, 322 volunteered and 2,075 by systematic assessment. The median number of volunteered symptoms was one (range zero to six). Eighty-three percent of volunteered symptoms were moderate or severe and 17% mild. Ninety-one percent were distressing. Fatigue was the most common symptom identified by systematic assessment but pain was volunteered most often. The median number of symptoms found using systematic assessment was ten (0–25). Fifty-two percent were rated moderate or severe and 48% mild. Fifty-three percent were distressing. In total, 69% of 522 severe symptoms and 79% of 1,393 distressing symptoms were not volunteered. Certain symptoms were more likely to be volunteered; this was unaffected by age, gender, or race.
Conclusion
The median number of symptoms found using systematic assessment was tenfold higher (p<0.001) than those volunteered. Specific detailed symptom inquiry is essential for optimal palliation in advanced disease.




Similar content being viewed by others
References
Jemal A, Thomas A, Murray T, Thun M (2002) Cancer statistics. CA Cancer J Clin 52:181–182
Ingham JM, Portenoy RK (1996) Symptom assessment. Hematol Oncol Clin North Am 10(1):21–39
Donnelly S, Walsh D, Rybicki L (1995) The symptoms of advanced cancer: identification of clinical and research priorities by assessment of prevalence and severity. J Palliat Care 11(1):27–32
Donnelly S, Walsh D (1995) The symptoms of advanced cancer. Semin Oncol 22(2 Suppl 3):67–72
Walsh D, Donnelly S, Rybicki L (2000) The symptoms of advanced cancer: relationship to age gender and performance status in 1,000 patients. Supportive Care Cancer 8:175–179
Simel DL (2004) Approach to the patient: history and physical examination. In: Goldman L, Ausiello D (eds) Cecil textbook of medicine, 22nd edn. WB Saunders, Phildelphia, PA, pp 18–23
Stillman MJ, Rybicki LA (2000) The bedside confusion scale: development of a portable bedside test for confusion and its application to the palliative medicine population. J Palliat Med 3(4):449–456
Sprangers MA, Aaronson NK (1992) The role of health care providers and significant others in evaluating the quality of life of patients with chronic disease: a review. J Clin Epidemiol 45(7):743–760
Stromgren AS, Groenvold M, Pedersen L, Olsen AK, Spile M, Sjogren P (2001) Does the medical record cover the symptoms experienced by cancer patients receiving palliative care? A comparison of the record and patient self-rating. J Pain Symptom Manage 21(3):189–196
Stromgren AS, Groenvold M, Sorensen A, Andersen L (2001) Symptom recognition in advanced cancer. A comparison of nursing records against patient self-rating. Acta Anaesthesiol Scand 45(9):1080–1085
Portenoy RK, Thaler HT, Kornblith AB, Lepore JM, Friedlander-Klar H, Kiyasu E et al (1994) The Memorial Symptom Assessment Scale: an instrument for the evaluation of symptom prevalence, characteristics and distress. Eur J Cancer 30A(9):1326–1336
Zobora J, BrintzenhofeSzoc K, Jacobsen P, Curbow B, Piantadosi S, Hooker C et al (2001) A new psychosocial screening instrument for use with cancer patients. Psychosomatics 42(31):241–246
Heedman PA, Strang P (2001). Symptom assessment in advanced palliative home care for cancer patients using the ESAS: clinical aspects. Anticancer Res 21(6A):4077–4082
Bruera E, Kuehn N, Miller MJ, Selmser P, Macmillan K (1991) The Edmonton Symptom Assessment System (ESAS): a simple method for the assessment of palliative care patients. J Palliat Care 7:6–9
Cleeland CS, Mendoza TR, Wang XS, Chou C, Harle MT, Morrissey M et al (2000) Assessing symptom distress in cancer patients: the M.D. Anderson Symptom Inventory. Cancer 89(7):1634–1646
