Abstract
Purpose
The present study established the national prevalence of substance use disorders (SUDs) among Danish psychiatric patients. Furthermore, patients with SUDs and those without SUDs were compared on a range of socio-demographic, clinical, and treatment characteristics.
Methods
Data were obtained from several Danish population-based registers. The study population was defined as all individuals with incidents of schizophrenia, schizotypal disorder, other psychoses, bipolar disorder, depression, anxiety, obsessive–compulsive disorder (OCD), post-traumatic stress disorder (PTSD), and personality disorders since 1969. The prevalence of SUDs was examined for the following psychoactive substances: alcohol, opioids, cannabis, sedatives, cocaine, psycho-stimulants and hallucinogens.
Results
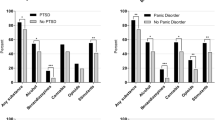
A total of 463,003 patients were included in the analysis. The prevalence of any lifetime SUD was: 37 % for schizophrenia, 35 % for schizotypal disorder, 28 % for other psychoses, 32 % for bipolar disorder, 25 % for depression, 25 % for anxiety, 11 % for OCD, 17% for PTSD, and 46 % for personality disorders. Alcohol use disorder was the most dominating SUD in every psychiatric category (25 % of all included patients). Patients with SUDs were more often men, had fewer years of formal education, more often received disability pension and died due to unnatural causes.
Conclusions
The study was the most comprehensive of its kind so far to estimate the prevalence of SUDs in an unselected population-based cohort, and it revealed remarkably high prevalence among the psychiatric patients. The results should encourage continuous focus on possible comorbidity of psychiatric patients, as well as specialised and integrated treatment along with increased support of patients with comorbid disorders.

Similar content being viewed by others
References
Wittchen HU et al (2011) The size and burden of mental disorders and other disorders of the brain in Europe 2010. Eur Neuropsychopharmacol 21(9):655–679
Kessler RC et al (2005) Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the national comorbidity survey replication. Arch Gen Psychiatry 62(6):617–627
Grant BF (1996) Prevalence and correlates of drug use and DSM-IV drug dependence in the United States: results of the national longitudinal alcohol epidemiologic survey. J Subst Abuse 8(2):195–210
Saraceno B (2002) The WHO world health report 2001 on mental health. Epidemiologia e Psichiatria Sociale 11(2):83–87
Hartz SM et al (2014) Comorbidity of severe psychotic disorders with measures of substance use. JAMA Psychiatry 71(3):248–254
Regier DA et al (1990) Comorbidity of mental disorders with alcohol and other drug abuse. Results from the epidemiologic catchment area (ECA) Study. JAMA 264(19):2511–2518
Grant BF et al (2004) Prevalence and co-occurrence of substance use disorders and independent mood and anxiety disorders: results from the national epidemiologic survey on alcohol and related conditions. Arch Gen Psychiatry 61(8):807–816
Health, U.S.D.o (2003) A. Human services substance, and a. mental health services. 2003 National survey on drug use and health. http://www.oas.samhsa.gov/nhsda/2k3nsduh/2k3results.htm. Accessed Mar 2014
Jimenez-Castro L et al (2010) Substance use disorder comorbidity with schizophrenia in families of Mexican and Central American ancestry. Schizophr Res 120(1–3):87–94
Kessler RC et al (1997) Lifetime co-occurrence of DSM-III-R alcohol abuse and dependence with other psychiatric disorders in the national comorbidity survey. Arch Gen Psychiatry 54(4):313–321
Moore E et al (2012) The impact of alcohol and illicit drugs on people with psychosis: the second Australian national survey of psychosis. Aust N Z J Psychiatry 46(9):864–878
Nesvåg R et al (2015) Substance use disorders in schizophrenia, bipolar disorder, and depressive illness: a registry-based study. Soc Psychiatry Psychiatr Epidemiol 50(8):1267–1276
Whiteford HA et al (2013) Global burden of disease attributable to mental and substance use disorders: findings from the global burden of disease study 2010. Lancet 382(9904):1575–1586
Druss BG et al (2011) Understanding excess mortality in persons with mental illness: 17-year follow up of a nationally representative US survey. Med Care 49(6):599–604
Nordentoft M et al (2013) Excess mortality, causes of death and life expectancy in 270,770 patients with recent onset of mental disorders in Denmark, Finland and Sweden. PLoS One 8(1):e55176
Parks J et al (2006) Morbidity and mortality in people with serious mental illness. http://www.wvcbhc.org/PDFs/NASMHPD_Morbidity_and_Mortality_Paper_10-06.pdf. Accessed Nov 2013
Drake RE, Brunette MF (1998) Complications of severe mental illness related to alcohol and drug use disorders. Recent Dev Alcohol 14:285–299
Zammit S et al (2008) Effects of cannabis use on outcomes of psychotic disorders: systematic review. Br J Psychiatry 193(5):357–363
Soyka M (2000) Substance misuse, psychiatric disorder and violent and disturbed behaviour. Br J Psychiatry 176:345–350
Drake RE et al (2004) A review of treatments for people with severe mental illnesses and co-occurring substance use disorders. Psychiatr Rehabil J 27(4):360–374
Moore TH et al (2007) Cannabis use and risk of psychotic or affective mental health outcomes: a systematic review. Lancet 370(9584):319–328
Macleod J et al (2004) Psychological and social sequelae of cannabis and other illicit drug use by young people: a systematic review of longitudinal, general population studies. Lancet 363(9421):1579–1588
Mueser KT, Drake RE, Wallach MA (1998) Dual diagnosis: a review of etiological theories. Addict Behav 23(6):717–734
