Abstract
Objective
Opinions differ whether the rate of spontaneous preterm delivery (sPTD) increases in pregnancies complicated with GDM. We sought to characterize, which factors may influence the rate of sPTD in GDM.
Methods
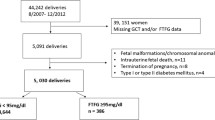
We conducted a retrospective study with 1,526 GDM patients, all treated at the same center by the same diabetic protocol using self-blood glucose monitoring. The rate of sPTD was compared to that of 10,560 non-diabetic women. Eligibility for the study was limited to women with a singleton pregnancy with spontaneous onset of delivery before 37 weeks of gestation with no history of chronic maternal illness, i.e., chronic hypertension or development of preeclampsia in the current pregnancy, and no clear indication for preterm delivery. Mean blood glucose < 105 mg dl−1 was defined as well controlled.
Results
Overall, no difference was found in the rate of sPTD in GDM (163/1,526, 10.7%) in comparison to non-GDM patients (1193/10,560, 11.3%, P = 0.2). In the GDM group, a comparison between women with and without sPTD found no difference in maternal age (28.1 ± 6 vs. 28.2 ± 6), prepregnancy BMI (28.1 ± 5 vs. 27.8 ± 6), rate of nulliparity (38 vs. 34%) or ethnicity origin. GDM patients with sPTD were characterized by higher glucose values in the OGTT and higher mean blood glucose (114 ± 16 vs. 106 ± 14, P < 0.0001). Sixty-five percent of patients with sPTD versus. 46% in the non-sPTD were in poor glycemic control (P = 0.004). Multiple logistic regressions, when the dependent variable was sPTD revealed that mean blood glucose (OR 1.94 95% CI 1.25–3.0), history of sPTD (OR 3.25 95% CI 2.1–4.8) and parity (OR 1.49 95% CI 1.05–2.2) were contributing factors.
Conclusion
The rate of sPTD in GDM is not increased in comparison to non-GDM patients, but reaching established levels of glycemic control may reduce the rate of sPTD in GDM.
Similar content being viewed by others
References
MacDorman MF, Minino AM, Strobino DM, Guyer B (2002) Annual summary of vital statistics––2001. Pediatrics 110:1037–1052
Goldenberg RL, Rouse DJ (1998) Prevention of premature birth. N Engl J Med 339:313–320
Paneth NS (1995) The problem of low birth weight. Future Child 5:19–34
McCormick MC (1985) The contribution of low birth weight to infant mortality and childhood morbidity. N Engl J Med 312:82–90
American College of Obstetricians and Gynecologists Committee on Practice Bulletins––obstetrics. perinatal care at the threshold of viability. ACOG practice bulletin no. 38. Obstet Gynecol 2002 100:617–624
Nordin NM, Wei JW, Naing NN, Symonds EM (2006) Comparison of maternal-fetal outcomes in gestational diabetes and lesser degrees of glucose intolerance. J Obstet Gynaecol Res 32(1):107–114
Yang X, Hsu-Hage B, Zhang H, Zhang C, Zhang Y (2002) Women with impaired glucose tolerance during pregnancy have significantly poor pregnancy outcomes. Diabetes Care 25:1619–1624
Rosenberg TJ, Garbers S, Lipkind H, Chiasson MA (2005) Maternal obesity and diabetes as risk factors for adverse pregnancy outcomes: differences among 4 racial/ethnic groups. Am J Public Health 95(9):1545–1551
Lao TT, Ho LF (2003) Does maternal glucose intolerance affect the length of gestation in singleton pregnancies? J Soc Gynecol Investig 10(6):366–371
Hedderson MM, Ferrara A, Sacks DA (2003) Gestational diabetes mellitus and lesser degrees of pregnancy hyperglycemia: association with increased risk of spontaneous preterm birth. Obstet Gynecol 102(4):850–856
Magee MS, Walden CE, Benedetti TJ, Knopp RH (1993) Influence of diagnostic criteria on the incidence of gestational diabetes and perinatal morbidity. JAMA 269:609–615
Sendag F, Terek MC, Itil IM, Oztekin K, Bilgin O (2001) Maternal and perinatal outcomes in women with gestational diabetes mellitus as compared to nondiabetic controls. J Reprod Med 46(12):1057–1062
Rudge MV, Calderon IM, Ramos MD, Abbade JF, Rugolo LM (2000) Perinatal outcome of pregnancies complicated by diabetes and by maternal daily hyperglycemia not related to diabetes. A retrospective 10-year analysis. Gynecol Obstet Invest 50(2):108–112
Tallarigo L, Giampietro O, Penno G, Miccoli R, Gregori G, Navalesi R (1986) Relation of glucose tolerance to complications of pregnancy in nondiabetic women. N Engl J Med 315:989–992
Bar-Hava I, Barnhard Y, Scarpelli SA, Orvieto R, Ben-Rafael, Divon MY (1997) Gestational diabetes and preterm labour: is glycaemic control a contributing factor? Eur J Obstet Gynecol Reprod Biol 73(2):111–114
Roversi GD, Pedretti E, Gargiulo M, Tronconi G (1982) Spontaneous preterm delivery in pregnant diabetics: a high risk hitherto “unrecognized”. J Perinat Med 10(5):249–253
Carpenter MW, Coustan DR (1982) Criteria for screening tests for gestational diabetes. Am J Obstet Gynecol 144:768–773
Naylor CD, Sermer M, Chen E, Sykora K (1996) Cesarean delivery in relation to birth weight and gestational glucose tolerance: Pathophysiology or practice style? Toronto trihospital gestational diabetes investigators. JAMA 275:1165–1170
Meis PJ, Klebanoff M, Thom E, Dombrowski MP, Sibai B, Moawad AH, et al (2003) Prevention of recurrent preterm delivery by 17 alpha-hydroxyprogesterone caproate. N Engl J Med 12; 348(24):2379–2385
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yogev, Y., Langer, O. Spontaneous preterm delivery and gestational diabetes: the impact of glycemic control. Arch Gynecol Obstet 276, 361–365 (2007). https://doi.org/10.1007/s00404-007-0359-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00404-007-0359-8