de Haes JC, van Knippenberg FC, Neijt JP (1990) Measuring psychological and physical distress in cancer patients: structure and application of the Rotterdam Symptom Checklist. Br J Cancer 62:1034–1038
Caraceni A, Cherny N, Fainsinger R, Kaasa S, Poulain P, Radbruch L et al (2002) Pain measurement tools and methods in clinical research in palliative care: recommendations of an expert working group of the European Association of Palliative Care. J Pain Symptom Manage 23(3):239–255
Lloyd-Williams M (2001) Screening for depression in palliative care patients: a review. Eur J Cancer 10(1):31–35
Kaasa S, Loge JH, Knobel H, Jordhoy MS, Brenne E (1999) Fatigue. Measures and relation to pain. Acta Anaesthesiol Scand 43(9):939–947
Lloyd-Williams M, Freidman T, Rudd N (2001) An analysis of the validity of the Hospital Anxiety and Depression scale as a screening tool in patients with advanced metastatic cancer. J Pain Symptom Manage 22:990–996
Stromgren AS, Groenvold M, Pedersen L, Olsen AK, Sjogren P (2002) Symptomatology of cancer patients in palliative care: content validation of self-assessment questionnaires against medical records. Eur J Cancer 38(6):788–794
Massie MJ, Popkin MK (1998) Depression. In: Holland J, Rowland J (eds) Handbook of psychooncology. Oxford University Press, New York, pp 518–540
Walsh D, Rybicki L, Nelson KA, Donnelly S (2002) Symptoms and prognosis in advanced cancer. Support Care Cancer 10:385–388
Homsi J, Walsh D, Nelson KA, LeGrand SB, Davis M, Khawam E, Nouneh C (2002) The impact of a palliative medicine consultation service in medical oncology. Support Care Cancer 10(4):337–342
Ward SE, Goldberg N, Miller-McCauley V, Mueller C, Nolan A, Pawlik-Plank D et al (1993) Patient-related barriers to management of cancer pain. Pain 52(3):319–324
Levin DN, Cleeland CS, Dar R (1985) Public attitudes toward cancer pain. Cancer 56(9):2337–2339
Cleeland CS (1987) Barriers to the management of cancer pain. Oncology (Huntingt) 1(2 Suppl):19–26
Diekmann JM, Engber D, Wassem R (1989) Cancer pain control: one state's experience. Oncol Nurs Forum 16(2):219–223
Mann E, Redwood S (2000) Improving pain management: breaking down the invisible barrier. Br J Nurs 9(19):2067–2072
Miaskowski C, Dodd MJ, West C, Paul SM, Tripathy D, Koo P et al (2001) Lack of adherence with the analgesic regimen: a significant barrier to effective cancer pain management. J Clin Oncol 19(23):4275–4279
de Haes JCJM, van Knippenberg FCE, Neijt JP (1990) Measuring psychosocial and physical distress in cancer patients: structure and application of the Rotterdam Symptom Checklist. Br J Cancer 62(6):1034–1038
Portenoy RK, Thaler HT, Kornblith AB, McCarthy Lepore J, Friedlander-Klar H, Kiyasu E, Sobel K, Coyle N, Kemeny N, Norton L, Scher H (1994) The Memorial Symptom Assessment Scale: an instrument for the evaluation of symptom prevalence, characteristics and distress. Eur J Cancer 30A(9):1326–1336
Slevin ML, Plant H, Lynch D, Drinkwater K, Gregory WM (1988) Who should measure quality of life, the doctor or the patient? Br J Cancer 57:109–112
Author information
Authors and Affiliations
Corresponding author
Additional information
The Harry R. Horvitz Center for Palliative Medicine is a World Health Organization demonstration project in palliative medicine
Rights and permissions
About this article
Cite this article
Homsi, J., Walsh, D., Rivera, N. et al. Symptom evaluation in palliative medicine: patient report vs systematic assessment. Support Care Cancer 14, 444–453 (2006). https://doi.org/10.1007/s00520-005-0009-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00520-005-0009-2