Miles H et al (2003) Characteristics of subgroups of individuals with psychotic illness and a comorbid substance use disorder. Psychiatr Serv 54(4):554–561
Lai HM, Huang QR (2009) Comorbidity of mental disorders and alcohol- and drug-use disorders: analysis of New South Wales inpatient data. Drug Alcohol Rev 28(3):235–242
Pedersen CB (2011) The danish civil registration system. Scand J Public Health 39(7 Suppl):22–25
Mors O, Perto GP, Mortensen PB (2011) The Danish psychiatric central research register. Scand J Public Health 39(7 Suppl):54–57
World Health Organisation, WHO (2008). International classification of diseases (ICD). http://www.who.int/classifications/icd/en/. Accessed Oct 2013
Lynge E, Sandegaard JL, Rebolj M (2011) The Danish national patient register. Scand J Public Health 39(7 Suppl):30–33
The national board of social services and the ministry of social affairs (2014) Registry of drug abusers undergoing treatment. http://www.stofmisbrugsdatabasen.dk/. Accessed Oct 2013
Kildemoes HW, Sorensen HT, Hallas J (2011) The Danish national prescription registry. Scand J Public Health 39(7 Suppl):38–41
Thygesen LC et al (2011) Introduction to Danish (nationwide) registers on health and social issues: structure, access, legislation, and archiving. Scand J Public Health 39(7 Suppl):12–16
Helweg-Larsen K (2011) The Danish register of causes of death. Scand J Public Health 39(7 Suppl):26–29
Kavanagh DJ et al (2004) Demographic and clinical correlates of comorbid substance use disorders in psychosis: multivariate analyses from an epidemiological sample. Schizophr Res 66(2–3):115–124
Swendsen J et al (2010) Mental disorders as risk factors for substance use, abuse and dependence: results from the 10-year follow-up of the national comorbidity survey. Addiction 105(6):1117–1128
Hansen SS et al (2000) Psychoactive substance use diagnoses among psychiatric in-patients. Acta Psychiatr Scand 102(6):432–438
Drake RE et al (2002) Psychosocial aspects of substance abuse by clients with severe mental illness. J Nerv Ment Disease 190(2):100–106
Lembke A (2012) Time to abandon the self-medication hypothesis in patients with psychiatric disorders. Am J Drug Alcohol Abuse 38(6):524–529
Khantzian EJ (1985) The self-medication hypothesis of addictive disorders: focus on heroin and cocaine dependence. Am J Psychiatry 142(11):1259–1264
Henwood B, Padgett DK (2007) Reevaluating the self-medication hypothesis among the dually diagnosed. Am J Addict 16(3):160–165
Dixon L et al (1990) Acute effects of drug abuse in schizophrenic patients: clinical observations and patients’ self-reports. Schizophr Bull 16(1):69–79
Hvidtfeldt UA et al (2008) Alkoholforbrug i Danmark; Kvantificering og karakteristik af storforbrugere og afhængige. The National Institute of Public Health, University of Southern Denmark, Copenhagen
The Danish health and medicines authority (2012) Narkotikasituationen i Danmark 2012. Public report. http://sundhedsstyrelsen.dk/publ/Publ2012/11nov/NarkositDK2012.pdf. Accessed Oct 2013
Menezes PR et al (1996) Drug and alcohol problems among individuals with severe mental illness in south London. Br J Psychiatry 168(5):612–619
Haywood TW et al (1995) Predicting the “revolving door” phenomenon among patients with schizophrenic, schizoaffective, and affective disorders. Am J Psychiatry 152(6):856–861
Lybrand J, Caroff S (2009) Management of schizophrenia with substance use disorders. Psychiatr Clin North Am 32(4):821–833
Drake RE, Mueser KT (2000) Psychosocial approaches to dual diagnosis. Schizophr Bull 26(1):105–118
Ridgely MS, Goldman HH, Willenbring M (1990) Barriers to the care of persons with dual diagnoses: organizational and financing issues. Schizophr Bull 16(1):123–132
Curran GM et al (2008) The association of psychiatric comorbidity and use of the emergency department among persons with substance use disorders: an observational cohort study. BMC Emerg Med 8:17
Minassian A, Vilke GM, Wilson MP (2013) Frequent emergency department visits are more prevalent in psychiatric, alcohol abuse, and dual diagnosis conditions than in chronic viral illnesses such as hepatitis and human immunodeficiency virus. J Emerg Med 45(4):520–525
Drake RE, Osher FC, Wallach MA (1991) Homelessness and dual diagnosis. Am Psychol 46(11):1149–1158
Laursen TM et al (2007) Increased mortality among patients admitted with major psychiatric disorders: a register-based study comparing mortality in unipolar depressive disorder, bipolar affective disorder, schizoaffective disorder, and schizophrenia. J Clin Psychiatry 68(6):899–907
Buckley PF (2006) Prevalence and consequences of the dual diagnosis of substance abuse and severe mental illness. J Clin Psychiatry 67(Suppl 7):5–9
Acknowledgments
Nanna Gilliam Toftdahl received a grant from the Lundbeck Foundation to fund the work. The Lundbeck Foundation had no influence on the protocol, analysis, interpretation, drafting of the manuscript, decision to publish, or any other areas other than funding of the authors work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethics
Register-based analyses in Denmark do not require consent from participants or ethical approval. The protocol was approved by the Danish Data Protection Agency.
Rights and permissions
About this article
Cite this article
Toftdahl, N.G., Nordentoft, M. & Hjorthøj, C. Prevalence of substance use disorders in psychiatric patients: a nationwide Danish population-based study. Soc Psychiatry Psychiatr Epidemiol 51, 129–140 (2016). https://doi.org/10.1007/s00127-015-1104-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-015-1104-4