Abstract
Purpose
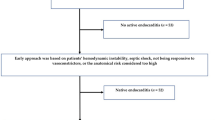
We compared early results of homograft aortic root replacement (ARR) in native (NVE) and prosthetic (PVE) aortic valve endocarditis in order to identify predictors for early mortality (<30 days).
Methods
Between 05/1986 and 12/2007, 1,163 endocarditis patients were operated upon. Of these, 221 patients (n = 185 men, median age 55 years) underwent homograft ARR due to 99 cases of NVE (45%) and 122 of PVE (55%) aortic root endocarditis. Demographics, clinical differences, survival rates and predictors of early mortality were analyzed. Follow-up (mean 5.2 ± 0.4 years, maximum 18.4 years) was completed in 96.8% with a total of 1,127 patient years.
Results
Main causes of the 47 (21.2%) early deaths were septic multiorgan failure in 23 (48.9%) and myocardial failure in 10 (21.3%) patients with a significantly better survival for NVE than for PVE patients (patients = 0.029). The highest ORs were found in the univariate analysis for preoperative development of septic shock (OR 14.28), preoperative necessity of ventilation (OR 7.08), high doses of catecholamines (OR 5.60), severe aortic root destruction (OR 5.12), emergency operation (OR 4.25) and persistent fever despite antibiotic treatment (OR 4.11). Multivariate analysis showed that preoperative ventilation (OR 5.43), persistent fever under antibiotic treatment (OR 2.84) and prosthetic endocarditis (OR 2.32) were independent risk factors for early mortality.
Conclusions
Our results suggest that early outcome could be improved if patients were referred earlier for surgery. A multidisciplinary approach is necessary, involving at least specialists in intensive care medicine, cardiology, infectious disease and cardiac surgery in order to identify the optimal time for surgery and decrease early mortality.

Similar content being viewed by others
Abbreviations
- ARR:
-
Aortic root replacement
- AIE:
-
Active infective endocarditis
- CI:
-
Confidence interval
- ICU:
-
Intensive care unit
- MOF:
-
Multiorgan failure
- NVE:
-
Native valve endocarditis
- OR:
-
Odds ratio
- POD:
-
Postoperative day
- PVE:
-
Prosthetic valve endocarditis
References
Tornos P, Iung B, Permanyer-Miralda G, Baron G, Delahaye F, Gohlke-Barwolf C, Butchart EG, Ravaud P, Vahanian A (2005) Infective endocarditis in Europe: lessons from the Euro heart survey. Heart 91:571–575
Hoen B, Alla F, Selton-Suty C, Beguinot I, Bouvet A, Briancon S, Casalta JP, Danchin N, Delahaye F, Etienne J, Le Moing V, Leport C, Mainardi JL, Ruimy R, Vandenesch F (2002) Changing profile of infective endocarditis: results of a 1-year survey in France. Jama 288:75–81
Cabell CH, Abrutyn E, Fowler VG Jr, Hoen B, Miro JM, Corey GR, Olaison L, Pappas P, Anstrom KJ, Stafford JA, Eykyn S, Habib G, Mestres CA, Wang A (2005) Use of surgery in patients with native valve infective endocarditis: results from the International Collaboration on Endocarditis Merged Database. Am Heart J 150:1092–1098
Anguera I, Miro JM, San Roman JA, de Alarcon A, Anguita M, Almirante B, Evangelista A, Cabell CH, Vilacosta I, Ripoll T, Munoz P, Navas E, Gonzalez-Juanatey C, Sarria C, Garcia-Bolao I, Farinas MC, Rufi G, Miralles F, Pare C, Fowler VG Jr, Mestres CA, de Lazzari E, Guma JR, del Rio A, Corey GR (2006) Periannular complications in infective endocarditis involving prosthetic aortic valves. Am J Cardiol 98:1261–1268
Habib G, Thuny F, Avierinos JF (2008) Prosthetic valve endocarditis: current approach and therapeutic options. Prog Cardiovasc Dis 50:274–281
Hill EE, Herregods MC, Vanderschueren S, Claus P, Peetermans WE, Herijgers P (2008) Outcome of patients requiring valve surgery during active infective endocarditis. Ann Thorac Surg 85:1564–1569
Yankah AC, Pasic M, Klose H, Siniawski H, Weng Y, Hetzer R (2005) Homograft reconstruction of the aortic root for endocarditis with periannular abscess: a 17-year study. Eur J Cardiothorac Surg 28:69–75
Lund O, Chandrasekaran V, Grocott-Mason R, Elwidaa H, Mazhar R, Khaghani A, Mitchell A, Ilsley C, Yacoub MH (1999) Primary aortic valve replacement with allografts over twenty-five years: valve-related and procedure-related determinants of outcome. J Thorac Cardiovasc Surg 117:77–90 (Discussion 1)
Wang A, Pappas P, Anstrom KJ, Abrutyn E, Fowler VG Jr, Hoen B, Miro JM, Corey GR, Olaison L, Stafford JA, Mestres CA, Cabell CH (2005) The use and effect of surgical therapy for prosthetic valve infective endocarditis: a propensity analysis of a multicenter, international cohort. Am Heart J 150:1086–1091
Tugtekin SM, Alexiou K, Wilbring M, Daubner D, Kappert U, Knaut M, Matschke K (2006) Native infective endocarditis: which determinants of outcome remain after surgical treatment? Clin Res Cardiol 95:72–79
Musci M, Siniawski H, Knosalla C, Grauhan O, Weng Y, Pasic M, Meyer R, Hetzer R (2006) Early and mid-term results of the Shelhigh stentless bioprosthesis in patients with active infective endocarditis. Clin Res Cardiol 95:247–253
David TE, Gavra G, Feindel CM, Regesta T, Armstrong S, Maganti MD (2007) Surgical treatment of active infective endocarditis: a continued challenge. J Thorac Cardiovasc Surg 133:144–149
Moon MR, Miller DC, Moore KA, Oyer PE, Mitchell RS, Robbins RC, Stinson EB, Shumway NE, Reitz BA (2001) Treatment of endocarditis with valve replacement: the question of tissue versus mechanical prosthesis. Ann Thorac Surg 71:1164–1171
O’Brien MF, Harrocks S, Stafford EG, Gardner MA, Pohlner PG, Tesar PJ, Stephens F (2001) The homograft aortic valve: a 29-year, 99.3% follow up of 1,022 valve replacements. J Heart Valve Dis 10:334–344 (Discussion 5)
Schmidtke C, Dahmen G, Sievers HH (2007) Subcoronary Ross procedure in patients with active endocarditis. Ann Thorac Surg 83:36–39
Bonow RO, Carabello BA, Kanu C, de Leon AC, Jr., Faxon DP, Freed MD, Gaasch WH, Lytle BW, Nishimura RA, O’Gara PT, O’Rourke RA, Otto CM, Shah PM, Shanewise JS, Smith SC Jr, Jacobs AK, Adams CD, Anderson JL, Antman EM, Fuster V, Halperin JL, Hiratzka LF, Hunt SA, Nishimura R, Page RL, Riegel B (2006) ACC/AHA 2006 guidelines for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (writing committee to revise the 1998 Guidelines for the Management of Patients With Valvular Heart Disease): developed in collaboration with the Society of Cardiovascular Anesthesiologists: endorsed by the Society for Cardiovascular Angiography and Interventions and the Society of Thoracic Surgeons. Circulation 114:e84–e231
Horstkotte D, Follath F, Gutschik E, Lengyel M, Oto A, Pavie A, Soler-Soler J, Thiene G, von Graevenitz A, Priori SG, Garcia MA, Blanc JJ, Budaj A, Cowie M, Dean V, Deckers J, Fernandez Burgos E, Lekakis J, Lindahl B, Mazzotta G, Morais J, Smiseth OA, Vahanian A, Delahaye F, Parkhomenko A, Filipatos G, Aldershvile J, Vardas P (2004) Guidelines on prevention, diagnosis and treatment of infective endocarditis executive summary; the task force on infective endocarditis of the European Society of Cardiology. Eur Heart J 25:267–276
Aksoy O, Sexton DJ, Wang A, Pappas PA, Kourany W, Chu V, Fowler VG Jr, Woods CW, Engemann JJ, Corey GR, Harding T, Cabell CH (2007) Early surgery in patients with infective endocarditis: a propensity score analysis. Clin Infect Dis 44:364–372
Reinhartz O, Herrmann M, Redling F, Zerkowski HR (1996) Timing of surgery in patients with acute infective endocarditis. J Cardiovasc Surg (Torino) 37:397–400
Acknowledgments
We thank Mrs. A. Benhennour for bibliographic assistance, Mrs. K. Weber for photographic work and Mrs. A. Gale for editorial assistance.
Conflict of interest statement
There is no financial relationship with any corporate sponsor that might relate in any way to the subject presented.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Musci, M., Weng, Y., Hübler, M. et al. Predictors of early mortality in patients with active infective native or prosthetic aortic root endocarditis undergoing homograft aortic root replacement. Clin Res Cardiol 98, 443–450 (2009). https://doi.org/10.1007/s00392-009-0015-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-009-0015-3